Latest KFF Health News Stories
Dietary Choices Are Linked to Higher Rates of Preeclampsia Among Latinas
Researchers at the USC Keck School of Medicine found that Latinas who ate vegetables, fruits, and healthy oils-based foods had fewer incidences of preeclampsia. More research is needed to determine the exact diet that could be beneficial.
KFF Health News' 'What the Health?': Florida Limits Abortion — For Now
The Florida Supreme Court handed down dual abortion rulings this week. One said voters will be allowed to decide in November whether to create a state right to abortion. The other ruling, though, allows a 15-week ban to take effect immediately — before an even more sweeping, six-week ban replaces it in May. Meanwhile, President Joe Biden is doubling down on his administration’s health care accomplishments as he kicks off his general election campaign. Lauren Weber of The Washington Post, Joanne Kenen of the Johns Hopkins University schools of nursing and public health, and Tami Luhby of CNN join KFF Health News’ Julie Rovner to discuss these stories and more. Also this week, Rovner interviews health care analyst Jeff Goldsmith about the growing size and influence of UnitedHealth Group in the wake of the Change Healthcare hack.
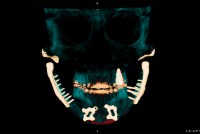
The Horrors of TMJ: Chronic Pain, Metal Jaws, and Futile Treatments
TMJ disorders affect as many as 1 in 10 Americans and yet remain poorly understood and ineffectively treated. Many common treatments used by dentists lack scientific evidence.
End of Internet Subsidies for Low-Income Households Threatens Telehealth Access
A federal program that helped pay for more than 23 million low-income households’ internet access runs out of money soon. The end of the subsidy launched earlier in the pandemic could have profound impacts on health care access.
Feds Join Ranks of Employers with Generous Fertility Benefits
Starting this year, federal employees can choose plans that cover a broad menu of fertility services, including up to $25,000 annually for in vitro fertilization procedures. At the same time, politics around IVF and reproductive health have become a central issue in the current election-year debate.
Attacks on Emergency Room Workers Prompt Debate Over Tougher Penalties
In California, assaulting paramedics or other emergency medical workers in the field carries stiffer fines and jail time than assaulting emergency room staffers. State lawmakers are considering a measure that would standardize the penalties.
Medical Debt Affects Much of America, but Colorado Immigrants Are Hit Especially Hard
Colorado is ahead of the curve on policies to prevent medical debt, but the gap between the debt load in places inhabited primarily by people of color versus non-Hispanic white residents is greater than the national average.
Heat Protections for California Workers Are in Limbo After Newsom Abandons Rules
Proposed rules to protect millions of workers from potentially dangerous heat inside workplaces are dead after Gov. Gavin Newsom’s administration refused to sign off. Labor advocates and state regulators are calling for emergency regulations before temperatures soar this summer.
More Patients Are Losing Their Doctors — And Trust in the Primary Care System
A shortage of primary care providers is driving more people to seek routine care in emergency settings. In Rhode Island, safety-net clinics are under pressure as clinicians retire or burn out, and patients say it’s harder to find care as they lose connections to familiar doctors.
California Universities Are Required to Offer Abortion Pills. Many Just Don’t Mention It.
One year after California became the first state to require public universities to provide abortion pills to students, LAist found that basic information for students to obtain the medication is often nonexistent.
Track Opioid Settlement Payouts — To the Cent — In Your Community
Want to know how much opioid settlement money your city, county, or state has received so far? Or how much it’s expecting in the future? Use our new searchable database to find out.
Hospitals Cash In on a Private Equity-Backed Trend: Concierge Physician Care
Hospitals are increasingly stretching a velvet rope, offering “concierge service” to an affluent clientele. Critics say the practice exacerbates primary care shortages.
Four Years After Shelter-in-Place, Covid-19 Misinformation Persists
False claims that covid vaccines cause deaths and other diseases are still prevalent despite multiple studies showing the vaccines are safe and saved lives.
For-Profit Companies Open Psychiatric Hospitals in Areas Clamoring for Care
State institutions and community hospitals have closed inpatient mental health units, often citing staffing and financial challenges. Now, for-profit companies are opening psychiatric hospitals to fill the void.
How Primary Care Is Being Disrupted: A Video Primer
Under pressure from increased demand, consolidation, and changing patient expectations, the model of care no longer means visiting the same doctor for decades.
A Physician Travels to South Asia Seeking Enduring Lessons From the Eradication of Smallpox
Physician and podcast host Céline Gounder traveled to India and Bangladesh and brought back never-before-heard stories, many from public health workers whose voices have been missing from the record documenting the eradication of smallpox.
Your Doctor or Your Insurer? Little-Known Rules May Ease the Choice in Medicare Advantage
Disputes between hospitals and Medicare Advantage plans are leading to entire hospital systems suddenly leaving insurance networks. Patients are left stuck in the middle, choosing between their doctors and their insurance plan. There’s a way out.
KFF Health News' 'What the Health?': The Supreme Court and the Abortion Pill
The Supreme Court this week heard its first abortion case since overturning Roe v. Wade in 2022, about an appeals court ruling that would dramatically restrict the availability of the abortion pill mifepristone. But while it seems likely that this case could be dismissed on a technicality, abortion opponents have more challenges in the pipeline. Meanwhile, health issues are heating up on the campaign trail, as Republicans continue to take aim at Medicare, Medicaid, and the Affordable Care Act — all things Democrats are delighted to defend. Alice Miranda Ollstein of Politico, Sarah Karlin-Smith of the Pink Sheet, and Lauren Weber of The Washington Post join KFF Health News chief Washington correspondent Julie Rovner to discuss these issues and more. Also this week, Rovner interviews KFF Health News’ Tony Leys, who wrote a KFF Health News-NPR “Bill of the Month” feature about Medicare and a very expensive air-ambulance ride. Plus, for “extra credit,” the panelists suggest health policy stories they read this week they think you should read, too.
California Is Expanding Insurance Access for Teenagers Seeking Therapy on Their Own
A California law that takes effect this summer will grant minors on public insurance the ability to get mental health treatment without their parents’ consent, a privilege that their peers with private insurance have had for years. But the law has become a flashpoint in the state’s culture wars.
The Burden of Getting Medical Care Can Exhaust Older Patients
It’s estimated that an older patient can spend three weeks of the year getting care — and that doesn’t count the time it takes to arrange appointments or deal with insurance companies.