Latest KFF Health News Stories
Doing More Harm Than Good? Epidemic of Screening Burdens Nation’s Older Patients
Patients are often aggressively screened for cancer, even if they won’t live long enough to benefit.
These Annual Checkups Help Seniors Not Only Survive But Thrive
Seniors are living longer and defying predictions of cognitive and functional decline. Wellness coaches guide them in setting goals for the year — whether physical, social, intellectual or spiritual.
Straight From The Patient’s Mouth: Videos Can Clearly State Your End-Of-Life Wishes
Video advance directives enable people to speak directly to their families and physicians about their wishes for end-of-life care.
This Thanksgiving, Carve Out Time To Talk About End-Of-Life Wishes
A vital tradition is gaining steam as more families use the holiday gathering to discuss and document advance-care plans.
Hospice Workers Who Care For The Dying Don’t Plan Ahead Themselves
Fewer than half of health care workers at a nonprofit Florida hospice had completed advance directives for end-of-life care.
New ‘Instructions’ Could Let Dementia Patients Refuse Spoon-Feeding
Patients with Alzheimer’s disease and other dementias can say in advance if and when they want caregivers to stop offering food and fluids by hand.
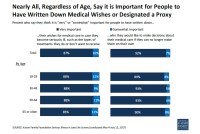
Poll: Americans Avoid Planning For Serious Illness
A majority of Americans say it’s important to write down their medical wishes in case of serious illness, but only a third have done so.
‘No One Is Coming’: Hospice Patients Abandoned At Death’s Door
U.S. hospice agencies promise to be available around-the-clock to help patients dying in their homes. But a Kaiser Health News investigation shows that in an alarming number of cases, that promise is broken.
El doloroso costado positivo del marketing médico
Una paciente con cáncer de seno terminal asegura que los comerciales solo promueven curas milagrosas y pacientes felices. La realidad es distinta, asegura.
The Painful Side Of Positive Health Care Marketing
Advertising for hospitals, unlike pharmaceutical companies, doesn’t have to be backed up by data or facts. Cheerful messages of hope can feel like a slap in the face to a dying patient.
Amid For-Profit Surge, Rural Hospice Has Offered Free Care for 40 Years
Tiny Washington state hospice accepts no federal funds, relies on community volunteers and donations to serve the dying.
Dementia Patient At Center of Spoon-Feeding Controversy Dies
Nora Harris, 64, who had early-onset Alzheimer’s disease, raised questions about the power — and limits — of an advance directive to withdraw care.
In Oregon, End-of-Life Wishes Are Just A Click Away
A new link creates two-way access to the state registry that documents the type of medical care sick and frail patients want — or refuse.
Quiz: How Well Are You Paying Attention?
To strengthen your core knowledge of health care policy, it helps to be a regular reader of Kaiser Health News. Here’s a pop quiz to gauge what you have learned.
Shedding New Light On Hospice Care: No Need To Wait For The ‘Brink Of Death’
Hospice care often prompts fear and misunderstanding, but the services provided can lead to less pain and trauma at the end of life.
Despite Advance Directive, Dementia Patient Denied Last Wish, Says Spouse
Oregon court says Alzheimer’s patient Nora Harris must be spoon-fed. But her husband says she never wanted to live like this.
Medicare Unveils ‘Skeletal’ Site For Hospice Comparison Shopping
This is the first federal website designed to help families choose a hospice, but experts aren’t impressed.
Medicare ayuda a 575,000 personas a hacer planes para el final de la vida
En 2016, el Medicare comenzó a pagar por las sesiones en las que pacientes, médicos y familiares discuten sobre las decisiones a tomar cuando se acerca el final de la vida.
End-Of-Life Advice: More Than 500,000 Chat On Medicare’s Dime
In the first year of payments for advance-care planning sessions, once decried as ”death panels,“ use is higher than expected, new data show.
¿Por qué las personas no hacen planes para el final de la vida?
Aunque se han promovido directrices anticipadas durante casi 50 años, sólo un tercio de los adultos estadounidenses las prepara, revela un estudio reciente.