Medicare Enrollees Can Switch Coverage Now. Here’s What’s New and What to Consider.
Fall is the time when enrollees in the federal program for older people and people with certain disabilities can make changes to their health and drug plans. The decision can be complicated, but here are some key points to keep in mind.
Es el momento de revisar el plan de Medicare. Lo nuevo que hay que saber
Desde el 15 de octubre y hasta el 7 de diciembre, los afiliados al programa tradicional o a los planes de Medicare Advantage, que ofrecen aseguradoras privadas, pueden cambiar su cobertura.
Feds Hope to Cut Sepsis Deaths by Hitching Medicare Payments to Treatment Stats
A new rule sets specific treatment metrics for suspected sepsis cases in an effort to reduce deaths, but some experts say the measures could add to antibiotic overuse and need to be more flexible.
Hospitales perderán reembolsos de Medicare si no combaten mejor la mortal sepsis
La sepsis es la respuesta extrema del organismo a una infección y afecta cada año a 1,7 millones de adultos en Estados Unidos.
Timing and Cost of New Vaccines Vary by Virus and Health Insurance Status
Flu. Covid. RSV. When and how to get vaccinated against them can be confusing. Here are some of the most important things to know.
Proposed Rule Would Make Hospital Prices Even More Transparent
A Biden administration proposal would help standardize the data on prices that hospitals provide to patients, increase its usefulness to consumers, and boost enforcement. Previous rules gave hospitals too many loopholes.
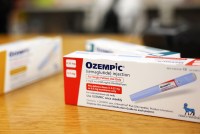
Survey: Americans Want Weight Loss Drugs Despite High Cost
A new poll reveals enthusiasm for a pricey new generation of weight loss drugs, but interest drops if users potentially have to deal with weekly injections, lack of insurance coverage, or a need to continue the medications indefinitely to avoid regaining weight.
Everything Old Is New Again? The Latest Round of Health Policy Proposals Reprises Existing Ideas
House Republican legislation promises more health insurance options but fewer protections, even as the Biden administration seeks to rein in short-term plans, which were expanded in the Trump era.
La atención primaria está cambiando: el acceso y la calidad están en juego
Una relación sólida y duradera con un médico de atención primaria —que conozca el historial del paciente y pueda vigilar nuevos problemas— se ha considerado durante mucho tiempo la base de un sistema sanitario de calidad.
Will the Doctor See You Now? The Health System’s Changing Landscape
The “front door” to the health system is changing, under pressure from increased demand, consolidation, and changing patient expectations.
A Windfall in Health Insurance Rebates? It’s Not as Crazy as It Sounds
The billion-dollar amount cited by former Sen. Al Franken, while an estimate, is likely very close to what insurers will owe this year under a provision of the Affordable Care Act that compels rebates when insurers spend too little on actual medical care.
No-Cost Preventive Services Are Now in Jeopardy. Here’s What You Need to Know.
A federal judge’s recent ruling on the Affordable Care Act is by no means the final word. Even parsing its impact is complicated. Here are key issues to watch as the case works its way through the legal system.
The Big Squeeze: More Enrollees and Smaller Networks Plague Some ACA Plans
Despite record enrollment in health insurance plans under the Affordable Care Act, some consumers who bought coverage and agents who helped them do so have had a tough start to the new year: Many say it’s hard to find an in-network doctor or hospital.
La decisión podría afectar los exámenes de detección sin copago y servicios preventivos similares que la mayoría de los estadounidenses con seguro tienen como parte de sus planes de salud.
Judge’s Decision Would Make Some No-Cost Cancer Screenings a Thing of the Past
A U.S. District Court ruling overturned the section of the Affordable Care Act that makes preventive health services — from colonoscopies to diabetes screenings and more — available at no cost to consumers.
Se acaba la era de las vacunas y las pruebas gratuitas contra covid. ¿Quién va a pagar?
Las personas podrán obtener estas vacunas a bajo costo o sin costo mientras duren los suministros del gobierno. Luego, dependerá de su seguro de salud.
Era of ‘Free’ Covid Vaccines, Test Kits, and Treatments Is Ending. Who Will Pay the Tab Now?
Insurers, employers, and taxpayers will all be affected as drug manufacturers move these products to the commercial market.
Numbers Don’t Lie. Biden Kept His Promise on Improving Obamacare.
KHN has teamed up with our partners at PolitiFact to monitor 100 key promises made by Joe Biden during the 2020 presidential campaign — including those surrounding the Affordable Care Act.
Nueva herramienta ayudaría a comparar costos de hasta 500 servicios médicos
Desde el 1 de enero, las aseguradoras y los empleadores que ofrecen planes de salud deben proporcionar calculadoras en línea para que los pacientes obtengan estimaciones detalladas de lo que deberán por una variedad de servicios y medicamentos, teniendo en cuenta sus deducibles y copagos.
Want a Clue on Health Care Costs in Advance? New Tools Take a Crack at It
Another effort to make upfront cost comparisons possible in an industry known for its opaqueness: an online tool for consumers to get some idea of what they may pay for medical care.