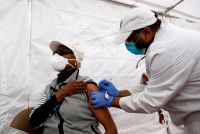
Rural Hospital Remains Entrenched in Covid ‘War’ Even Amid Vaccine Rollout
Louisiana’s St. James Parish Hospital thought the vaccine would mean the end of its long covid fight. Then the ICU beds surrounding them ran out.
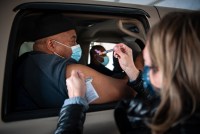
As Vaccine Rollout Expands, Black Americans Still Left Behind
Covid vaccines are reaching more Americans, but Black residents are being vaccinated at dramatically lower rates in the 23 states where data is publicly available. The Centers for Disease Control and Prevention plans to release national data next week.
Black Americans Are Getting Vaccinated at Lower Rates Than White Americans
Black Americans are receiving covid vaccines at a much lower rate than their white peers due to a combination of mistrust and access issues, leaving them behind in the mission to vaccinate the nation’s population.
CVS and Walgreens Under Fire for Slow Pace of Vaccination in Nursing Homes
A federal program that sends retail pharmacists into nursing homes to vaccinate residents and workers has been hindered by bureaucratic hurdles and scheduling woes.
In Los Angeles and Beyond, Oxygen Is the Latest Covid Bottleneck
The oxygen delivery infrastructure is crumbling under pressure in Los Angeles and other covid hot spots, jeopardizing patients’ access to precious air and limiting hospital turnover.
Inside the First Chaotic Days of the Effort to Vaccinate America
After missteps in Washington, each state and county is left to juggle where to send vaccines first and how to get them to each nursing home, hospital local health department and even school.
Ataques a la salud pública generan éxodo de funcionarios en medio de la pandemia
Estas partidas son una erosión adicional a la ya frágil infraestructura de salud pública del país, antes de la campaña de vacunación más grande en la historia de los Estados Unidos.
Pandemic Backlash Jeopardizes Public Health Powers, Leaders
At least 181 public health leaders in 38 states have resigned, retired or been fired amid the turmoil of the pandemic. The departures come as backlash against public health is rising with threats to officials’ personal safety and legislative and legal efforts to strip their governmental public health powers.
Nursing Homes Still See Dangerously Long Waits for COVID Test Results
The Trump administration hailed rapid tests as the way to halt COVID’s spread in nursing homes. A KHN analysis of federal data shows they’re not being used, as questions linger about accuracy and best practices.
Why State Mask Stockpiling Orders Are Hurting Nursing Homes, Small Providers
More than eight months into the pandemic, stockpiling of masks and other protective equipment by wealthy hospital systems is straining nursing homes and smaller providers who also need precious protective gear to keep front-line workers safe from COVID-19.
COVID Takes Challenge of Tracking Infectious College Students to New Level
Amid a surge of college coronavirus cases, some local and state health departments have been scrambling to properly trace contacts and assign cases across state and county lines.
Stigma Against D.O.s Had Been Dissipating Until Trump’s Doctor Took the Spotlight
Two types of licensed physicians exist in this country — M.D.s and D.O.s. Here’s what you need to know about the differences.
Inside the Flawed White House Testing Scheme That Did Not Protect Trump
President Trump relied heavily on testing as protection against COVID exposure, eschewing masks and social distancing.
El sistema de pruebas para COVID de la Casa Blanca no protegió al presidente
El diagnóstico de COVID-19 del presidente Donald Trump está generando nuevas preguntas sobre la estrategia de la Casa Blanca para realizar pruebas y contener la propagación del virus.
The Mask Hypocrisy: How COVID Memos Contradict the White House’s Public Face
When in public, President Donald Trump and Vice President Mike Pence join crowded rallies where many do not wear masks. Behind the scenes, the White House is recommending states adopt mask mandates and even fines — leaving it up to local officials to handle the consequences.
Lack of Antigen Test Reporting Leaves Country ‘Blind to the Pandemic’
A KHN review found more than 20 states either don’t count or have incomplete data on the use of COVID-19 antigen tests, leaving the public in the dark about the true scope of the pandemic.
La política frena el flujo de fondos a las agencias para detener la pandemia
Desde que comenzó la pandemia, el Congreso ha reservado miles de millones para aliviar la crisis. Pero parte de ese dinero no se ha distribuido, o gastado, apropiadamente.
Politics Slows Flow of US Pandemic Relief Funds to Public Health Agencies
Congress has allocated trillions of dollars to ease the coronavirus crisis. A joint KHN and AP investigation finds that many communities with big outbreaks have spent little of that federal money on local public health departments for work such as testing and contact tracing.
Public Health Officials Are Quitting or Getting Fired in Throes of Pandemic
A review by KHN and the Associated Press finds at least 49 state and local public health leaders have resigned, retired or been fired since April across 23 states. One of the latest departures came Sunday, when California’s public health director was ousted.
KHN’s Midwest correspondent Lauren Weber drills through the vital health care policy stories of the week, so you don’t have to.