Latest KFF Health News Stories
For-Profit Companies Open Psychiatric Hospitals in Areas Clamoring for Care
State institutions and community hospitals have closed inpatient mental health units, often citing staffing and financial challenges. Now, for-profit companies are opening psychiatric hospitals to fill the void.
How Primary Care Is Being Disrupted: A Video Primer
Under pressure from increased demand, consolidation, and changing patient expectations, the model of care no longer means visiting the same doctor for decades.
A State-Sanctioned Hospital Monopoly Raises Concerns
The Federal Trade Commission has long argued that competition makes the economy better. But some states have stopped the agency from blocking hospital mergers that create local or regional monopolies, and the results have been messy. Two dozen states have at some point passed controversial legislation waiving anti-monopoly laws, allowing rival hospitals to merge and replacing competition […]
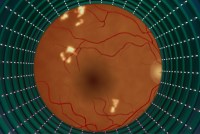
Programas de inteligencia artificial diagnostican retinopatía diabética en minutos
En medio de todo el revuelo en torno a la inteligencia artificial en la atención médica, la tecnología de exámenes de la vista está surgiendo como uno de los primeros casos de uso probados de diagnósticos basados en IA en un entorno clínico.
The Burden of Getting Medical Care Can Exhaust Older Patients
It’s estimated that an older patient can spend three weeks of the year getting care — and that doesn’t count the time it takes to arrange appointments or deal with insurance companies.
As AI Eye Exams Prove Their Worth, Lessons for Future Tech Emerge
With artificial intelligence in health care on the rise, eye screenings for diabetic retinopathy are emerging as one of the first proven use cases of AI-based diagnostics in a clinical setting.
Some Medicaid Providers Borrow or Go Into Debt Amid ‘Unwinding’ Payment Disruptions
Used to operating with scarce resources, Montana Medicaid providers say gaps in state payments have left them struggling further.
This State Isn’t Waiting for Biden To Negotiate Drug Prices
As the federal government negotiates with drugmakers to lower the price of 10 expensive drugs for Medicare patients, impatient legislators in some states are trying to go even further. Leading the pack is Colorado, where a new Prescription Drug Affordability Review Board is set to recommend an “upper payment limit” for drugs it deems unaffordable. In late […]
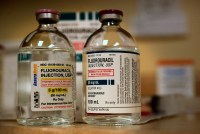
Overdosing on Chemo: A Common Gene Test Could Save Hundreds of Lives Each Year
The FDA and some oncologists have resisted efforts to require a quick, cheap gene test that could prevent thousands of deaths from a bad reaction to a common cancer drug.
After Appalachian Hospitals Merged Into a Monopoly, Their ERs Slowed to a Crawl
Ballad Health was granted the nation’s largest state-sanctioned hospital monopoly in 2018. Since then, its emergency rooms have become more than three times as slow.
KFF Health News' 'What the Health?': The ACA Turns 14
Saturday marks the 14th anniversary of the still somewhat embattled Affordable Care Act. Health and Human Services Secretary Xavier Becerra joins host Julie Rovner to discuss the accomplishments of the health law — and the challenges it still faces. Also this week, Alice Miranda Ollstein of Politico, Tami Luhby of CNN, and Mary Agnes Carey of KFF Health News join Rovner to discuss what should be the final funding bill for HHS for fiscal 2024, next week’s Supreme Court oral arguments in a case challenging abortion medication, and more. Plus, for “extra credit,” the panelists suggest health policy stories they read this week they think you should read, too.
Social Security Chief Testifies in Senate About Plans to Stop ‘Clawback Cruelty’
Commissioner Martin O’Malley testifies to two Senate panels that his agency will stop the “injustices” of suspending people’s monthly benefits to recover alleged overpayments. The burden will be on the Social Security Administration to prove the beneficiary was to blame.
Biden Said Medicare Drug Price Negotiations Cut the Deficit by $160B. That’s Years Away.
Savings estimated by the Congressional Budget Office from allowing the federal government to negotiate Medicare drug prices are based on a 10-year cumulative projection.
Georgia’s Medicaid Work Requirements Costing Taxpayers Millions Despite Low Enrollment
Republican Gov. Brian Kemp’s Georgia Pathways to Coverage program has seen anemic enrollment while chalking up millions in start-up costs — largely in technology and consulting fees. Critics say the money’s being wasted on a costly and ineffective alternative to Obamacare’s Medicaid expansion.
Needle Pain Is a Big Problem for Kids. One California Doctor Has a Plan.
The pain and trauma from repeated needle sticks leads some kids to hold on to needle phobia into adulthood. Research shows the biggest source of pain for children in the health care system is needles. But one doctor thinks he has a solution and is putting it into practice at two children’s hospitals in Northern California.
Under Fire for Massive Health System Hack, Biden Team Leans on Insurers
The Biden administration has hit on a strategy to deal with the massive, industry-paralyzing cyberattack on a UnitedHealth Group unit: pressuring insurers to fix it. Federal officials have been in constant conversation with senior leaders at UnitedHealth and across the industry, including at a Monday meeting where Department of Health and Human Services and White […]
Cuando tu cobertura de salud dentro de la red… simplemente se esfuma
los contratos de las aseguradoras con médicos, hospitales y farmacéuticas (o sus intermediarios, los llamados administradores de beneficios farmacéuticos) pueden cambiar abruptamente de la noche a la mañana.
When Copay Assistance Backfires on Patients
Drugmakers offer copay assistance programs to patients, but insurers are tapping into those funds, not counting the amounts toward patient deductibles. That leads to unexpected charges. But the practice is under growing scrutiny.
How Your In-Network Health Coverage Can Vanish Before You Know It
One of the most unfair aspects of medical insurance is this: Patients can change insurance only during end-of-year enrollment periods or at the time of “qualifying life events.” But insurers’ contracts with doctors, hospitals, and pharmaceutical companies can change abruptly at any time.
KFF Health News' 'What the Health?': Maybe It’s a Health Care Election After All
Health care wasn’t expected to be a major theme for this year’s elections. But as President Joe Biden and former President Donald Trump secured their respective party nominations this week, the future of both Medicare and the Affordable Care Act appears to be up for debate. Meanwhile, the cyberattack of the UnitedHealth Group subsidiary Change Healthcare continues to do damage to the companies’ finances with no quick end in sight. Margot Sanger-Katz of The New York Times, Anna Edney of Bloomberg News, and Joanne Kenen of Johns Hopkins University and Politico Magazine join KFF Health News’ Julie Rovner to discuss these issues and more. Also this week, Rovner interviews Kelly Henning of Bloomberg Philanthropies about a new, four-part documentary series on the history of public health, “The Invisible Shield.” Plus, for “extra credit” the panelists suggest health policy stories they read this week that they think you should read, too.