Medicare’s Push To Improve Chronic Care Attracts Businesses, but Not Many Doctors
Most Medicare enrollees have two or more chronic health conditions, making them eligible for a federal program that rewards physicians for doing more to manage their care. It shows promise in reducing costs. But not many doctors have joined.
Biden Is Right About $35 Insulin Cap but Exaggerates Prior Costs for Medicare Enrollees
Most Medicare enrollees likely were not paying a monthly average of $400 — as President Joe Biden stated — before the insulin cap took effect. However, because costs and other factors result in widely varying prices, some Medicare enrollees might have paid that much in a given month.
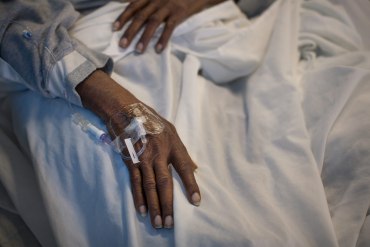
The Burden of Getting Medical Care Can Exhaust Older Patients
It’s estimated that an older patient can spend three weeks of the year getting care — and that doesn’t count the time it takes to arrange appointments or deal with insurance companies.
Social Security Chief Testifies in Senate About Plans to Stop ‘Clawback Cruelty’
Commissioner Martin O’Malley testifies to two Senate panels that his agency will stop the “injustices” of suspending people’s monthly benefits to recover alleged overpayments. The burden will be on the Social Security Administration to prove the beneficiary was to blame.
Exclusive: Social Security Chief Vows to Fix ‘Cruel-Hearted’ Overpayment Clawbacks
New Social Security Commissioner Martin O’Malley is promising to change how the agency reclaims billions of dollars it wrongly pays to beneficiaries, saying the existing process is “cruel-hearted and mindless.”
Concerns Grow Over Quality of Care as Investor Groups Buy Not-for-Profit Nursing Homes
For-profit groups own more than 70% of U.S. nursing homes. Industry leaders and researchers wonder whether corporations and investors can succeed where not-for-profit organizations have struggled. Or, will quality of care suffer in the name of making money?
An Arm and a Leg: The Medicare Episode
On this episode of “An Arm and a Leg,” host Dan Weissmann breaks down the complicated and expensive world of Medicare with practical tips to pick the right plan and avoid penalties.
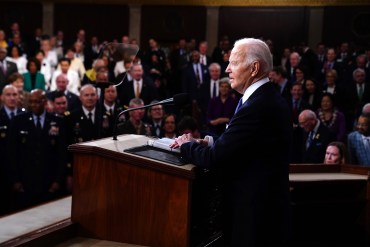
Biden Said State of the Union Is Strong and Made Clear His Campaign Is Off and Running
President Joe Biden used his roughly 68-minute address to Congress to counter lackluster public approval ratings and draw clear contrasts between his administration’s policies and those of Donald Trump and some congressional Republicans. Abortion and health care were in the spotlight.
Operating in the Red: Half of Rural Hospitals Lose Money, as Many Cut Services
A recent report finds half of America’s rural hospitals are losing money, and many are struggling to stay open. Researchers and advocates worry the hospitals’ financial spiral will have immediate and long-term health effects on their communities.
Whistleblower Accuses Aledade, Largest US Independent Primary Care Network, of Medicare Fraud
A recently unsealed lawsuit alleges Aledade Inc. developed billing software that boosted revenues by making patients appear sicker than they were.
America Worries About Health Costs — And Voters Want to Hear From Biden and Republicans
The presidential election is likely to turn on the simple question of whether Americans want Donald Trump back in the White House. But health care tops the list of household financial worries for adults from both parties.
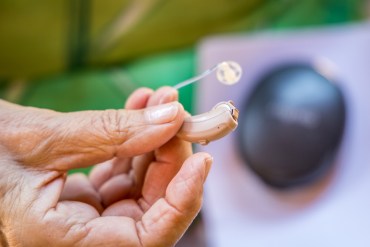
Say That Again: Using Hearing Aids Can Be Frustrating for Older Adults, but Necessary
Hearing loss is more than a nuisance. It also raises the risk of cognitive decline, dementia, falls, depression, and social isolation.
Death and Redemption in an American Prison
More than a quarter century after an inmate helped start a hospice program in one of the nation’s most notorious prisons, he is trying to spread the idea.
Patients See First Savings From Biden’s Drug Price Push, as Pharma Lines Up Its Lawyers
A restructuring of the Medicare drug benefit has wiped out big drug bills for people who need expensive medicines. But the legal battle over drug negotiations means uncertainty over long-term savings.
KFF Health News' 'What the Health?': Biden Wins Early Court Test for Medicare Drug Negotiations
A federal district court judge dismissed a lawsuit attempting to invalidate the Biden administration’s Medicare prescription-drug price negotiation program. But the suit turned on a technicality, and several more court challenges are in the pipeline. Meanwhile, health policy pops up in Super Bowl ads, as Congress approaches yet another funding deadline. Alice Miranda Ollstein of Politico, Lauren Weber of The Washington Post, and Rachel Cohrs of Stat join KFF Health News’ Julie Rovner to discuss these issues and more. Plus, for “extra credit,” the panelists suggest health policy stories they read this week they think you should read, too.
Do We Simply Not Care About Old People?
Recently, thousands of older Americans have been dying weekly of covid. But most Americans aren’t wearing masks in public, a move that could prevent infections. Many at-risk seniors aren’t getting antiviral therapies, and older adults in nursing homes aren’t getting vaccines. Why?
Where Are the Nation’s Primary Care Providers? It’s Not an Easy Answer
Politicians keep talking about fixing primary care shortages. But flawed national data leaves big holes in how to evaluate which policies are effective.
Senate Probes the Cost of Assisted Living and Its Burden on American Families
In the wake of a KFF Health News-New York Times series, members of the Special Committee on Aging are asking residents and their families to submit their bills and are calling for a Government Accountability Office study.
Preparing to Hang Up the Car Keys as We Age
As cognitive skills erode with age, driving skills weaken, but an aging driver may not recognize that. Advance directives on driving are one way to handle this challenge.
Medicare Advantage Is Popular, but Some Beneficiaries Feel Buyer’s Remorse
Medicare Advantage plans are booming — 30.8 million of the 60 million Americans with Medicare are now enrolled in the private plans rather than the traditional government-run program. But a little-known fact: Once you’re in a Medicare Advantage plan, you may not be able to get out. Traditional Medicare usually requires beneficiaries to pay 20 […]