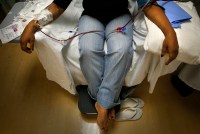
Coverage Denied: Medicaid Patients Suffer As Layers Of Private Companies Profit
Managed-care plans, which reap billions in taxpayer dollars to coordinate care for low-income Americans on Medicaid, outsource crucial treatment decisions to subcontractors that aren’t directly accountable to the government. In California, health officials say one firm improperly withheld or delayed care for hundreds of people.
Billions In ‘Questionable Payments’ Went To California’s Medicaid Insurers And Providers
The money was paid on behalf of more than 400,000 people who may have been ineligible for the public program, a state audit found. One had been dead for four years before payments stopped.
Planes privados de Medicaid reciben millones, pero… ¿quién supervisa el negocio?
Las aseguradoras contratistas de Medicaid, que ofrecen servicios llamados de atención administrada, están en el banquillo: expertos cuestionan los servicios que ofrecen.
As Billions In Tax Dollars Flow To Private Medicaid Plans, Who’s Minding The Store?
Insurance companies profit from government contracts but are subject to little oversight of how they spend the money or care for patients. The expansion of Medicaid under the Affordable Care Act has only exacerbated the problem.
Paper Jam: California’s Medicaid Program Hits ‘Print’ When The Feds Need Info
Amid the buzz over apps and electronic medical records rescuing modern medicine, California’s Medicaid program still clings to 1970s-era technology. A reboot may cost half a billion dollars.
As California Hospitals Sweep Up Physician Practices, Patients See Higher Bills
A Health Affairs study quantifies the financial effects of such mergers on consumers and their insurers. The hospital industry and doctor practices say the consolidation leads to better coordination of care.
Hospital baja cuenta de $109,000 a $332… ¿qué pasa con las facturas sorpresa?
El hospital St. David’s Medical Center, en Austin, Texas, bajó una cuenta médica drásticamente. ¿Por qué fue tan alta en principio? ¿Qué pasa con las cuentas sorpresa?
The $109K Heart Attack Bill Is Down To $332. What About Other Surprise Bills?
“I don’t feel any consumer should have to go through this,” says Drew Calver, who faced a life-changing surprise bill from an Austin hospital after a heart attack last year. After attention as a “Bill of the Month” patient, he paid the hospital $332. But he worries about other patients with surprise bills.
¡Puñalada! Tienes seguro, pero igual debes pagar $109 mil por un ataque al corazón
Un maestro de Austin, Texas, quien sufrió un ataque cardíaco, tuvo que vivir una odisea cuando recibió una cuenta astronómica.
A Jolt To The Jugular! You’re Insured But Still Owe $109K For Your Heart Attack
A Texas teacher, 44, faces a “balance bill” of almost twice his annual salary for a heart attack he never expected to have.
A Black Eye For Blue Shield: Consumers Lash Out Over Coverage Lapses
California’s third-largest insurer faces anger from customers in the individual market who unexpectedly lost their insurance despite paying premiums faithfully. In its recently filed lawsuit, the company blamed a contractor for “egregious” billing problems.
Top Trump Health Official Takes Swipes At ACA, Single-Payer In Enemy Territory
After a San Francisco speech focused mostly on Medicare, Seema Verma fielded questions that underscored the administration’s differences with California on other key health care issues.
California’s ACA Rates To Rise 8.7% Next Year
The average increase in California is smaller than the double-digit hikes expected around the nation, due largely to a healthier mix of enrollees and more competition in its marketplace. Still, health insurance prices keep growing faster than wages and general inflation.
Insurers Fall Short In Catching And Reporting Medicaid Fraud, Inspectors Find
Medicaid has struggled for years with poor oversight and billions lost to improper payments. A new report finds that despite their fraud-fighting rhetoric, Medicaid managed-care companies are not as rigorous as they should be in ensuring the integrity of the Medicaid payment system.
Could California Shape The Fate Of The Affordable Care Act In November?
With the primary now over, health care may well emerge as an issue that helps voters distinguish between candidates for governor, attorney general and other offices in the general election.
California Hospital Giant Sutter Health Faces Heavy Backlash On Prices
In a case with possible national repercussions, the state’s attorney general has sued over alleged price gouging, and other legal and legislative challenges are afoot. Sutter is pushing back hard, denying anticompetitive behavior.
Study: Nearly Three-Quarters Of Commonly Used Medical Scopes Tainted By Bacteria
The ‘scary’ findings show a discouraging lack of progress in cleaning the devices, despite more vigorous efforts in the wake of deadly superbug outbreaks, experts say.
California Takes On Health Giant Over High Costs
The lawsuit is a bold move against Northern California’s dominant hospital chain, whose prices have drawn complaints for years. It has disputed such allegations in the past.
Calif. Bill Targets Profiteering In Addiction Treatment, Dialysis Industries
The legislation is intended to curb schemes in which some treatment providers sign patients up for private plans, pay their premiums and then rake in profits from inflated claims.
Thousands Mistakenly Enrolled During California’s Medicaid Expansion, Feds Find
California health officials do not dispute most of the findings, saying they have already made improvements in determining eligibility.