Latest KFF Health News Stories
Senate Probes the Cost of Assisted Living and Its Burden on American Families
In the wake of a KFF Health News-New York Times series, members of the Special Committee on Aging are asking residents and their families to submit their bills and are calling for a Government Accountability Office study.
KFF Health News' 'What the Health?': Health Enters the Presidential Race
New Hampshire voters have spoken, and it seems increasingly clear that this November’s election will pit President Joe Biden against former President Donald Trump. Both appear to be making health a key part of their campaigns, with Trump vowing (again) to repeal the Affordable Care Act, and Biden stressing his support for contraception and abortion rights. Meanwhile, both candidates will try to highlight efforts to rein in prescription drug prices. Alice Miranda Ollstein of Politico, Anna Edney of Bloomberg News, and Jessie Hellmann of CQ Roll Call join KFF Health News chief Washington correspondent Julie Rovner to discuss these issues and more. Also this week, Rovner interviews Sarah Somers of the National Health Law Program about the potential consequences for the health care system if the Supreme Court overturns a key precedent attempting to balance executive vs. judicial power.
The FTC Escalates Biden’s Fight Against Drug Prices
It’s daggers out at the Federal Trade Commission in its fight against anticompetitive practices in health care. This past year, it has issued more stringent guidelines to block and discourage hospital mergers, and it investigated practices by middlemen in the drug supply chain. Now drug manufacturers themselves are in the agency’s crosshairs. In November, the FTC challenged the validity of more […]
The Colonoscopies Were Free. But the ‘Surgical Trays’ Came With $600 Price Tags.
Health providers may bill however they choose — including in ways that could leave patients with unexpected bills for “free” care. Routine preventive care saddled an Illinois couple with his-and-her bills for “surgical trays.”
New York Joins Local Governments in Erasing Billions in Medical Debt
New York City is the latest jurisdiction to buy and forgive a backlog of unpaid medical bills for its residents. Local governments across the country, including in the Chicago area, are doing the same to reduce debt burdens for lower-income residents.
With Trump Front of Mind, New Hampshire Voters Cite Abortion and Obamacare as Concerns
New Hampshire’s primary election was dominated by voters’ feelings about Donald Trump. But health care remains a concern — and for Democrats, preserving abortion access is a priority.
In This Oklahoma Town, Most Everyone Knows Someone Who’s Been Sued by the Hospital
Hospitals nationwide face growing scrutiny over how they secure payment from patients, but at one community hospital, the debt collection machine has been quietly humming along for decades.
Insurance Doesn’t Always Cover Hearing Aids for Kids
California’s governor vetoed a bill extending insurance coverage for kids with hearing loss, but most states now require it.
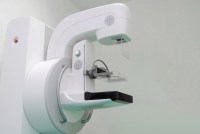
Mamografías que usan inteligencia artificial cuestan dinero extra… pero, ¿vale la pena?
Este software puede identificar patrones y anomalías que los radiólogos humanos podrían pasar por alto. Pero no es el estándar de atención.
Mary Lou Retton’s Explanation of Health Insurance Takes Some Somersaults
The gold-medal gymnast’s explanation of why she remained uninsured has health policy experts doing mental gymnastics — because it makes little sense.
KFF Health News' 'What the Health?': All About the (Government) Funding
With days to go until a large chunk of the federal government runs out of money needed to keep it operating, Congress is still struggling to find a compromise spending plan. Meanwhile, the Supreme Court agreed to hear — this year — a case that pits federal requirements for emergency treatment against state abortion bans. Alice Miranda Ollstein of Politico, Sarah Karlin-Smith of the Pink Sheet, and Tami Luhby of CNN join KFF Health News chief Washington correspondent Julie Rovner to discuss these issues and more. Also this week, Rovner interviews American Medical Association President Jesse Ehrenfeld about the choppy waters facing the nation’s physicians in 2024.
Mammography AI Can Cost Patients Extra. Is It Worth It?
Artificial intelligence software to aid radiologists in detecting problems or diagnosing cancer has been moving rapidly into clinical use, where it shows great promise. But it’s a turnoff for some patients asked to pay out-of-pocket for technology that’s not quite ready for prime time.
Rising Malpractice Premiums Price Small Clinics Out of Gender-Affirming Care for Minors
Even in states where laws protect minors’ access to gender-affirming care, malpractice insurance premiums are keeping small and independent clinics from treating patients.
These Patients Had to Lobby for Correct Diabetes Diagnoses. Was Their Race a Reason?
Adults who develop one autoimmune form of diabetes are often misdiagnosed with Type 2 diabetes. Those wrong diagnoses make it harder to get the appropriate medications and technology to manage their blood sugar. Many Black patients wonder if their race plays a role.
Adultos mayores se sienten “atrapados” en planes de Medicare Advantage
Al parecer el programa de planes privados para adultos mayores comienza a presentar obstáculos cuando surgen enfermedades.
Older Americans Say They Feel Trapped in Medicare Advantage Plans
As enrollment in private Medicare Advantage plans grows, so do concerns about how well the insurance works, including from those who say they have become trapped in the private plans as their health declines.
Most People Dropped in Medicaid ‘Unwinding’ Never Tried to Renew Coverage, Utah Finds
Medicaid officials in Utah conducted a survey to answer a burning question in health policy: What happened to people dropped from the program in the post-pandemic “unwinding”?
Woman Petitions Health Insurer After Company Approves — Then Rejects — Her Infusions
Even people with good insurance aren’t guaranteed affordable care, as this KFF Health News follow-up to one patient’s saga shows.
Utah Survey Shows Why So Many People Were Dumped From Medicaid
It’s one of the biggest mysteries in health policy: What happened to millions of Americans kicked out of Medicaid last year? A survey conducted for state officials in Utah, obtained by KFF Health News, holds some clues. Like many states, Utah terminated Medicaid coverage for a large share of enrollees whose eligibility was reevaluated in […]
An Arm and a Leg: When Hospitals Sue Patients (Part 2)
Why do hospitals sue patients who can’t afford to pay their medical bills? On this episode of “An Arm and a Leg,” host Dan Weissmann investigates such lawsuits and covers new laws and regulations that may change this practice.