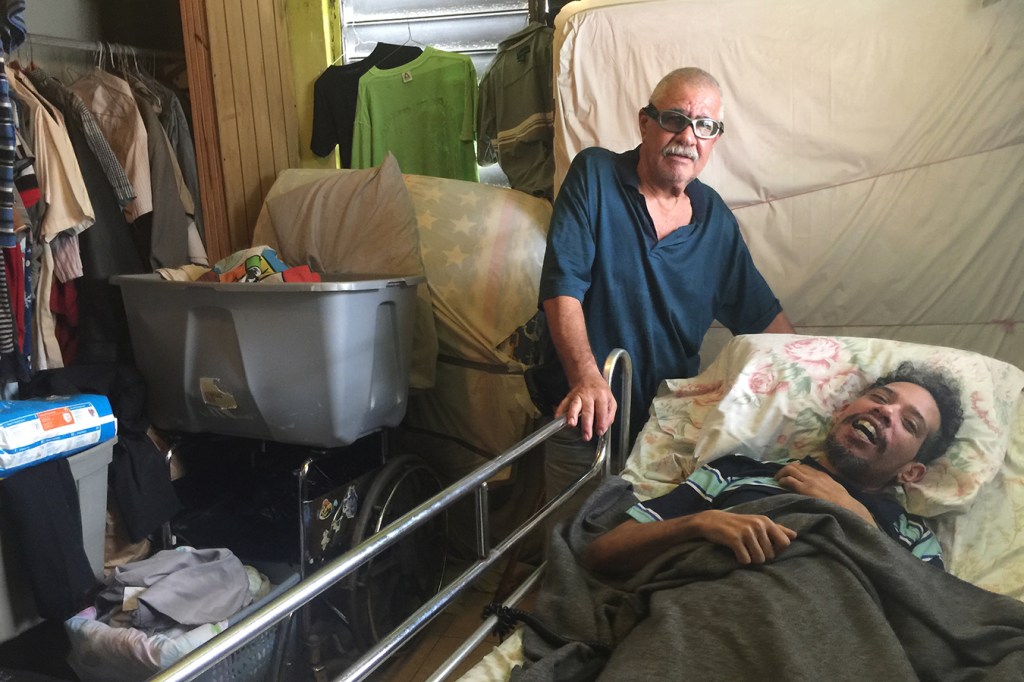
To reach the Martinez home in Puerto Rico’s central mountains, social worker Eileen Calderon steers around piles of dirt, treacherous potholes and power company trucks that block the road. Finally, she pulls up to a sagging, cement home, its roof done in by Hurricane Maria. Laundry hangs under a tarp, and a cat is tied to a leash outside the door.
Calderon, who is based in San Juan, and works for VarMed, a company that handles complex medical cases in Puerto Rico, has brought two colleagues — a nurse, Anamelia Velazquez, and a primary care physician, Dr. Carla Rossotti — to check in on Osvaldo Martinez and his son, Osvaldo Daniel Martinez.
Inside a darkened bedroom, the elder Martinez, a 67-year-old former star pitcher in the local baseball league, spoons rice and sausage into his son’s mouth. The younger Martinez lies in a hospital bed, his arms and fingers spasm and his eyes loll around in his head. He’s 37, born in Chicago, a former security guard.
Three years ago, after he and his father moved back to Puerto Rico from Illinois, the younger Martinez started showing early signs of multiple sclerosis. During the past year, his world became this room, then this bed.
His father points to the ceiling — leaking from the morning’s rain and covered in mold.
“All of this leaking that you can see came out because of the hurricane,” he said.
The power came back on in his house about a month ago, and the family has running water, so he is able to keep his son clean. The father carries a plastic basin into the bathroom and draws the water. Then, as he does a few times each day, he returns to the bedroom to bathe his adult son and gently change his diaper.
But Rossotti, whose company, VarMed, has been paid by the Puerto Rican government to help take care of the junior Martinez, said the younger man can’t yet get an appointment to see a neurologist to confirm his multiple sclerosis and start treatment. There is a chronic shortage of neurologists on the island, and those who remained after the storm have few slots in their schedules for Medicaid patients.
Calderon, the social worker, said she has been trying for a year to get an appointment for Martinez, but receptionist after receptionist tells her the neurologists they work for are taking no new patients. “We have a patient who was stable a year ago, and now he’s bedridden,” Rossotti said. “He hasn’t been able to get that neurologist evaluation.”

The roof of the Martinezes’ home in Cayey, Puerto Rico, was damaged in Hurricane Maria, leading to moisture and mold problems in the house. (Sarah Varney/KHN)
People here in Puerto Rico talk about life “before Maria” and life after. Accessing medical care here has always been a challenge, given the island’s chronic shortage of physicians and its unusual system for Medicaid — known as a block grant. The government provides a certain amount of money for each citizen in the program, no matter how great the needs are for care.
And for many of the island’s most vulnerable residents, like the Martinez family, the 2017 storm turned a challenge into a full-blown medical crisis that cannot be easily reversed. Since the turn of the century, a number of effective medicines that treat MS have come on the market, transforming the lives of people with the progressive disease, which can damage nerve conduction to anywhere in the body — the eye, the brain, the bladder, the legs. Treatment both helps slow progression and resolves symptoms. But it is less effective once damage to the nervous system is done.
The island’s financial crisis has sent doctors fleeing to the States during the past decade; Hurricane Maria added further fuel to that exodus. There is no exact accounting yet of just how many physicians have left the island, but from 2006 to 2016, the number of doctors dropped from 14,000 to 9,000, according to the Puerto Rico College of Physicians and Surgeons.
Nearly half of Puerto Ricans on the island rely on Medicaid — compared with around 20 percent of the population in the continental U.S. The territory’s government has long struggled to cover the costs of health care.
Currently, Molina Healthcare, a California-based company that provides insurance coverage to low-income people on Medicaid in Puerto Rico and elsewhere in the U.S., is ostensibly responsible for guaranteeing access to needed doctors.
A spokeswoman for Molina, Laura Murray, said the company cannot comment on the Martinez case, or that of any individual patient, because of privacy laws. But in a written statement, the company representative reported that it contracts with 41 neurologists in Puerto Rico’s eastern and southwestern regions, and meets “the network adequacy requirements in our contract.”
“However,” the statement continued, “we recognize that there is an island-wide shortage of physicians — particularly specialists — and we are proposing suggestions to [the Puerto Rican government] on how we could work together to remediate this.”
The island government recently announced that it will overhaul how Medicaid contracts are awarded.
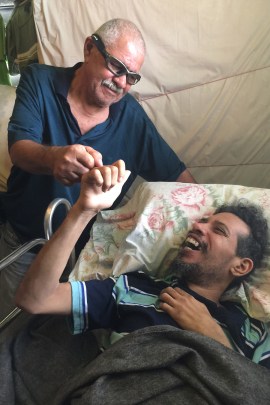
Osvaldo Martinez tends to his son, Osvaldo Daniel Martinez, whose world, over the past year, has slowly become one room, then one hospital bed. (Sarah Varney/KHN)
For now, the younger Martinez languishes — each day and night no different than the next, as the disease lays siege to his central nervous system, disrupting the vital connections between brain and body.
Without a confirmed diagnosis, he can’t get certain public disability benefits. And he isn’t getting medication for his condition or his pain; the agency Rossotti works for can only advocate for patients, not treat them.
The outward perseverance of father and son belies the true terror of their confinement. As the elder Martinez describes his son’s decline, tears come to his eyes; his son, who can understand everything, rolls on his side and begins to weep.
“I have to do all that needs to be done for him,” Martinez said. But he is not in good health himself, with severe arthritis and a painful bulge in his abdomen. During the months they went without power, he said, the hospital bed didn’t go up and down. He showed a photo of his arm — black-and-blue and swollen — from pressing against the metal bars of the bed as he leaned down to tend to his son.
But it’s his son’s withering away that pains him most.
“If something would happen to me,” the father said, clasping his hands together in prayer — “I don’t know.”