Rural Seniors Benefit From Pandemic-Driven Remote Fitness Boom
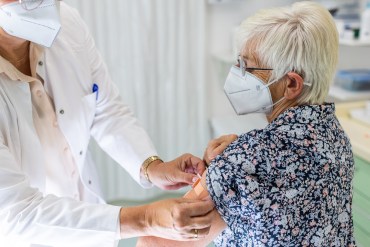
When the pandemic began, senior service agencies hustled to rework health classes to include virtual options for older adults. Now that isolation has ended, virtual classes remain. For seniors in rural areas, those classes have broadened access to supervised physical activity.
Much of the CDC Is Working Remotely. That Could Make Changing the Agency Difficult.
Like many U.S. workplaces, the Centers for Disease Control and Prevention went remote during the pandemic. Most of the agency’s staff members haven’t returned to the office full time, raising concerns about the CDC’s ability to reform itself after recent stumbles.
Blackfeet Nation Challenges Montana Ban on Vaccine Mandates as Infringement on Sovereignty
The Montana tribe has entered a legal fight over whether the state has the right to enforce a prohibition of vaccine mandates on its reservation.
Watch: Meet the Latest Fact-Checker — Your Doctor
KHN’s Mary Agnes Carey talks with American Medical Association President Dr. Jack Resneck Jr. about how misinformation affects doctors and their daily efforts to treat patients.
Journalists Dig In on the Fiscal Health of the Nation and Hospital Closures in Rural Missouri
KHN and California Healthline staff made the rounds on national and local media this week to discuss their stories. Here’s a collection of their appearances.
KHN’s ‘What the Health?’: On Government Spending, Congress Decides Not to Decide
Congress has once again decided not to decide how to fund the federal government in time for the start of the fiscal year, racing toward a midnight Sept. 30 deadline to pass a stopgap bill that would keep the lights on for two more months. However, it does appear the FDA’s program that gets drugmakers to help fund some of the agency’s review staff will be renewed in time to stop pink slips from being sent. Alice Miranda Ollstein of Politico, Rachel Cohrs of Stat, and Victoria Knight of Axios join KHN’s Julie Rovner to discuss these topics and more. Also this week, Rovner interviews filmmaker Cynthia Lowen, whose new documentary, “Battleground,” explores how anti-abortion forces played the long game to overturn Roe v. Wade.
Journalists Dissect Medical Coding and Parse the President’s Words
KHN and California Healthline staff made the rounds on national and local media this week to discuss their stories. Here’s a collection of their appearances.
Readers and Tweeters Place Value on Community Services and Life-Sustaining Care
KHN gives readers a chance to comment on a recent batch of stories.
¿Ponerse el refuerzo ahora o esperar? Muchos se preguntan cómo navegar la próxima ola de covid
Aproximadamente el 70% de los estadounidenses de 50 años o más que recibieron una primera vacuna de refuerzo contra covid, y casi la misma cantidad de personas de 65 años o más, no han recibido un segundo, según datos de los CDC.
Boost Now or Wait? Many Wonder How Best to Ride Out Covid’s Next Wave
As the country faces a rise in new infections driven by the omicron BA.5 subvariant of the coronavirus, about 70% of people 50 and older who got a first covid-19 booster shot haven’t received the recommended second one, according to the Centers for Disease Control and Prevention. Many undervaccinated Americans have lost interest, and others aren’t sure whether to get boosted again now or wait for vaccines reformulated to target newer strains of the virus.
A Free-for-All From Readers and Tweeters, From Medical Debt to Homelessness
KHN gives readers a chance to comment on a recent batch of stories.
‘An Arm and a Leg’: One ER Doctor Grapples With the Inequities of American Health Care
This episode is an interview with Dr. Thomas Fisher, author of “The Emergency: A Year of Healing and Heartbreak in a Chicago ER.”
Feds Want a Policy That Advocates Say Would Let Hospitals Off the Hook for Covid-Era Lapses
The pandemic disrupted all sense of normalcy for U.S. hospitals, so federal officials are proposing to pause financial penalties against the facilities and to block public access to key hospital safety data — such as the frequency of falls and sepsis — because of concerns that the data isn’t accurate enough. But consumer advocates are furious about the proposal.
‘My Body, My Choice’: How Vaccine Foes Co-Opted the Abortion Rallying Cry
Anti-vaccine advocates discovered a catchy, succinct, and potent slogan. Its unlikely source: the abortion rights movement.
Cómo Pfizer le ganó a la pandemia, alcanzando influencia y ganancias descomunales
Su éxito en el desarrollo de medicamentos contra covid le ha dado a la farmacéutica un peso inusual en la determinación de la política de salud de Estados Unidos. Algo que preocupa a expertos.
How Pfizer Won the Pandemic, Reaping Outsize Profit and Influence
The drugmaker has the best-selling vaccine to prevent covid and the most effective drug to treat it. Its success has overshadowed the government’s covid-fighting strategy.
KHN’s ‘What the Health?’: A World Without ‘Roe’
The Supreme Court’s decision overturning Roe v. Wade has created far more questions than it has answered about the continued legality and availability of abortion, as both abortion rights supporters and anti-abortion activists scramble to put their marks on policy. Meanwhile, Congress completes work on its gun bill and the FDA takes up the problem of the next covid-19 booster. Margot Sanger-Katz of The New York Times, Sarah Karlin-Smith of the Pink Sheet, and Victoria Knight of KHN join KHN’s Julie Rovner to discuss these issues and more. Also this week, Rovner interviews KHN’s Angela Hart, who reported and wrote the latest KHN-NPR “Bill of the Month” episode about two identical eye surgeries with very different price tags.
Readers and Tweeters Weigh In on Medical Debt, the Obesity Epidemic, and Opioid Battles
KHN gives readers a chance to comment on a recent batch of stories.
KHN’s ‘What the Health?’: Closing In on Covid Vaccines for ‘The Littles’
The wait is nearly over for parents of kids under 5 as a key advisory committee to the FDA recommends authorizing a covid-19 vaccine for the youngest children. Meanwhile, Congress is struggling to fill in the details of its gun control compromise, and, as the Supreme Court prepares to throw the question of abortion legality back to the states, the number of abortions has been rising. Shefali Luthra of The 19th, Sarah Karlin-Smith of the Pink Sheet, and Sandhya Raman of CQ Roll Call join KHN’s Julie Rovner to discuss these issues and more. Plus, for extra credit, the panelists recommend their favorite health policy stories of the week they think you should read, too.
At a Bay Area ‘Test-to-Treat’ Site, Few Takers for Free Antivirals
In carrying out the federal covid-19 “test-to-treat” initiative, California is targeting the uninsured by outfitting 138 testing sites with screenings for free antiviral drugs. But as of mid-June, fewer than 800 people had been prescribed the medicines. And two-thirds of those undergoing screenings are insured.