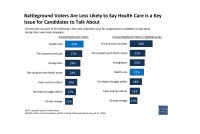
In Battleground Races, Health Care Lags As Hot-Button Issue, Poll Finds
The economy and jobs tend to eclipse health care as the top voter concern in competitive congressional and gubernatorial races.
Half Of Hospitals In Conn., Del. Hit By Medicare’s Safety Penalties
Seven states saw a third or more of their hospitals punished under the federal heath law’s campaign against hospital-acquired conditions.
Care Suffers As More Nursing Homes Feed Money Into Corporate Webs
Increasingly, owners of nursing homes outsource services to companies in which they also have financial interest or control. That allows the nursing homes to claim to be in the red while owners reap hidden profits.
Trump Administration Relaxes Financial Penalties Against Nursing Homes
Medicare is discouraging regional offices from levying fines for “one-time mistakes” or from using daily fines that seek to put pressure on nursing homes to make changes.
Infection Lapses Rampant In Nursing Homes But Punishment Is Rare
A Kaiser Health News analysis of federal inspection records shows that nursing home inspectors labeled mistakes in infection control as serious for only 161 of the 12,056 homes they have cited since 2014.
751 Hospitals Hit With Safety Penalties For 2018: Data Table
The federal government has cut payments to hospitals with high rates of patient injuries this year. Those hospitals will lose 1 percent of Medicare payments over the federal fiscal year, which runs from October through September. Maryland hospitals are exempted from penalties because that state has a separate payment arrangement with Medicare. Below are the […]
Medicare Penalizes Group Of 751 Hospitals For Patient Injuries
Each hospital will have its payments reduced by 1 percent for the year.
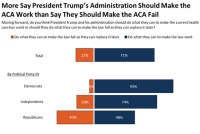
While Trump Moves To Dismantle Health Law, Public Favors Repair
Nearly three-quarters of Americans would like to see the administration focus on efforts on making the Affordable Care Act work, rather than trying to make it fail.
Why Glaring Quality Gaps Among Nursing Homes Are Likely To Grow If Medicaid Is Cut
Medicaid covers about two-thirds of nursing home residents, but it pays less than other types of insurance.
Nursing Home Disaster Plans Often Faulted As ‘Paper Tigers’
Too often enforcement of rules for dealing with crisis is lax, advocates for nursing home residents say.
Under Trump, Hospitals Face Same Penalties Embraced By Obama
Federal records show that 2,573 hospitals around the country will have their Medicare payments reduced because they have too many patients readmitted.
Opposition To GOP Repeal Bill Inches Up And Intensifies
Six in 10 Americans say they do not approve of the Senate Republicans’ plan to replace Obamacare, according to a poll by the Kaiser Family Foundation.
Nursing Homes Move Into The Insurance Business
Although proponents say the policies offered by nursing homes are more attuned to patients, some report frustrations when trying to dispute care decisions.
Millions Of Kids Fall Outside Senate Plan To Shield Disabled From Medicaid Cuts
The Republican plan to replace Obamacare would reduce federal funding for Medicaid, but senators want to keep current funding levels for children who are blind or have other disabilities. Their proposal, however, would not apply to the majority of those kids.
Half The Time, Nursing Homes Scrutinized On Safety By Medicare Are Still Treacherous
Of the 528 nursing homes that graduated from special focus status before 2014 and are still operating, more than half — 52 percent — have harmed patients or operated in a way that put patients in serious jeopardy within the past three years, a KHN analysis finds.
Senate And House Take Different Plans To Scrap Individual Mandate
The Republicans’ penalty would affect people buying insurance who had a lapse in coverage of more than 63 days over a year.
In The End, Even The Middle Class Would Feel GOP Squeeze On Nursing Home Care
Medicaid pays for two-thirds of nursing home residents, but some recipients don’t even know they’re on it.
Americans Not Sold On Cost And Coverage Claims In GOP’s Health Bill
Nearly half of the people in this month’s Kaiser Family Foundation tracking poll believe the Republican legislation will increase the number of uninsured Americans and increase coverage costs.
GOP Fix To Insurance Markets Could Spike Premiums For Older Customers
As Republicans consider how to bring down costs for younger people, lawmakers may relax or eliminate the restrictions on how much more insurers can charge older consumers.
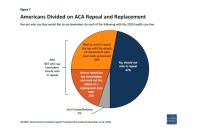
Only 20 Percent Of Americans Support Health Law Repeal Without Replacement Plan
A new poll shows that GOP lawmakers’ strategy lacks widespread support and most people are more concerned that health care is affordable and available.