Less-Lethal Weapons Blind, Maim and Kill. Victims Say Enough Is Enough.
Time and again over the past two decades, peace officers have targeted demonstrators with munitions designed only to stun and stop. Protests this year in reaction to George Floyd’s death in police custody have reignited a controversy surrounding their use.
Fractured Skulls, Lost Eyes: Police Often Break Own Rules Using ‘Rubber Bullets’
Around the country, police responded to protests in the wake of George Floyd’s death by shooting “less lethal” projectiles, which can seriously hurt and kill. In a joint investigation, KHN and USA TODAY found some officers appear to have violated their department’s own rules when they fired.
A Senator From Arizona Emerges As A Pharma Favorite
Sen. Kyrsten Sinema has received almost $100,000 from drug companies in the current election cycle, a KHN analysis shows, one of the largest cash hauls in Congress. And it’s only her first term.
Drugmakers Tout COVID-19 Vaccines To Refurbish Their Public Image
Vaccines and antivirals have long been an afterthought but Johnson & Johnson and other firms are widely publicizing how they might stop COVID 19.
Telehealth Will Be Free, No Copays, They Said. But Angry Patients Are Getting Billed.
Politicians pledged to stop providers from charging for video appointments or telephone calls, but some patients are being charged $70 or $80 per virtual visit.
Furor Erupts: Billions Going To Hospitals Based On Medicare Billings, Not COVID-19
In the first round of emergency relief, some states will get more than $300,000 per COVID-19 patient, while hard-hit New York gets just $12,000 per patient.
COVID-19 Crisis Threatens Beleaguered Assisted Living Industry
The Capital Senior Living chain of assisted living communities and others like it were struggling financially before coronavirus suddenly appeared. Now their situation is really getting tough.
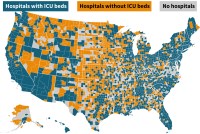
Millions Of Older Americans Live In Counties With No ICU Beds As Pandemic Intensifies
A Kaiser Health News analysis shows that counties with ICUs average one ICU bed for every 1,300 older residents, those most at risk for needing hospitalization.
VCU Health Halts 30-Year Campaign That Seized Patients’ Wages, Put Liens On Homes
The bold move by the giant hospital system will help thousands of patients in the wake of a Kaiser Health News investigation last year.
Hospital Group Mum As Members Pursue Patients With Lawsuits And Debt Collectors
The influential trade association has said little over the years as health systems, including those of its own trustees, seized patients’ incomes and assets. Now it is reevaluating.
UVA Doctors Decry Aggressive Billing Practices By Their Own Hospital
In the wake of a Kaiser Health News investigation, doctors want the University of Virginia’s health system to stop suing its patients over unpaid bills.
As UVA Scales Back Lawsuits, Pain For Past Patients Persists
Patients were thrilled last month when UVA announced it would scale back lawsuits and provide more financial assistance, but the excitement has waned.
VCU Health Will Halt Patient Lawsuits, Boost Aid In Wake Of KHN Investigation
Patients at VCU Health will no longer be taken to court and can more easily get financial assistance to pay their bills.
UVA To Cut Back On Lawsuits Against Patients
But critics say the new policy still leaves some patients exposed to lawsuits and crippling bills.
UVA Suspends Medical Lawsuits In Wake Of KHN Investigation
KHN reported this week that the University of Virginia Health System has filed 36,000 lawsuits against patients the past six years.
Virginia Governor And UVA Vow To Revamp Practice Of Suing Patients As CEO Exits
A Kaiser Health News investigation, which first appeared in The Washington Post, showed that the University of Virginia Health System has sued patients 36,000 times for more than $106 million.
‘UVA Has Ruined Us’: Health System Sues Thousands Of Patients, Seizing Paychecks And Claiming Homes
Over six years, the state institution filed 36,000 lawsuits against patients seeking a total of more than $106 million in unpaid bills, a KHN analysis finds.
Pharma Cash Rolls Into Congress To Defend An Embattled Industry
Congress has a variety of reforms in mind that could roil the drugmaking business and potentially slash prices.
Drugmakers Master Rolling Out Their Own Generics To Stifle Competition
Known as “authorized generics,” in-house spinoffs of brand-name drugs quietly undermine the competition.
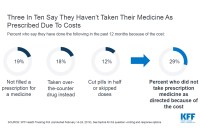
Americans Ready To Crack Down On Drug Prices That Force Some To Skip Doses
In a new poll, consumers give thumbs up to ads that display drug prices and the removal of barriers to generics, among other cost-cutting measures.