Latest Morning Briefing Stories
Casi 1 de cada 4 adultos desafiliados de Medicaid siguen sin seguro, indica encuesta
Las protecciones que tuvo el programa durante la pandemia, que impedían que se expulsaran beneficiarios, expiraron la primavera pasada.
Nearly 1 in 4 Adults Dumped From Medicaid Are Now Uninsured, Survey Finds
A first-of-its-kind survey of Medicaid enrollees found that nearly a quarter who were dropped from the program in the last year’s unwinding say they’re uninsured.
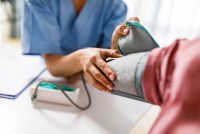
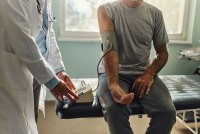
Doctors Take On Dental Duties to Reach Low-Income and Uninsured Patients
More doctors are integrating oral health care into their practices, filling a need in America’s dental deserts.
En California, la cobertura de salud ampliada a inmigrantes choca con las revisiones de Medicaid
El proceso de redeterminación ha afectado de forma desproporcionada a los latinos, que constituyen la mayoría de los beneficiarios de Medi-Cal.
California’s Expanded Health Coverage for Immigrants Collides With Medicaid Reviews
A state policy to extend Medi-Cal to qualified Californians without legal residency is running up against a federal requirement to resume eligibility checks. The redetermination process is causing many Latinos, who make up a majority of Medi-Cal beneficiaries, to be disenrolled.
In California, Faceoff Between Major Insurer and Health System Shows Hazards of Consolidation
Even as Anthem Blue Cross and University of California Health announced a contract agreement this month, analysts say patients are increasingly at risk of being affected by such disputes.
Halfway Through ‘Unwinding,’ Medicaid Enrollment Is Down About 10 Million
While more Medicaid beneficiaries have been purged in the span of a year than ever before, enrollment is on track to settle at pre-pandemic levels.
Halfway Through ‘Unwinding,’ Medicaid Enrollment Is Down About 10 Million
We’re halfway through the Medicaid “unwinding,” in which states are dropping people from the government health insurance program for the first time since the pandemic began. Millions of people have been dumped from the rolls since April, often for procedural issues like failing to respond to notices or return paperwork. But at the same time, […]
Mary Lou Retton’s Explanation of Health Insurance Takes Some Somersaults
The gold-medal gymnast’s explanation of why she remained uninsured has health policy experts doing mental gymnastics — because it makes little sense.
Most People Dropped in Medicaid ‘Unwinding’ Never Tried to Renew Coverage, Utah Finds
Medicaid officials in Utah conducted a survey to answer a burning question in health policy: What happened to people dropped from the program in the post-pandemic “unwinding”?
Utah Survey Shows Why So Many People Were Dumped From Medicaid
It’s one of the biggest mysteries in health policy: What happened to millions of Americans kicked out of Medicaid last year? A survey conducted for state officials in Utah, obtained by KFF Health News, holds some clues. Like many states, Utah terminated Medicaid coverage for a large share of enrollees whose eligibility was reevaluated in […]
States Expand Health Coverage for Immigrants as GOP Hits Biden Over Border Crossings
More than 1 million immigrants, most lacking permanent legal status, are covered by state health programs. Several states, including GOP-led Utah, will soon add or expand such coverage.
Bold Changes Are in Store for Medi-Cal in 2024, but Will Patients Benefit?
California’s Medicaid program is undergoing major changes that could improve health care for residents with low incomes. But they are happening at the same time as several other initiatives that could compete for staff attention and confuse enrollees.
Se avecinan cambios para Medi-Cal en 2024, pero ¿beneficiarán a los pacientes?
A partir del próximo año, más de 700,000 inmigrantes sin papeles serán elegibles para una cobertura completa de Medi-Cal.
Medicaid’s ‘Unwinding’ Can Be Especially Perilous for Disabled People
Earlier this year, Beverly Likens thought she’d done everything she needed to do to keep her Medicaid. Then came an unwelcome surprise: Ahead of surgery to treat chronic bleeding, the hospital said her insurance was inactive, jeopardizing her procedure. Likens had just been diagnosed with severe anemia and given a blood transfusion at the emergency room. “I […]
1 in 3 People Dropped by Utah Medicaid Left Uninsured, a ‘Concerning’ Sign for Nation
About a third of the 130,000 people Utah has dropped from Medicaid this year say they now lack health insurance. It’s a glimpse into the fate of people caught up in Medicaid’s “unwinding.”
Nueva ley de California ofrece protección contra facturas por viajes en ambulancia
En California, casi tres cuartas partes de los traslados de emergencia en ambulancia generan facturas fuera de la red. La factura sorpresa promedio es de $1,209, la más alta del país
New California Law Offers Fresh Protection From Steep Ambulance Bills
The law, which takes effect Jan. 1, prohibits out-of-network ground ambulance operators from billing patients more than they would pay for in-network rides. It also caps how much the uninsured must pay.
GOP Presidential Primary Debate No. 2: An Angry Rematch and the Same Notable No-Show
Though never framed as a marquee issue, the topic of health care crept into the chaotic seven-way faceoff throughout the evening, highlighting Republican culture-war themes.
KFF Health News' 'What the Health?': Underinsured Is the New Uninsured
The percentage of working-age adults with health insurance went up and the uninsured rate dropped last year, the U.S. Census Bureau reported this week. There isn’t much suspense about which way the uninsured rate is now trending, as states continue efforts to strip ineligible beneficiaries from their Medicaid rolls. But is the focus on the uninsured obscuring the struggles of the underinsured? Margot Sanger-Katz of The New York Times, Sarah Karlin-Smith of the Pink Sheet, and Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico join KFF Health News’ Emmarie Huetteman to discuss these issues and more.