Charlottesville, Virginia – There have been lots of parties this year at the University of Virginia School of Nursing, but Dean Dorrie Fontaine is in no mood to celebrate. So far, eleven professors have retired, a full 25 percent of the whole faculty. The health law is predicted to boost demand for nurses to take care of the newly-insured, especially in primary care. “I need faculty to teach the practitioners that are going to take care of these uninsured,” she says.
In many places, there is already a nursing shortage and it’s expected to get worse. Polly Bednash, head of the American Association of Colleges of Nursing, says that while nurses – the oldest group of workers in the country – kept working during the recession, now that the economy is improving, “they are going to leave in droves.”
But turning out more nurses doesn’t seem likely. In the last year, nursing schools turned away more than 76,000 qualified applicants because there weren’t enough professors.
Finding more professors will be difficult, because faculty members usually need a Ph.D. Of three million nurses in this country, fewer than one percent have doctorates and that’s not changing. Associate Professor Emily Drake notes most nurses are unwilling to go for more years in school. “After you finish your degree,” she says, “what we want to do is take care of patients.”
Pay and lifestyle are also problems. Nurses with a master’s degree and special training can be certified as nurse practitioners – paid $120,000 a year or more. After ten years as a professor, Drake earns about $75,000. And, by the time most nurses consider a Ph.D., Dean Fontaine worries that their lives are complicated with a job, financial obligations and children.
Diversity in the teacher population is missing, too, according to Fontaine: “We want to have our faculty and students match the population we serve, so we do not have enough Hispanic nurses or faculty, as well as African-Americans and other minorities – and men!” Men make up just 10 percent of the nursing workforce, and Fontaine hopes the field can draw more them to get PhDs and step into the classroom.
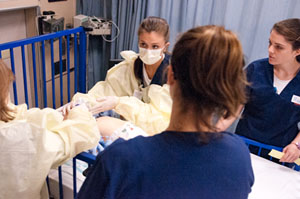
Prof. Emily Drake says one solution – just increasing class size – won’t work because much of the training for nurses is hands-on: “By law, for each additional ten students we take, we need another clinical faculty member to supervise them in the hospital.”
So schools are looking for other ways to teach, according to Polly Bednash. “Faculty are getting more and more creative about how they prepare students. They bring in other clinicians to the educational experience – having pharmacists, for instance, be involved in teaching the pharmacotherapeutics.”
Schools also using technology – simulators and computer-based lessons – to supplement classroom and lab experience. Nationwide, nearly 8 percent of nursing school jobs – about 1,200 — are vacant, so the American Association of Colleges of Nursing is lobbying for more state, federal and foundation money to train PhDs. And they’re urging their most promising students to get the advanced degree before they acquire a family and a mortgage.
This story is part of a partnership with Virginia Public Radio, NPR and Kaiser Heath News.