
Last summer, Neil Mahoney was diagnosed with stage 4 cancer. Mahoney had to spend his last days fighting to find doctors willing to help him end his life.(Heidi de Marco/KHN)
GOLDEN, Colo. ― The call came the last week of September, when Neil Mahoney could still stagger from his bed to the porch of his mobile home to let out his boisterous yellow Lab, Ryder.
Rodney Diffendaffer, a clinical pharmacist in Longmont, 45 miles away, had left a message.
Your prescription is ready, it said.
Mahoney, a once-rugged outdoorsman now reduced to bones, his belly swollen with incurable cancer, sighed with relief. After months of obstacles, the frail 64-year-old finally had access to lethal drugs under Colorado’s 2016 End of Life Options Act, one of a growing number of U.S. state laws that allow terminally ill patients to obtain medications to end their lives.
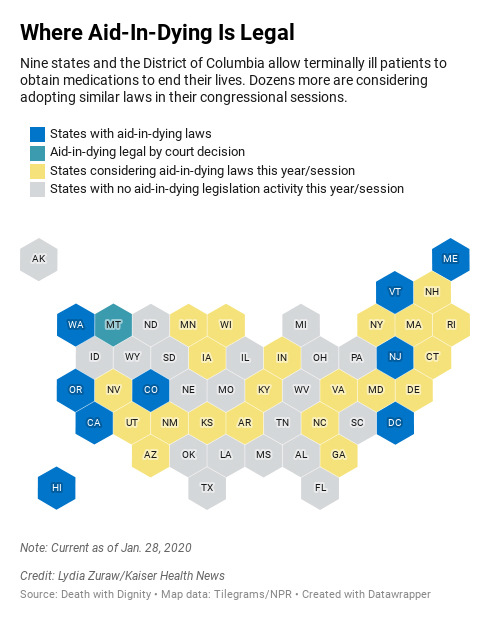
Even as an increasing number of U.S. states have legalized aid-in-dying laws, exercising that option is challenging for patients in a country where most large hospital systems have deep religious ties and the religious right is powerful. One in 6 hospital patients is now cared for at a Catholic hospital, according to the Catholic Health Association. Aid-in-dying is a legal right, but desperate patients are often left feeling they are doing something terribly, morally wrong.
Centura Health Corp., the Christian-run hospital where Mahoney sought treatment for his cancer, regards the practice as “intrinsically evil,” citing the firm’s governing rules, the Ethical and Religious Directives for Catholic Health Care Services. The hospital has barred its doctors from following the state law. In August, it fired his physician, Dr. Barbara Morris, for consulting with Mahoney with the aim of carrying out his wishes.
As his condition deteriorated over the summer, Mahoney left the lawsuit, with Morris still unable to assist him. She sued the hospital for wrongful dismissal; the case is pending. In December, Centura officials filed a countersuit that says the hospital’s actions are protected by the U.S. and state constitutions’ freedom of religion guarantees.

Mahoney had access to lethal drugs under Colorado’s 2016 End of Life Options Act, a law that allows terminally ill patients to obtain medications to end their lives. He was the patient at the center of a legal battle over whether a Christian-run hospital system could bar its doctors from following the law.(Heidi de Marco/KHN)
In opposing the practice, the country’s religious institutions have received support from the Trump administration, which has consistently given providers wide latitude to refuse to participate in medical interventions they object to on religious grounds, though that previously applied primarily to abortion and contraception.
That leaves dying patients like Mahoney feeling abandoned during the most vulnerable time of their lives. When Centura fired Morris for encouraging “a morally unacceptable option,” Mahoney lost both his doctor and the confidence that he would be able to end his life when the suffering became too great.
So the brief message on his phone meant an important victory.
“This way I can say, ‘Yes, I can go,’” he said last summer. “I can call them up with a couple days’ notice and do it.”
Legal But Not Accessible
Oregon was out front in permitting aid-in-dying, approving it more than two decades ago. In recent years, eight other states and the District of Columbia have allowed the practice. It’s being considered in more than a dozen others.
Even when the practice is legal, it often isn’t accessible. Some doctors are barred from participating by their employers. Others refuse to do so. In some cases, the drugs themselves may be too expensive. A dose of Seconal, which was once the most commonly prescribed drug for the practice, can run more than $3,000. The government and some private insurers won’t cover it.
One of nine siblings in a close Catholic family, Mahoney seemed an unlikely candidate to test the Colorado law.

Left: Neil Mahoney (wearing a tie in the front row) in a 1962 family portrait in Denver; Right: Mahoney in Boulder, Colorado, in April 2013(Photos courtesy of Patrick Mahoney)
Weathered and rangy, with a reddish crew cut and broad hands, he’d never had a major illness or injury despite years of physical labor. For the past five years, he managed planting crews at Welby Gardens, a wholesale nursery near Denver.
“The dahlias have always been one of my favorites,” Mahoney said. “Just because of the flowers, the way those millions of petals can open up. That just still baffles me.”
He lived with Ryder, his 6-year-old golden Lab, and Lakewood, a sleek calico cat.
Mahoney was never comfortable around doctors, said his youngest brother, Patrick Mahoney, 60, who supported his older brother’s efforts to obtain help in planning his death.
“Neil had a long belief that health systems, including physicians, capitalize on those that are ill,” Patrick Mahoney said.

Mahoney, who worked at a local landscape company, said he’d never had a major illness or injury despite decades of physical labor.(Heidi de Marco/KHN)

Mahoney lived alone with his dog, Ryder, and cat, Lakewood. (Heidi de Marco/KHN)
Neil Mahoney started feeling sick last January, then worse in April and May. By mid-June, he couldn’t ignore a bout of stomach cramps, nausea and vomiting that sent him to urgent care.
Doctors ordered a CT scan, which showed multiple masses on his liver and likely in his lymph nodes, plus tumors at the junction of his stomach and esophagus. In July, tests at a local cancer center confirmed the bad news: stage 4 adenocarcinoma, a cancer that forms in the body’s glands.
There’s no cure, the doctor said. Without treatment, Mahoney could expect to live four more months. With chemotherapy, he might make it a little more than a year.
Neil Mahoney immediately asked about medical aid-in-dying. He was among 65% of Colorado voters who supported the law in 2016, and now he expected to use it. The medical oncologist turned him down flat.
Neil Mahoney recalled: “I feel like I got slapped in the face.”

Mahoney struggled to move around despite the use of his cane. Mahoney eventually lost more than 50 pounds from his 185-pound frame.(Heidi de Marco/KHN)
‘The Healing Ministry’
Mahoney’s primary care doctor had no qualms about participating. At 65, with 40 years of experience, Morris said that, in her view, medical aid-in-dying should be part of a continuum of care for dying patients.
“We cannot know when a person has reached their limit of suffering,” she said. “Only that person knows.”

Dr. Barbara Morris was fired by Centura Health Corp. in August 2019 for wanting to help her patient, Neil Mahoney, under the guidelines of Colorado’s End of Life Options Act.(Heidi de Marco/KHN)
But Centura, jointly run by Catholic and Seventh-day Adventist churches, describes its work as “the healing ministry of Christ.” When it became aware of the plans in the works, Centura fired Morris, contending that Morris had violated an employment contract requiring her to abide by its faith-based rules.
Morris immediately lost her malpractice insurance and access to a medical office, leaving her unable to prescribe drugs or provide care for Mahoney ― and 400 geriatric patients.
The lawsuit she and Mahoney filed in August alleged that Centura’s faith-based policy violates both the End of Life Options Act and Colorado laws barring health systems from interfering with medical judgment. It sought to clarify whether Centura could prevent Morris from helping Mahoney as long as he wasn’t on the health system premises.
“We believe it is a morally unacceptable act, regardless of how you couch it, and we are not going to participate in it,” Centura chief executive Peter Banko told Kaiser Health News.
In December, Centura officials hired Nussbaum Speir Gleason, a Colorado law firm that specializes in religious freedom cases. In its counterclaim, Centura officials are asking a judge to declare that a health care organization cannot be forced to allow its employees to support or carry out provisions of Colorado’s End of Life Options Act.
Mahoney didn’t have the time to let the legal battle play out in the courts. By July, he’d lost 30 pounds from his 185-pound frame. He grew weaker, wrenched with pain from tumors at the junction of his stomach and esophagus.
The Mahoney children had watched their mother, Charlotte Mahoney, endure a slow decline two weeks before her death in 2007 at age 85.
“I did not want to face an agonizing death without any means to help control when and where I will die,” Neil Mahoney told lawyers.
With his own doctor’s hands tied, a desperate Mahoney resorted to a backdoor route to exercise his legal right.

Mahoney was never comfortable around doctors and typically handled health issues on his own. In the weeks preceding his death, he had to take multiple medications to ease nearly constant pain.(Heidi de Marco/KHN)
Rodney Diffendaffer, a pharmacist who runs a network that quietly connects terminally ill patients in Colorado with doctors willing to follow the law, reached out after reading about Mahoney’s dilemma.
“It’s his choice to have that drug,” said Diffendaffer, 51, who works at the independently owned Flatirons Family Pharmacy in Longmont. “No one else should even have a say.”
In the past two years, Diffendaffer and his fledgling group, Dying With Dignity of the Rockies, have helped more than 50 terminally ill Coloradans obtain medications to end their lives.
“I have seen the pure torture that people went through,” said Diffendaffer, who grew up on a farm and says dying animals are treated more humanely.
Instead of planning for retirement, I’m planning for death.
Although nearly 4,000 people in the United States have used a medical aid-in-dying law, under-the-radar groups like Diffendaffer’s have emerged to match patients with doctors willing to help — but not willing to be included on a public list.
“They don’t want to be labeled ‘Dr. Death,’” said Lynne Calkins, a board member for End of Life Choices California, a volunteer group formed in that state last spring.
The problem grows not just from powerful religious medical centers, but also the loud voice of the religious right in national politics as well as a genuine discomfort among some physicians who are loath to use their skills to end lives rather than save them.
Dr. Ira Byock, founder and chief medical officer at the Institute for Human Caring at Providence St. Joseph Health in Gardena, Calif., has long opposed the practice he calls “hastened death.” He said his objections are based on his understanding of his profession, not on faith.
“I can only say that from my perspective, and that of many non-Catholic practitioners, it is outside the scope of medical practice,” he said. “Ending somebody’s life intentionally is not part of medical practice. It is something else.”
In Vermont, where the practice has been legal since 2013, few doctors outside larger cities such as Burlington are trained to administer the law and few pharmacies are equipped to supply the drugs, said Betsy Walkerman, president of the group Patient Choices Vermont.
“The rest of the state is very thin on medical presence,” Walkerman said. “It’s much more difficult.”
In New Jersey, which enacted a law in August, the family of Zeporah “Zebbie” Geller contacted 40 doctors before they found two willing to help. Geller, 80, a retired teacher, had been diagnosed with terminal lung cancer and died on Sept. 30 after ingesting the prescribed medication.

Mahoney made arrangements for his beloved companion to live with his close friend after his passing. “I feel like he knows what’s happening,” said Mahoney. After his death, his cat went to live with Mahoney’s sister.(Heidi de Marco/KHN)
Neil Mahoney’s Choice
Dr. Glenda Weeman, 60, a family physician who operates an independent practice in Longmont, agreed to prescribe aid-in-dying drugs for Mahoney after two exams, which confirmed he met the law’s requirements.
Weeman had prescribed the drugs for only one patient before Mahoney under Colorado’s relatively young law.
“My role is to relieve pain and suffering. That is my job,” Weeman said. “I have to help people understand that there are choices. If you don’t know the choices of how to die, I’m going to help you figure that out.”
By late September, Mahoney had his prescription, which included two anti-nausea drugs and a cocktail of four medications that would induce death. He paid about $575 for it all, out-of-pocket.
Still, he wasn’t sure when — or if — he’d use them. About a third of people who get the drugs don’t wind up taking them, data from Oregon and Washington show.
“It’s a little spooky,” Mahoney said on Sept. 30, sitting in his small, cluttered mobile home. A green T-shirt hung from his bony shoulders; he’d lost another 20 pounds. Around his neck was a pendant that said DNR: Do not resuscitate.
Mahoney still had a list of things to do. A friend had promised to care for Ryder, the dog. The cat might do OK on her own, though his sister later offered to take her. He wanted to write a will.
“It’s quite a turnaround,” he said quietly. “Instead of planning for retirement, I’m planning for death.”

Mahoney and Ryder in late August. On Nov. 5, surrounded by family, Mahoney took his prescribed end-of-life medication. He died within an hour. The once-rugged outdoorsman, now reduced to gaunt bones and a swollen belly, was determined that he ― not the disease ― would decide when he died.(Heidi de Marco/KHN)
Over the next few weeks, Neil grew frailer day by day. Patrick Mahoney, who quit his job to help, said that he and another brother, John, took turns sleeping on their brother’s couch.
Neil Mahoney knew he had a window of time where he could take the medicine. If he waited too long, he wouldn’t be able to swallow it. Then he’d lose his chance to make the choice.
On Tuesday, Nov. 5, he decided it was time.
At 9:45 p.m., in bed, surrounded by family, Neil Mahoney took the drugs to halt anxiety and nausea. Minutes later, using a straw, he quickly drank the rest of the medications, dry powders mixed with raspberry-flavored liquid. Then they waited.
“It was perhaps the hardest hour of our lives,” Patrick Mahoney said.
About 10:45, Patrick “felt for his pulse. I put my hand on his chest to check his respiration rate, and then I said, ‘He’s gone.’”
Reached by email, Barbara Morris was somber about the death of a patient whom the religious teachings of her former employer had prevented her from helping. She has found another place to practice, starting in the new year.
“It was great honor to know Neil both as his doctor and his friend,” she wrote. “Out of respect for his memory, we will continue to advocate for care focused on patient values and wishes.”






