Trumpeting a landmark study released recently, hospitals around the country have started offering deeply discounted CT scans for smokers worried about lung cancer. But some experts question whether the strategy is a marketing ploy that could bring more harm than good.
St. Luke’s Hospital in Bethlehem, Pa., put out a single-page flyer with a headline that a “10-second scan could be life-saving” and a clip-out coupon for a $49 procedure. University Hospitals in Cleveland has a slick video on its website promoting its $99 scan, noting that some experts say this could be the “new hope needed to help save lives.”
The hospitals including the University of Pittsburgh Medical Center, Swedish Medical Center in Denver, Abbott Northwestern Hospital in Minneapolis, Rhode Island Hospital in Providence and Pomona Valley Hospital Medical Center in California say they are responding to the study by the National Cancer Institute. It found annual low-dose CT or computerized tomography screening of asymptomatic current or former smokers could cut the death rate from lung cancer by 20 percent by identifying the disease earlier than X-rays. The results were so striking that federal officials last November ended the study early to announce their findings.
The nearly decade-long study of more than 50,000 current and heavy smokers showed 354 lung cancer deaths had occurred among those with CT screening compared to 442 deaths among those who were screened only with an X-ray.
“The data is pretty compelling,” said Dr. Christopher Faber, medical director of the University of Pittsburgh Comprehensive Lung Center.
Most lung cancers are detected when they cause symptoms such as shortness of breath, by which time the disease is more likely to be advanced and less curable.
William Burfeind, a cardiothoracic surgeon at St. Luke’s, said the goal of offering the low-cost scans is to identify patients with earlier stages of lung cancer who have better chance of being cured by treatment. “The vast majority of my patients show up with stage 3 or 4 which is treatable, but rarely curable,” he said. “Once we learned the results of the national study, we felt compelled to offer this to our patients.”
Hospitals have marked down the CT scan which typically costs as much as $1,000 to help cash-paying customers. The test is not covered by Medicare or private insurers. Neither the American Cancer Society nor the U.S. Preventive Services Task Force, an independent panel of medical experts that examines the effectiveness of preventive tests, has recommended the screening, although both groups are studying the issue.
“You have to ask the question whose interests are being served here,” Dr. H. Gilbert Welch, a Dartmouth researcher who studies cancer screening, said of hospitals’ sales pitches. “Screening tests are a great way to recruit new patients that produce revenues with follow up biopsies and procedures.”
Welch and other experts worry that hospitals pushing the low-cost CT scans will focus on promoting the benefits of the lung cancer study to patients rather than warn about its costs and complications.
The biggest risk of the test is the possibility of false positives – a scan that finds an abnormality in the lung that turns out not to be cancer. Nearly one in four people in the national study had a false positive from the CT scans, which often can lead to a biopsy or other invasive procedures that carry their own health risks. Another concern is added radiation exposure from scans.
In addition, there are economic considerations: The results of the study suggest that more than 300 heavy smokers will need to be screened to prevent just one death from lung cancer over a five-year period.
Dr. Peter Bach, a researcher at Memorial Sloan-Kettering Cancer Center in New York who evaluates testing for the cancer society, said the hospitals offering the low-cost CT scans may be unfairly inducing patient to have a test they don’t need.
“It is troubling behavior,” he said. While some hospitals see a public health benefit to the testing, others may see it as a profit strategy. He notes the scans won’t make anyone better. “It’s not like they are giving away a flu shot or a nicotine patch,” he said.
Lung cancer is the leading cause of cancer-related deaths in the United States, with more than 94 million current or former smokers at elevated risk of the disease. Each year more than 222,000 people nationwide will be diagnosed with lung cancer and approximately 157,000 will die from the disease.
Leslie Greissing, 64, of Brunswick, Ohio, who had the test last month at University Hospitals in Cleveland, said she was attracted by the $99 price and the chance to catch a cancer before an X-ray. She said her doctor told her about the problem with false positives, but she decided to have the test anyway.
“As a heavy smoker on and off since I was 16, and my father died of lung cancer, I figured I was playing with a loaded deck,” she said. Her test was negative and she plans to have another scan next year.
This is not the first time the health industry has pushed screening tests before major medical groups endorsed their use. In the 1990s, hospitals promoted PSA blood tests as a screen for prostate cancer. But because of concern over false positives that could lead to high risk surgery, neither the cancer society nor the Preventive Services Task Force recommends the test.
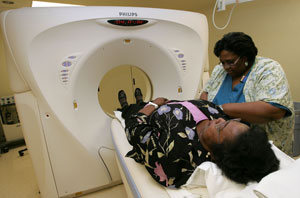
A low dose CT scan of the entire chest takes about 10 seconds. The technology uses a coordinated series of X-rays taken from many different angles to create a three-dimensional image allowing physicians to see smaller details than those that show up on a traditional X-ray. “This screening scan could make a real difference for people considered high-risk for developing lung cancer,” says Dr. Andrew Halpern, a St. Luke’s radiologist.
At St. Luke’s, 72 patients have taken advantage of the offer since early July. Fourteen of the patients have been recommended for follow-up screening in less than a year to check on abnormalities. Patients can only get the test with their doctor’s permission and they have to meet the same requirements as those in the national study: Current or former smokers age 55 to 74 who had an average of a pack a day habit.
Dr. David Midthun, a pulmonologist at the Mayo Clinic in Minnesota, said the national lung cancer screening study proves that on an individual basis the CT is a good idea. “We now have the evidence that the test is effective in mortality reduction,” he said.
But what’s not known is whether considering the cost of the test, it makes sense to recommend for millions of people. “We’re at the intersection now of what’s good public policy and individual patient decision making,” he said.






