Latest KFF Health News Stories
‘When It Starts Getting Into Your Local Hospital, It Becomes Real’
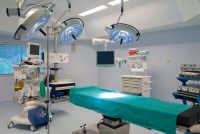
Located about 45 minutes from New Orleans in one of the hardest-hit counties nationally, the 25-bed rural St. James Parish Hospital has hunkered down as staffers became infected, patient intake numbers have doubled, and intubations have skyrocketed. This is what it looks like inside a rural hospital when COVID-19 hits.
Second Time Around? Health Care Issues Trump Might Tackle If Reelected
KHN’s Julie Rovner examines what health care issues the administration might encounter if President Donald Trump wins in November.
More Than 5,000 Surgery Centers Can Now Serve As Makeshift Hospitals During COVID-19 Crisis
Under pressure, the federal government announced it will let surgery centers, hotels and even college dorms serve as hospitals to treat an overflow of patients.
COVID-19 Bonanza: Stimulus Hands Health Industry Billions Not Directly Related To Pandemic
Congress retreats on long-planned cost cuts to benefit the health care industry with a grab bag full of incentives.
Physicians Fear For Their Families As They Battle Coronavirus With Too Little Armor
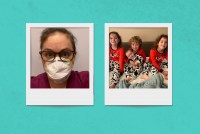
Doctors sent an impassioned, desperate letter to Congress describing the lack of protective equipment across the country — from masks to respirators to gowns to goggles. They’re using equipment from construction sites and home-repair stores or wearing the same mask from patient to patient. And they worry about what exposure without sufficient protection means for them and their families.
Under Financial Strain, Community Health Centers Ramp Up Coronavirus Response
Many of the nation’s safety-net clinics for low-income patients are having to turn their model of care upside down overnight to deal with the realities of the pandemic — a challenge both financially and logistically. Federal funding is on the way.
Are Vital Home Health Workers Now A Safety Threat?
Hundreds of thousands of health care workers go into homes to provide important services for seniors and disabled people. But with the rising concerns about the danger of the coronavirus pandemic, especially for older people, these health workers could be endangering their patients and themselves.
With Medical Safety Gear Scarce, The Public Is Stepping Up. Here’s Help On Ways To Help.
If you or your company have useful supplies and want to donate them, here are some answers to questions you might be asking.
Abortion-Rights Supporters Fear Loss Of Access If Adventist Saves Hospital
As community hospitals struggle, they often turn to large religious-based hospital groups to bail them out. But that can limit the types of services they offer, especially reproductive health treatment such as abortion.
How Fast Can A New Internet Standard For Sharing Patient Data Catch Fire?
The web-based standard FHIR — pronounced “fire” — could hasten the day when we can view our full medical histories on a smartphone screen. Tech giants are hungry for a piece of the pie, but obstacles remain.
Hospital Known For Glamorous Patients Opens New Doors To Its Neediest
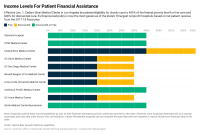
For years, Cedars-Sinai Medical Center in Los Angeles, one of California’s largest nonprofit hospitals, has been spending less on charity care than other nonprofit hospitals in the state. Now it is expanding eligibility for free and discounted medical care.
Hospital Group Mum As Members Pursue Patients With Lawsuits And Debt Collectors
The influential trade association has said little over the years as health systems, including those of its own trustees, seized patients’ incomes and assets. Now it is reevaluating.
California AG Details ‘Historic’ Settlement Agreement In Sutter Health Antitrust Case
Sutter Health will pay $575 million to settle a high-profile antitrust case filed by California’s attorney general. In addition, it has agreed to end a host of practices that the state alleged unfairly stifled competition.
Promising Greater Safety, A Tiny Widget Creates Chaos For Tube Feeders
A standard connector for feeding tubes was supposed to improve patient safety by preventing accidental misconnections to equipment used for IVs or other purposes. But critics say the design instead could keep patients from real food and inadvertently creates a host of new risks, including for vulnerable premature infants.
Must-Reads Of The Week From Brianna Labuskes
Newsletter editor Brianna Labuskes wades through hundreds of health care policy stories each week, so you don’t have to.
Medical Device Failures Brought To Light Now Bolster Lawsuits And Research
Millions of injuries and malfunctions once funneled into a hidden Food and Drug Administration database are now available.
‘I Feel Like I’m In Jail’: Hospital Alarms Torment Patients
As alarms proliferate, hospitals are working to sort through the cacophony that can overwhelm staff and cause them to overlook real signs of harm.
UVA Doctors Decry Aggressive Billing Practices By Their Own Hospital
In the wake of a Kaiser Health News investigation, doctors want the University of Virginia’s health system to stop suing its patients over unpaid bills.
No Safety Switch: How Lax Oversight Of Electronic Health Records Puts Patients At Risk
Special interests and congressional inaction blocked efforts to track the safety of electronic medical records, leaving patients at risk.
Startup Seeks To Hold Doctors, Hospitals Accountable On Patient Record Requests
Despite laws requiring that health care providers hand over copies of patient records in a timely fashion, many people have trouble getting theirs. Ciitizen, a Palo Alto, Calif., company that helps cancer patients with the task, recently published a scorecard that rates hospitals, doctors and clinics on their compliance with records requests.