Latest KFF Health News Stories
Readers Call on Congress to Bolster Medicare and Fix Loopholes in Health Policy
KFF Health News gives readers a chance to comment on a recent batch of stories.
Si eres pobre, un tratamiento de fertilidad suele ser un sueño inaccesible
Pero las personas con ingresos más bajos, a menudo de minorías, tienen más probabilidades de estar cubiertas por Medicaid o por seguros limitados que no tienen esta cobertura.
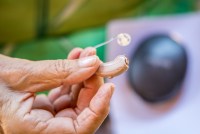
Say That Again: Using Hearing Aids Can Be Frustrating for Older Adults, but Necessary
Hearing loss is more than a nuisance. It also raises the risk of cognitive decline, dementia, falls, depression, and social isolation.
An Arm and a Leg: Wait, Is Insulin Cheaper Now?
Did the price of insulin go down? It’s not quite that simple. On this episode of “An Arm and a Leg,” producer Emily Pisacreta explores recent changes to the cost of the diabetes medication.
Without Medicare Part B’s Shield, Patient’s Family Owes $81,000 for a Single Air-Ambulance Flight
Sky-high bills from air-ambulance providers have sparked complaints and federal action in recent years. But a rural Tennessee resident fell through the cracks of billing protections — and a single helicopter ride could cost much of her estate’s value.
If You’re Poor, Fertility Treatment Can Be Out of Reach
For low-income people who are on Medicaid or whose employer health plan is skimpy, help for infertility seems unattainable.
Patients See First Savings From Biden’s Drug Price Push, as Pharma Lines Up Its Lawyers
A restructuring of the Medicare drug benefit has wiped out big drug bills for people who need expensive medicines. But the legal battle over drug negotiations means uncertainty over long-term savings.
Southern Lawmakers Rethink Long-Standing Opposition to Medicaid Expansion
While many Republican state lawmakers remain firmly against Medicaid expansion, some key leaders in holdout states are showing a willingness to reconsider. Public opinion, financial incentives, and widening health care needs make resistance harder.
KFF Health News' 'What the Health?': Biden Wins Early Court Test for Medicare Drug Negotiations
A federal district court judge dismissed a lawsuit attempting to invalidate the Biden administration’s Medicare prescription-drug price negotiation program. But the suit turned on a technicality, and several more court challenges are in the pipeline. Meanwhile, health policy pops up in Super Bowl ads, as Congress approaches yet another funding deadline. Alice Miranda Ollstein of Politico, Lauren Weber of The Washington Post, and Rachel Cohrs of Stat join KFF Health News’ Julie Rovner to discuss these issues and more. Plus, for “extra credit,” the panelists suggest health policy stories they read this week they think you should read, too.
The No Surprises Act Comes With Some Surprises
The No Surprises Act, the landmark law intended to protect patients from surprise out-of-network medical bills, has come with, well, some surprises. A little more than two years after it took effect, there’s good and bad news about how it’s working. First, it’s important to note that the law has successfully protected millions of patients […]
For the Love of Health Care and Health Policy
KFF Health News shares the crème de la crème of reader-submitted health policy valentines. Two of our favorites melted our hearts and inspired original illustrations.
GoFundMe, ¿realmente ayuda a pagar facturas médicas?
Incluso defensores de pacientes y personal del área de ayuda financiera en hospitales recomiendan iniciar una sesión en GoFundMe como una alternativa a terminar con una cuenta en una agencia de cobros.
GoFundMe Has Become a Health Care Utility
Resorting to crowdfunding to pay medical bills has become so routine, in some cases health professionals recommend it.
Cerca de 10 millones ya perdieron Medicaid, y todavía faltan meses de purga
Medicaid y el Programa de Seguro de Salud Infantil crecieron hasta alcanzar un récord de 94 millones de inscritos durante la pandemia.
Halfway Through ‘Unwinding,’ Medicaid Enrollment Is Down About 10 Million
While more Medicaid beneficiaries have been purged in the span of a year than ever before, enrollment is on track to settle at pre-pandemic levels.
Halfway Through ‘Unwinding,’ Medicaid Enrollment Is Down About 10 Million
We’re halfway through the Medicaid “unwinding,” in which states are dropping people from the government health insurance program for the first time since the pandemic began. Millions of people have been dumped from the rolls since April, often for procedural issues like failing to respond to notices or return paperwork. But at the same time, […]
KFF Health News' 'What the Health?': The Struggle Over Who Gets the Last Word
As science skepticism pervades politics, the Supreme Court will soon consider two cases that seek to define the power of “experts.” Meanwhile, abortion opponents are laying out plans for how Donald Trump, if reelected as president, could effectively curtail abortion even in states where it remains legal. Sandhya Raman of CQ Roll Call, Joanne Kenen of Johns Hopkins University and Politico Magazine, and Sarah Karlin-Smith of the Pink Sheet join KFF Health News’ Julie Rovner to discuss these issues and more. Also this week, Rovner interviews Samantha Liss, who reported and wrote the latest KFF Health News-NPR “Bill of the Month” feature about a husband and wife who got billed for preventive care that should have been fully covered.
The FTC Is Attacking Drugmakers’ ‘Patent Thickets’
It’s a big job clearing out so-called “patent thickets” drugmakers create to keep their products’ prices high. But the Federal Trade Commission is giving it a shot.
An Arm and a Leg: Self-Defense 101: Keeping Your Cool While You Fight
On this episode of “An Arm and a Leg,” host Dan Weissmann seeks advice for fighting unfair medical bills from an unexpected source: an expert in self-defense.
Readers Weigh Downsides of Medicare Advantage and Stick Up for Mary Lou Retton
KFF Health News gives readers a chance to comment on a recent batch of stories.