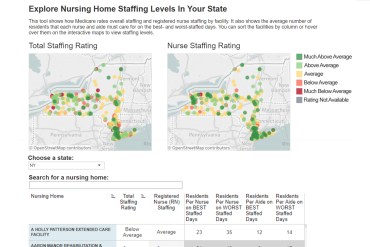
Look-Up: How Nursing Home Staffing Fluctuates Nationwide
Use this tool to see staffing levels at skilled nursing homes in the U.S.
Trump escucha quejas de la industria y bajan las multas en hogares de adultos mayores
Bajo la administración actual, la multa promedio se redujo a $28,405, muy por debajo de los $41,260 en 2016, el último año en el cargo del presidente Barack Obama.
Nursing Home Fines Drop As Trump Administration Heeds Industry Complaints
Inspectors are citing nursing facilities for violating health and safety more often than during the Obama administration. But the average fine is nearly a third lower than it was before President Donald Trump took office.
Assisted Living’s Breakneck Growth Leaves Safety Of Dementia Patients Behind
An analysis of inspection records in California, Florida and Texas shows significant numbers of violations related to assisted living residents with dementia.
1,400 Nursing Homes Get Lower Medicare Ratings Because Of Staffing Concerns
Medicare said those homes either lacked a registered nurse for “a high number of days” over three months, provided data the government couldn’t verify or didn’t supply their payroll data at all.
‘Like A Ghost Town’: Erratic Nursing Home Staffing Revealed Through New Records
Daily nursing home payroll records just released by the federal government show the number of nurses and aides dips far below average on some days and consistently plummets on weekends.
Medicare Takes Aim At Boomerang Hospitalizations Of Nursing Home Patients
One in 5 Medicare patients who leave the hospital for a nursing home end up back in the hospital. To discourage this, the Centers for Medicare & Medicaid Services will soon give bonuses and penalties to facilities based on their rehospitalization rates.
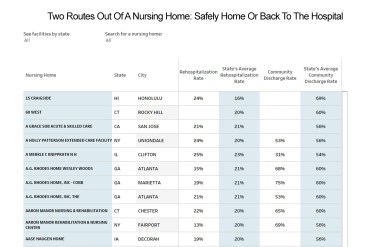
Look-Up: Compare Nursing Homes’ Track Records On Boomerang Hospitalizations
Use this tool to see how skilled nursing homes in the U.S. performed on two metrics of quality.
Care Suffers As More Nursing Homes Feed Money Into Corporate Webs
Increasingly, owners of nursing homes outsource services to companies in which they also have financial interest or control. That allows the nursing homes to claim to be in the red while owners reap hidden profits.
Trump Administration Relaxes Financial Penalties Against Nursing Homes
Medicare is discouraging regional offices from levying fines for “one-time mistakes” or from using daily fines that seek to put pressure on nursing homes to make changes.
Infection Lapses Rampant In Nursing Homes But Punishment Is Rare
A Kaiser Health News analysis of federal inspection records shows that nursing home inspectors labeled mistakes in infection control as serious for only 161 of the 12,056 homes they have cited since 2014.
Why Glaring Quality Gaps Among Nursing Homes Are Likely To Grow If Medicaid Is Cut
Medicaid covers about two-thirds of nursing home residents, but it pays less than other types of insurance.
Nursing Home Disaster Plans Often Faulted As ‘Paper Tigers’
Too often enforcement of rules for dealing with crisis is lax, advocates for nursing home residents say.
Nursing Homes Move Into The Insurance Business
Although proponents say the policies offered by nursing homes are more attuned to patients, some report frustrations when trying to dispute care decisions.
Half The Time, Nursing Homes Scrutinized On Safety By Medicare Are Still Treacherous
Of the 528 nursing homes that graduated from special focus status before 2014 and are still operating, more than half — 52 percent — have harmed patients or operated in a way that put patients in serious jeopardy within the past three years, a KHN analysis finds.
In The End, Even The Middle Class Would Feel GOP Squeeze On Nursing Home Care
Medicaid pays for two-thirds of nursing home residents, but some recipients don’t even know they’re on it.
When Looking For A Nursing Home, You May Get Little Help From Your Hospital
Hospitals rarely help patients find the best nursing home. When they do advise, hospitals sometimes push their own facilities.