GUNNISON, Colo. — For the past eight years, my wife, Ky Hamilton, has undergone gender-affirming hormone therapy. As a transgender woman, she injects Depo-Estradiol liquid estrogen into her thigh once a week. This drug has allowed her to physically transition as a woman, and each vial, which lasts around five weeks, was completely covered by insurance.
That was until she lost her job in April 2020 and we switched to a subsidized private health insurance plan in Colorado’s Affordable Care Act marketplace. We discovered that our new insurance from Anthem doesn’t cover Depo-Estradiol and it would cost $125 out-of-pocket per vial. With both of us — and our four pets — depending heavily on Ky’s weekly $649 unemployment check, such medical expenses proved difficult. And as of Sept. 6, those unemployment checks ran out.
“I’m absolutely stressed. I don’t know what to do,” Ky said in August as we tried to find a solution.
Because of Ky’s physical transition as a transgender woman, her body doesn’t make the testosterone it once used to. So, without the medication, she would essentially go through menopause. A decline in estrogen levels can also cause transgender women to lose the physical transitions they’ve achieved, resulting in gender dysphoria, which is psychological distress from the mismatch between their biological sex and their gender identity.
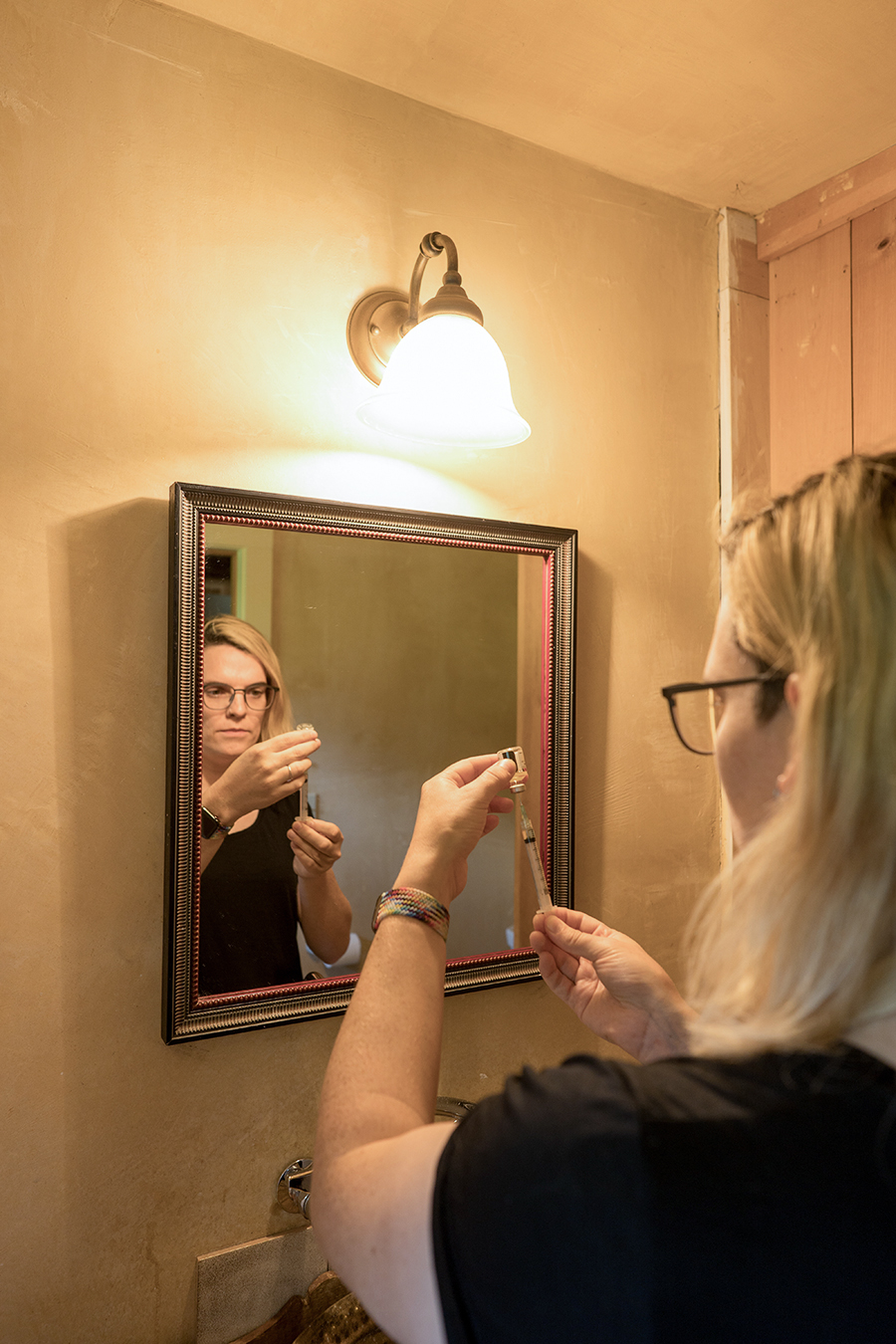
Unfortunately, Ky’s experience is shared by many other transgender Americans. The covid-19 pandemic has caused millions of people to lose their jobs and private health insurance, particularly LGBTQ adults, who reported at higher rates than non-LGBTQ adults that they lost their jobs during the crisis. Consequently, enrollment surged in ACA plans and Medicaid, the state-federal health program for low-income people. Yet many of those plans don’t fully cover gender-affirming care, partly because of conservative policies and lack of scientific research on how crucial this care is for transgender patients.
According to a survey by Out2Enroll, a national initiative to connect LGBTQ people with ACA coverage, 46% of the 1,386 silver marketplace plans polled cover all or some medically necessary treatment for gender dysphoria. However, 7% have trans-specific exclusions, 14% have some exclusions, and 33% don’t specify.
“It’s this whack-a-mole situation where plans for the most part do not have blanket exclusions, but where people are still having difficulty getting specific procedures, medications, etc., covered,” said Kellan Baker, executive director of the Whitman-Walker Institute, a nonprofit that focuses on LGBTQ research, policy and education.
Twenty-three states and Washington, D.C., include gender-affirming care in their Medicaid plans. But 10 states exclude such coverage entirely. In 2019, an estimated 152,000 transgender adults were enrolled in Medicaid, a number that has likely grown during the pandemic.
Yet even in states such as California that require their Medicaid programs to cover gender-affirming care, patients still struggle to get injectable estrogen, said Dr. Amy Weimer, an internist who founded the UCLA Gender Health Program. While California Medicaid, or Medi-Cal, covers Depo-Estradiol, doctors must request treatment authorizations to prove their patients need the drug. Weiner said those are rarely approved.
Such “prior authorizations” are an issue across Medicaid and ACA plans for medications including injectable estrogen and testosterone, which is used by transgender men, Baker said.
The lack of easy coverage may reflect the fact that injectable estrogen, which provides the high doses of the hormone needed for transgender women to physically transition, isn’t commonly used by non-trans women undergoing hormone therapy to treat menopause or other issues, Weimer said.
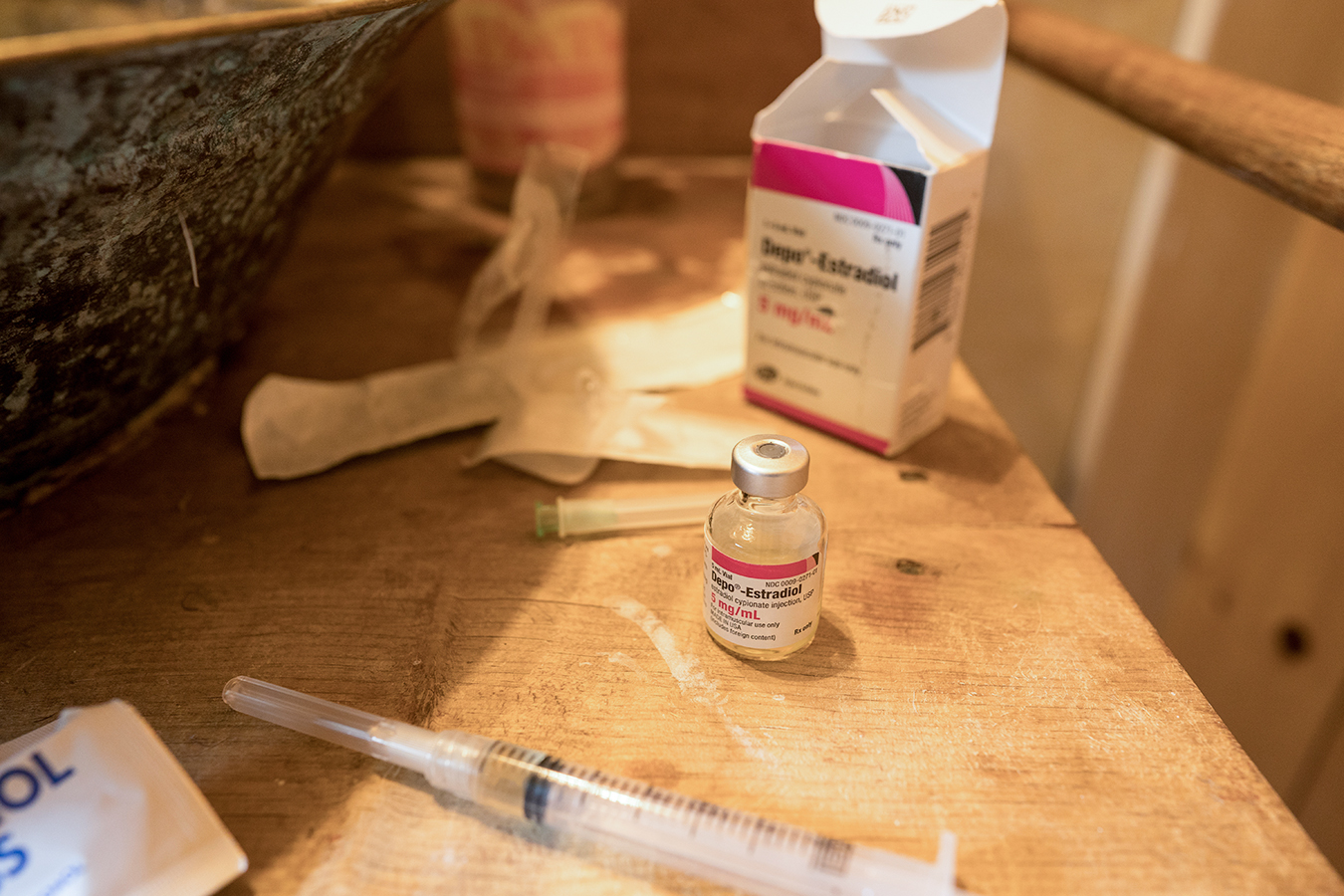
It also may be because cheaper options, including daily estrogen pills, exist, but these increase the risk of blood clots. Estrogen patches release the hormone through the skin but can cause skin reactions, and many people struggle to absorb enough estrogen, Weimer said. Consequently, many of Weimer’s patients wear up to four patches at a time, but Medi-Cal limits the number of patches patients can get monthly.
While such insurance gaps have existed for long before the pandemic, the current crisis seems to have amplified the matter, according to Weimer.
The ACA prohibits discrimination based on race, color, national origin, age, disability and sex in health programs and activities that receive federal financial assistance. The Trump administration significantly narrowed the power of that provision, including eliminating health insurance protections for transgender people.

However, in June 2020, before the Trump regulations could take effect, the Supreme Court ruled in Bostock v. Clayton County, Georgia, that employment discrimination based on sex includes sexual orientation and gender identity.
This landmark decision has served as a crucial tool to address LGBTQ discrimination in many aspects of life, including health care. As of July, for example, Alaska Medicaid can no longer exclude gender-affirming treatment after Swan Being, a transgender woman, won a class-action lawsuit that relied in part on the Bostock decision.
The Biden administration announced in May that the U.S. Department of Health and Human Services Office for Civil Rights will include gender identity and sexual orientation in its enforcement of the ACA’s anti-discrimination provision. The next month, Veterans Affairs health benefits were expanded to include gender confirmation surgery.
But for now, the pressure is still on patients like Ky to fight for their health benefits.
Anthem spokesperson Tony Felts said Depo-Estradiol is not on the list of covered drugs for its ACA plans, though many of its private employer-sponsored plans cover it.
Because we had one of those ACA plans, Ky had to be persistent. After four months of emails and phone calls — and just before unemployment ran out — Anthem finally authorized her Depo-Estradiol. That brings her out-of-pocket cost to $60 per vial for the next year. It’s still expensive for us right now, but we’ll find a way to make it work.
“The reality is that trans people are more likely to be in poverty and don’t have the time or knowledge to spend four months fighting to get their estradiol like I did,” Ky said.







