Social Security Chief Orders Broad Review of Benefit Overpayments
In the wake of an investigation by KFF Health News and Cox Media Group, the SSA acting commissioner said a special team will review “overpayment policies and procedures” and report directly back to her.
Social Security Overpayments Draw Scrutiny and Outrage From Members of Congress
Lawmakers are faulting the Social Security Administration for issuing billions of dollars of payments that beneficiaries weren’t entitled to receive — and then demanding the money back — in the wake of an investigation by KFF Health News and Cox Media Group.
New Medicare Advantage Plans Tailor Offerings to Asian Americans, Latinos, and LGBTQ+
As more seniors opt for Medicare Advantage, a few small insurers have begun offering plans that provide culturally targeted benefits for cohorts including Asian Americans, Latinos, and LGBTQ+ people. The approach, policy researchers say, has potential and perils.
Readers Rail at Social Security Overpayments and Insurers’ Prior Authorizations
KFF Health News gives readers a chance to comment on a recent batch of stories.
Nuevos planes de Medicare Advantage adaptan ofertas para asiáticos, latinos y LGTBQ+
A medida que Medicare Advantage gana popularidad entre los adultos mayores, tres compañías del sur de California están lanzando nuevos planes que se enfocan en comunidades culturales y étnicas, con ofertas especiales y profesionales que hablan su idioma nativo.
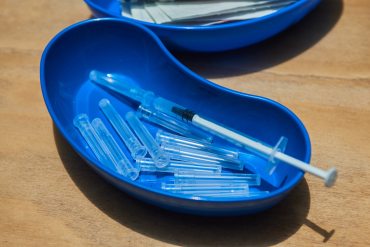
As Covid Infections Rise, Nursing Homes Are Still Waiting for Vaccines
“People want covid-19 to be in the rearview mirror,” one nursing home official says. Faced with a slow rollout of the updated covid vaccines, and without state mandates for workers to get vaccinated, most skilled nursing facilities are relying on persuasion to boost vaccination rates among staff and residents.
Cuando pienses en tu salud, no te olvides de tus ojos
Muchos planes de salud cubren los exámenes de visión de rutina, pero estos generalmente no incluyen el tipo de examen que se utiliza para recetar anteojos y lentes de contacto.
When You Think About Your Health, Don’t Forget Your Eyes
Americans think losing their eyesight would be one of the worst possible health outcomes, yet millions lack a fundamental understanding of eye health.
Rural Nursing Home Supporters Fear Proposed Staffing Standards Will Trigger More Closures
The Biden administration says a recently proposed minimum staffing standard would help ensure quality care, but nursing home leaders predict many rural facilities would struggle to meet it.
Social Security Overpays Billions to People, Many on Disability. Then It Demands the Money Back.
Beneficiaries in five states described what happened when they received letters calling on them to return overpayments that can reach tens of thousands of dollars or more.
Por qué los CDC recomiendan el nuevo refuerzo contra covid para todos
El Comité Asesor sobre Prácticas de Inmunización de los CDC votó 13-1 a favor de la moción después de meses de debate sobre si limitar los refuerzos a grupos de alto riesgo.
Why the CDC Has Recommended New Covid Boosters for All
As covid-19 hospitalizations tick upward with fall approaching, the CDC says it’s time for new boosters — and not only for those at highest risk of serious disease. Here are seven things you need to know.
KFF Health News' 'What the Health?': Welcome Back, Congress. Now Get to Work.
Congress returns from its summer recess with a long list of tasks and only a few work days to get them done. On top of the annual spending bills needed to keep the government operating, on the list are bills to renew the global HIV/AIDS program, PEPFAR, and the community health centers program. Meanwhile, over the recess, the Biden administration released the names of the first 10 drugs selected for the Medicare price negotiation program.
Biden Administration Proposes New Standards to Boost Nursing Home Staffing
The proposal would require major hiring at the most sparsely staffed homes. But the proposal is already badly received by the nursing home industry, which claims it can’t boost wages enough to attract workers.
Exclusive: CMS Study Sabotages Efforts to Bolster Nursing Home Staffing, Advocates Say
Research commissioned by the Centers for Medicare & Medicaid Services analyzed only staffing levels below what experts have previously called ideal. Patient advocates have been pushing for more staff to improve care.
A New Medicare Proposal Would Cover Training for Family Caregivers
The federal government is proposing having Medicare pay professionals to train family caregivers how to perform tasks like bathing and dressing their loved ones, and properly use medical equipment.
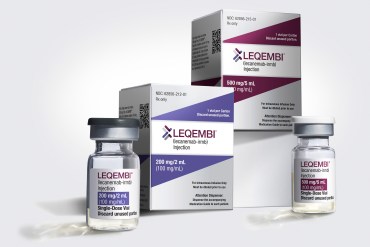
New Alzheimer’s Drug Raises Hopes — Along With Questions
Clinics serving Alzheimer’s patients are working out the details of who will get treated with the new drug Leqembi. It won’t be for everyone with memory-loss symptoms.
The Real Costs of the New Alzheimer’s Drug, Most of Which Will Fall to Taxpayers
The annual cost of lecanemab treatment quadruples if the expense of brain scans to monitor for bleeds and other associated care is factored in. The full financial toll likely puts it beyond reach for low-income seniors at risk of Alzheimer’s, experts say.
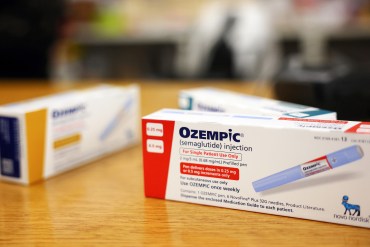
New Weight Loss Drugs Carry High Price Tags and Lots of Questions for Seniors
Although nearly 40% of Americans 60 and older are obese, Medicare doesn’t cover weight loss medications. Meanwhile, studies haven’t thoroughly examined new drugs’ impact on older adults.
En las personas mayores, un poco de sobrepeso no es tan malo
Comprender las pruebas científicas y la opinión de los expertos sobre los problemas de peso en los adultos mayores no es fácil.