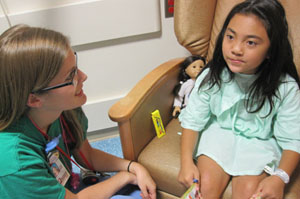
Yoselyn Gaitan, an eight-year-old with a shy smile, sits quietly in an exam room at Children’s National Medical Center in Washington D.C., wearing a tiny hospital gown. She looks a little uneasy as she waits to be brought back to the operating room for the final surgery on her cleft palate.
Kelly Schraf spots her through the curtain, and tiptoes into her room.
Schraf is a child life specialist, a type of health care provider whose job is to help sick children and their families navigate difficult medical situations emotionally and psychologically while in the hospital. They do it largely through play—the basis of how a child learns and grows.
Schraf introduces herself to Yoselyn and her mother, and explains to them why she’s there: “It’s my job at the hospital to make it easier for you to be here and make it more fun.” At the word “fun,” Yoselyn begins to look a little more relaxed.
One of the scariest parts of surgery for a child is the anesthesia mask, so Schraf brings Yoselyn the mask in advance, along with some sparkly stickers for decoration.
“The doctor is going to put sleepy air through this hole, and sometimes the sleepy air is stinky. Another little girl told me it smells like dirty socks,” Schraf explains. “So what I have are special smells to put inside to make it smell good. I have bubblegum, strawberry and cotton candy.”
Yoselyn picks bubblegum and applies a generous layer of it to her mask. By the end of their visit, she’s grinning, and so is Schraf.
Schraf is straight out of college, followed by a mandatory 480-hour child life internship. She says she’s already found her perfect job. Her favorite part, she explains, “is knowing that I made a difference in a child or a family’s life. Seeing them so stressed because they’ve gone through so much that a child shouldn’t have to experience, and knowing that I can work with the hospital team and make their stay better.”
Pediatric ear, nose and throat surgeon Rahul Shah says the doctors in the outpatient surgery unit are as grateful for child life specialists like Schraf as the patients are. “It’s really profound when you hear some of the most old school physicians or surgeons asking for something you would consider warm and fuzzy,” he says. But those doctors insist that they need child life specialists, largely because they make the unit more productive.
When the child life specialists aren’t available, Shah explains, “It’s hard. You’re pulling [children] sometimes away from the parents. The parents are upset. The child is upset. It heightens their anxiety. You bring them back to the operating room, and it’s a lot harder to put them back to sleep. It’s a lot harder to give them an IV.”
Even if each visit saves only four minutes of the surgical team’s time, he says, it can allow that team to accomplish an extra surgery each day.
There are about 4,000 child life specialists in the country. Most of them work in the acute units with the very sickest children. Liz Anderson, who, like Schraf, is bubbly, blond and 24, works in the oncology unit, where children often spend months at a time.
“I get to know them very, very well,” Anderson says.
She’s been working with nine-year-old Owen O’Hara for several weeks. He sits in his pajamas in an isolation room, a feeding tube in his nose. It’s been less than a week since his bone marrow transplant, which his doctors hope will cure his leukemia; his immune system still too vulnerable to be in the unit’s playroom with the other kids. So yesterday, Anderson brought him a brand new set of Legos to play with.
“We’re building an alien spaceship,” Owen explains, pointing out the cockpit and several green plastic men with tentacles.
Owen’s mom Jackie O’Hara says child life specialists have made a huge difference in helping Owen understand what’s happening to him, often explaining difficult medical concepts in child-friendly words. “Medical terminology is a different language altogether and it’s scary,” O’Hara explains. “They’re able to take the scariness out of it.”
But like all things in health care, child life programs come at a price. The 16 child life specialists at Children’s National Medical Center cost about $800,000 a year, which gets added to the hospital’s overhead, like electricity or maintenance, which gets passed on to patients and insurers.
Mark Wietecha, president and CEO of the Children’s Hospital Association, says the cost is “greatly worth it.” Child life specialists can minimize the trauma caused by a hospital stay – and that can pay dividends far into the future for a sick child, he said.
“It’s really almost an insignificant amount of money on our national expenditure to let the sickest kids have some opportunity to a life and be re-assimilated,” Wietecha said.
O’Hara couldn’t agree more. The child life program, she says, is “like having a little bit of a normal life in the middle of something that’s not normal.”