Readers Slam Hospital Monopolies and Blame the Feds for Understaffed Nursing Homes
KFF Health News gives readers a chance to comment on a recent batch of stories.
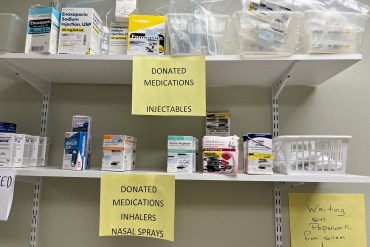
These Programs Put Unused Prescription Drugs in the Hands of Patients in Need
States and counties look to expand programs that accept donations of unused surplus drugs from places like nursing homes and hospitals and redistribute them to low-income and uninsured residents.
Desperate Families Search for Affordable Home Care
Facing a severe shortage of aides and high costs, people trying to keep aging loved ones at home often cobble together a patchwork of family and friends to help.
What to Know About Home Care Services
Finding an aide to help an older person stay at home safely takes work. Here’s a guide.
In Congress, Calls Mount for Social Security to Address Clawbacks
In the wake of a KFF Health News-Cox Media Group investigation, U.S. lawmakers are asking what Social Security will do about its demands on their constituents to repay money already distributed — and sometimes in error. Sen. Rick Scott called the agency’s actions “unacceptable.”
Adultos mayores, detectives contra avisos engañosos de Medicare Advantage
Funcionarios de los Centros de Servicios de Medicare y Medicaid le han pedido a las personas mayores y a otros miembros de la comunidad que sean detectives contra el fraude, denunciando tácticas de venta engañosas al 800-MEDICARE.
Uncle Sam Wants You … to Help Stop Insurers’ Bogus Medicare Advantage Sales Tactics
The Biden administration wants to crack down on deceptive or misleading Medicare Advantage and drug plan sales tactics. It’s counting on beneficiaries to help catch offenders.
Medicare Advantage Increasingly Popular With Seniors — But Not Hospitals and Doctors
Some hospitals and physician groups are rejecting Medicare Advantage plans over payment rates and coverage restrictions, causing turmoil for patients.
Coping with disability — and the cost of coping with disability — is an enormously important issue for older adults. Nora Super, an expert on aging, shares her personal story.
Back Pain? Bum Knee? Be Prepared to Wait for a Physical Therapist
Physical therapists left the field en masse during the covid-19 pandemic, even as demand from aging baby boomers skyrocketed. While universities try to boost their training programs to increase the number of graduates, patients seeking relief from often debilitating pain are left to wait.
A Guide to Long-Term Care Insurance
Deciding when, or whether, to buy long-term care insurance can be complex. Here’s what to know.
Why Long-Term Care Insurance Falls Short for So Many
The private insurance market has proved wildly inadequate in providing financial security for millions of older Americans, in part by underestimating how many policyholders would use their coverage.
What to Know About Assisted Living
The facilities can look like luxury apartments or modest group homes and can vary in pricing structures. Here’s a guide.
Extra Fees Drive Assisted Living Profits
The add-ons pile up: $93 for medications, $50 for cable TV. Prices soar as the industry leaves no service unbilled, out of reach for many families.
New Social Security Report Shows Growing Overpayment Problem Tops $23B
Social Security has been overpaying recipients for years, then demanding the money back, leaving people with bills for up to tens of thousands of dollars or more.
KFF Health News' 'What the Health?': Congress Kicks the (Budget) Can Down the Road. Again.
Congress narrowly avoided a federal government shutdown for the second time in six weeks, as Democrats came to the rescue of divided House Republicans over annual spending bills that were supposed to be finished by Oct. 1. But the brinksmanship is likely to repeat itself early in 2024, when the next temporary spending patches expire. Meanwhile, a pair of investigations unveiled this week demonstrate how difficult it still is for seniors to get needed long-term and rehabilitation care. Alice Miranda Ollstein of Politico, Rachel Cohrs of Stat, and Joanne Kenen of Johns Hopkins University and Politico Magazine join KFF Health News’ Julie Rovner to discuss these issues and more.
Facing Financial Ruin as Costs Soar for Elder Care
The United States has no coherent system of long-term care, leading many to struggle to stay independent or rely on a patchwork of solutions.
Adult Children Discuss the Trials of Caring for Their Aging Parents
The financial and emotional toll of providing and paying for long-term care is wreaking havoc on the lives of millions of Americans. Read about how a few families are navigating the challenges, in their own words.
What Long-Term Care Looks Like Around the World
Most countries spend more than the United States on care, but middle-class and affluent people still bear a substantial portion of the costs.
Who Will Care for Older Adults? We’ve Plenty of Know-How but Too Few Specialists
The principles and practices of geriatrics are being widely disseminated. And we understand much more now about how to improve older adults’ care. Yet we don’t have enough geriatricians to meet the growing demand.