La última década ha sido testigo de una rápida expansión de las pruebas genéticas. Pero, ¿cuál es su real relevancia clínica?
Genetic Tests Create Treatment Opportunities and Confusion for Breast Cancer Patients
Doctors are divided on whether blanket testing of breast cancer patients is warranted, since scientists and physicians are sometimes unsure about how to interpret the results.
Algunos estados permiten que se utilicen en estudios de investigación, a veces por parte de terceros a cambio de una cuota, o que se proporcionen al personal policial que investiga un delito.
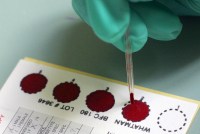
Newborns Get Routine Heel Blood Tests, but Should States Keep Those Samples?
Shortly after birth, babies are pricked in the heel so their blood can be tested for life-threatening conditions. States generally save leftover blood from those samples, and parents and privacy experts are concerned that information could be used without consent years later.
Lo que debes saber sobre Paxlovid para tratar covid, en especial, ¿debes tomarlo?
Desde que Paxlovid comenzó a estar disponible hace siete meses, ha eclipsado otras terapias disponibles para prevenir los síntomas graves de covid en pacientes de alto riesgo. Algunos médicos se apresuran a recetarlo, pero como ocurre con tanto sobre la pandemia de covid, hay controversia.
Everything You Need to Know About Paxlovid — Especially, Should You Take It?
Paxlovid has eclipsed other available therapies for preventing life-threatening covid symptoms in high-risk patients. But even as doctors praise its effectiveness, many say they have unanswered questions about prescribing the drug and want more and better data about it.
‘So Rudderless’: A Couple’s Quest for Autism Treatment for Their Son Hits Repeated Obstacles
Amparo and Victor Rios began searching for answers about their son’s development when he didn’t hit some milestones after turning 2. Three years later, they are still trying to get their insurance to pay for expensive therapy to help him.
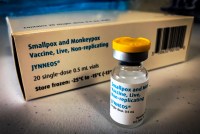
Igual que con covid, atraso en pruebas y vacunas para la viruela del simio
Los casos de la viruela del simio siguen aumentando, pero la respuesta sanitaria es lenta: escasean las pruebas y las dosis de la vacuna que puede prevenir la infección.
Vaccine and Testing Delays for Monkeypox Echo Failures in Early Covid Response
Public health officials say monkeypox is not as dangerous as covid and can be handled well with current treatments and if those at risk use caution. But the rollout of vaccines has been slow and led to angst among some at-risk people.
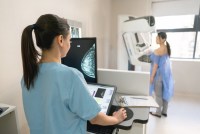
Preventive Care May Be Free, but Follow-Up Diagnostic Tests Can Bring Big Bills
Under the Affordable Care Act, insurers cannot charge consumers for various preventive services that have been recommended by experts. But if those screenings indicate more testing is needed to determine whether something is wrong, patients may be on the hook for hundreds or even thousands of dollars for diagnostic services.
Her First Colonoscopy Cost Her $0. Her Second Cost $2,185. Why?
Preventive care, like screening colonoscopies, is supposed to be free of charge to patients under the Affordable Care Act. But some hospitals haven’t gotten the memo.
Why So Slow? Legislators Take on Insurers’ Delays in Approving Prescribed Treatments
Insurers say prior authorization requirements are intended to reduce wasteful and inappropriate health care spending. But they can baffle patients waiting for approval. And doctors say that insurers have yet to follow through on commitments to improve the process.
Washington State Retools First-in-the-Nation Long-Term Care Benefit
The WA Cares Fund program, which would provide workers in the state a lifetime benefit of $36,500, was set to begin collecting money through a payroll tax in January, but it was delayed while lawmakers made adjustments to address equity problems. Now the payroll deductions will begin in July 2023, and benefits will become available in 2026.
Despite Doctors’ Concerns, Pharmacists Get More Leeway to Offer Treatment With Testing
In the battle against covid, pharmacies became a key place for consumers to seek vaccines and testing. Some states are expanding pharmacists’ work to include directly prescribing drugs for customers who seek some routine, point-of-care tests, such as those for flu or strep throat. But doctor groups oppose the move.
¿Por qué Medicare no paga por las pruebas caseras para covid?
Las mismas leyes del programa para los adultos mayores previenen que puedan comprar medicamentos de venta libre y obtener este tipo de pruebas sin una orden médica.
Why Medicare Doesn’t Pay for Rapid At-Home Covid Tests
The laws governing Medicare don’t provide coverage for self-administered diagnostic tests, which is precisely what the rapid antigen tests are and why they are an important tool for containing the pandemic.
Officials Struggle to Regulate Pop-Up Covid Testing Sites — And Warn Patients to Beware
High demand for covid screening and scarce supply have opened the door to bad actors, and officials in some states are sounding the alarm about dubious street testing operators that could put people’s personal data, their health or wallets at risk.
Funcionarios advierten sobre sitios de pruebas para covid de dudosa calidad
Lo sitios de pruebas de covid han proliferado en casi todas las grandes ciudades. Pero no todos ofrecen un servicio de calidad. Cómo detectarlos.
‘The Charges Seem Crazy’: Hospitals Impose a ‘Facility Fee’ — For a Video Visit
Facility fees, designed to help hospitals cover the high cost of staying open 24/7, have long rankled consumers. Now, some patients are assessed the fees while sitting at home for a telehealth appointment.
Muchos empleadores informaron que desde que comenzó la pandemia han realizado cambios en sus beneficios de salud mental y adicciones. La principal forma fue extender el uso de la telemedicina.