Latest KFF Health News Stories
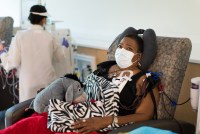
Massage Therapists Ease the Pain of Hospice Patients — But Aren’t Easy to Find
The pandemic disrupted the massage industry. Now those who specialize in hospice massage therapy are in demand and redefining their roles.
‘My Time to Live’: Through Novel Program, Kidney Patients Get Palliative Care, Dialysis ’Til the End
Seattle’s Northwest Kidney Centers, which pioneered kidney failure treatment 50 years ago, now pairs dying patients with hospice services, without forcing them to forgo the comfort dialysis can provide.
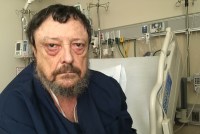
Palliative Care Helped Family Face ‘The Awful, Awful Truth’
Elizabeth and Robert Mar would have celebrated 50 years of marriage in August. Instead, they died within a day of each other. Their two very different deaths illustrate how palliative care is changing to help patients and families cope with the coronavirus pandemic.
Beset By Lawsuits And Criticism In U.S., Opioid Makers Eye New Market In India
What began in India as a populist movement to bring inexpensive morphine to the diseased and dying poor has paved the way for a booming pain management industry. Now, new customers are being funneled to U.S. drugmakers bedeviled by a government crackdown back home.
Kathy Brandt, A Hospice Expert Who Invited The World Into Her Own Last Days With Cancer, Dies
Kathy Brandt and her wife, Kim Acquaviva, national experts in hospice and palliative care, shared intimate details of Brandt’s experience with terminal cancer before her death Sunday.
La charla que tienen que tener los adultos mayores con sus médicos antes de una cirugía
Muchas veces los médicos no hablan con sus pacientes y familiares sobre los riesgos potenciales y las complicaciones que se pueden presentar durante o después de una intervención.
The Talk Seniors Need To Have With Doctors Before Surgery
Surgeons are rethinking the old notions of “informed consent.” With older patients especially, a push is on to talk candidly about what a surgery will do, its risks and how it will affect their quality of life.
‘Stonewall Generation’ Confronts Old Age, Sickness — And Discrimination
For a generation of LGBTQ people who lived through unprecedented social change, getting older poses new challenges — lack of services, discrimination, neglect and even abuse.
Facebook Live: Inclusive Care at the End of Life: The LGBTQ+ Experience
For a generation of LGBTQ+ people who lived through unprecedented social change, getting older poses new challenges. When it comes to seeking elder care, concerns about lack of services, discrimination, neglect and even abuse threaten to reverse recent progress.
‘Living Their Values’: Palliative Care Power Couple Faces Cancer At Home
Kathy Brandt and Kim Acquaviva are both leaders in the world of hospice and palliative care. When Brandt learned she was dying of ovarian cancer, the couple decided it could be a teachable moment.
Congress Targets Misuse Of Hospice Drugs
In the bipartisan opioid bill headed to the president’s desk, hospice workers would be allowed to destroy patients’ unneeded opioids, reducing the risk that families misuse them.
Decisión de Barbara Bush al final de su vida crea debate sobre los “cuidados paliativos”
Muchos creen que elegir los “cuidados paliativos” significa abandonar el tratamiento. Expertos aclaran por qué esta creencia es errónea.
Barbara Bush’s End-Of-Life Decision Stirs Debate Over ‘Comfort Care’
The former first lady’s announcement “not to seek additional medical treatment” and to focus on “comfort care” shone a light on end-of-life choices.
Reverberations From War Complicate Vietnam Veterans’ End-Of-Life Care
Vietnam veterans’ wartime experiences — and their lasting psychological toll — can make it harder to treat their physical and emotional pain as they approach death.
Consejos para enfrentar la mala atención en hospitales
El paciente tiene derecho a reclamar si cree que no está recibiendo una atención adecuada. Y el hospital debe resolver el problema rápidamente.
This Thanksgiving, Carve Out Time To Talk About End-Of-Life Wishes
A vital tradition is gaining steam as more families use the holiday gathering to discuss and document advance-care plans.
Problems With Your Hospital Care? Speak Up!
If you’re in the hospital and aren’t happy with how they are treating you, here are some simple steps to improve your situation.
Hospice Workers Who Care For The Dying Don’t Plan Ahead Themselves
Fewer than half of health care workers at a nonprofit Florida hospice had completed advance directives for end-of-life care.
Dying At Home In An Opioid Crisis: Hospices Grapple With Stolen Meds
As more patients receive hospice care at home, some of the powerful, addictive drugs they’re prescribed are ending up in the wrong hands.
¿Por qué las personas no hacen planes para el final de la vida?
Aunque se han promovido directrices anticipadas durante casi 50 años, sólo un tercio de los adultos estadounidenses las prepara, revela un estudio reciente.