Latest KFF Health News Stories
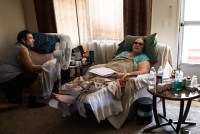
California Patients Fear Fallout From Third Dialysis Ballot Measure
Californians are facing the third statewide dialysis initiative in five years. The dialysis industry is spending tens of millions of dollars to defeat Proposition 29 and is running ads saying the measure would force clinics to close — a message that appears to be resonating with patients.
Las clínicas de salud sexual luchan sin medios contra la viruela del simio
Las clínicas que tratan las enfermedades de transmisión sexual —que ya se enfrentaban a un aumento explosivo de enfermedades como la sífilis y la gonorrea— se encuentran ahora en la primera línea de la lucha para controlar el brote de viruela del simio, que crece rápidamente.
Fighting Monkeypox, Sexual Health Clinics Are Underfunded and Ill-Equipped
Sexual health clinics are scrambling to properly track, test, and treat hundreds of monkeypox patients. So far, it isn’t going well.
‘It’s Not a Haven’: With Limited Capacity for Abortion Care, Minnesota Clinics Brace for Influx
In Minnesota, where abortion rights are protected by the state’s constitution, legal doesn’t necessarily mean accessible. The state has just eight clinics that provide abortions, and both providers and advocates say resources available aren’t enough to meet demand as nearby states reduce abortion access.
KHN’s ‘What the Health?’: Taking a Shot at Gun Control
The U.S. House passed a package of bills seeking to keep some guns out of the hands of children and teenagers, but its fate in the Senate remains a big question mark. Meanwhile, the Federal Trade Commission takes on drug and hospital prices. Alice Miranda Ollstein of Politico, Anna Edney of Bloomberg News, and Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico join KHN’s Julie Rovner to discuss these issues and more. Also this week, Rovner interviews Cori Uccello of the American Academy of Actuaries about the most recent report from Medicare’s trustees board.
With its latest venture into primary care clinics, is America’s leading organization for seniors selling its trusted seal of approval?
KHN’s ‘What the Health?’: Washington’s Slow Churn
Stemming gun violence is back on the legislative agenda following three mass shootings in less than a month, but it’s hard to predict success when so many previous efforts have failed. Meanwhile, lawmakers must soon decide if they will extend current premium subsidies for those buying health insurance under the Affordable Care Act, and the Biden administration acts, belatedly, on Medicare premiums. Margot Sanger-Katz of the New York Times, Sandhya Raman of CQ Roll Call, and Rachel Cohrs of Stat News join KHN’s Julie Rovner to discuss these issues and more. Also this week, Rovner interviews KHN’s Michelle Andrews, who reported and wrote the latest KHN-NPR “Bill of the Month” episode about a too-common problem: denial of no-cost preventive care for a colonoscopy under the Affordable Care Act.
Clínica de abortos en la frontera de Texas enfrenta desafíos legales y culturales únicos
La ley sobre el aborto de Texas, una de las más restrictivas del país, ha puesto a mujeres que viven cerca de la frontera ante dilemas de salud críticos.
Abortion Clinic on Texas-Mexico Border Faces Unique Legal and Cultural Challenges
Just as Texas has tightened its laws surrounding abortion, Mexico has gone the opposite direction, compelling people to seek potentially less-safe procedures south of the border.
In May 2021, Lags Medical Centers, one of California’s largest chains of pain clinics, abruptly closed its doors amid a cloaked state investigation. Nine months later, patients are still in the dark about what happened with their care and to their bodies.
‘Heart’ of Little Shell: Newest Federally Recognized Tribe to Open First Clinic
The Little Shell Tribe of Chippewa Indians of Montana plans to open the nation’s newest Indian Health Service clinic in Great Falls on Jan. 31 — marking the first time the tribe will have its culture reflected in health care offerings.
Clinics Say State’s New Medicaid Drug Program Will Force Them to Cut Services
On Jan. 1, California started buying prescription drugs for its nearly 14 million Medicaid enrollees, a responsibility that had primarily been held by managed-care insurance plans. State officials estimate California will save hundreds of millions of dollars by flexing its purchasing power, but some health clinics expect to lose money.
KHN’s ‘What the Health?’: Roe v. Wade on the Rocks
A Supreme Court majority appears ready to overturn nearly 50 years of abortion rights, at least judging by the latest round of oral arguments before the justices. And a new covid variant, omicron, gains attention as it spreads around the world. Alice Miranda Ollstein of Politico, Sarah Karlin-Smith of the Pink Sheet and Shefali Luthra of The 19th join KHN’s Julie Rovner to discuss these issues and more. Also this week, Rovner interviews Blake Farmer of Nashville Public Radio about the latest KHN-NPR “Bill of the Month” episode.
California Plans for a Post-Roe World as Abortion Access Shrinks Elsewhere
While other states dramatically restrict abortion and the conservative-leaning U.S. Supreme Court weighs Roe v. Wade, California is preparing to absorb the country’s abortion patients.
Community Clinics Shouldered Much of the Vaccine Rollout. Many Haven’t Been Paid.
Federally qualified health centers from California to Michigan are mired in a bureaucratic mess over how they should be paid under Medicaid for each dose of covid vaccine given. In California alone, clinics await reimbursement for at least 1 million shots, causing a “massive cash flow problem.”
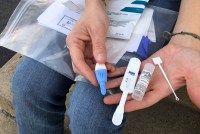
Change to Gilead Assistance Program Threatens PrEP Access, HIV Advocates Say
Safety-net clinics especially are bracing for how the drugmaker’s policy shift could reduce their budgets and hamstring their ability to provide care to an at-risk population.
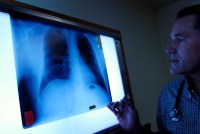
In Poisoned Montana Town, Warren Buffett-Owned Railroad Accuses Clinic of Medicare Fraud
BNSF Railway accuses the Center for Asbestos Related Disease of Medicare fraud by misdiagnosing and overtreating asbestos-caused illnesses, which the health clinic calls a cynical attempt by the company to limit its own liability.
Doctors Scramble to Understand Long Covid, but Causes and Prognosis Are Elusive
Medical experts are struggling to define or explain the lingering, debilitating symptoms some covid patients experience. Part of the problem is the wide range of symptoms, but doctors say getting a better understanding will mean tracking patients and their outcomes and establishing clinical trials.
Peligran avances contra el VIH por la lucha contra covid, en especial en el sur del país
El impacto exacto de una pandemia sobre la otra todavía está por evaluarse, pero los datos preliminares inquietan a expertos que hasta hace poco celebraban los enormes avances en el tratamiento del VIH.
Strides Against HIV/AIDS Falter, Especially in the South, as Nation Battles Covid
Public health resources have shifted from one pandemic to the other, and experts fear steep declines in testing and diagnoses mean more people will contract HIV and die of AIDS.