Latest KFF Health News Stories
Nuevas normas de elegibilidad son un alivio financiero para casi 2 millones de personas en Medi-Cal
Este grupo se equiparará a los aproximadamente 12 millones de otros beneficiarios que no tienen límites de activos.
New Eligibility Rules Are a Financial Salve for Nearly 2 Million on Medi-Cal
Nearly 2 million Medi-Cal enrollees, mainly people who are aged, disabled, or in long-term care, can now accumulate savings and property without limitations and still qualify for the state’s health insurance program for low-income residents. They join an additional roughly 12 million enrollees who already had no asset limits.
A New Medicare Proposal Would Cover Training for Family Caregivers
The federal government is proposing having Medicare pay professionals to train family caregivers how to perform tasks like bathing and dressing their loved ones, and properly use medical equipment.
How to Negotiate With Resistant Aging Parents? Borrow These Tips From the Business World
Negotiation techniques can help health care providers and family caregivers find common ground with older adults who resist advice or support.
Readers and Tweeters Weigh Marijuana’s Merits Against Those of Alcohol or Opioids
KFF Health News gives readers a chance to comment on a recent batch of stories.
Remote Work: An Underestimated Benefit for Family Caregivers
The debate about whether employees should be required to return to the workplace has generally focused on commuting, convenience, and child care. A fourth C, caregiving, has rarely been mentioned.
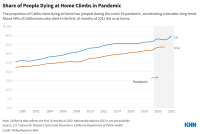
More Californians Are Dying at Home. Another Covid ‘New Normal’?
The proportion of Californians dying at home, rather than in a hospital or nursing home, accelerated during the pandemic, a trend that has outlasted the rigid lockdowns linked to the initial shift.
To Attract In-Home Caregivers, California Offers Paid Training — And Self-Care
Turnover ails a program that allows low-income people who are older or disabled to age in place. To attract new workers and improve retention, the state is paying caregivers to develop new skills.
Family Caregivers Find Support on #dementia TikTok
The TikTok hashtag “dementia” has billions of views. Caregivers of people with Alzheimer’s and other dementias have been using the site to swap tips and share the burdens of life with dementia.
To Families’ Dismay, Biden Nursing Home Reform Doesn’t View Them as Essential Caregivers
Relatives who often provide vital caregiving for nursing home residents say the lockdowns during the covid pandemic showed the need for family members to visit in person with their loved ones. About a dozen states have passed laws guaranteeing that right, and California is considering one.
Watch: Seniors Share How They’ve Made It Through the Pandemic
Nine seniors from across the country talk frankly about feeling alone and constrained, missing church, and family routines. They also share newfound hope and discoveries that arose from the crisis.
Pandemic-Fueled Shortages of Home Health Workers Strand Patients Without Necessary Care
Home health and hospice agencies are experiencing extreme worker shortages, which means they can’t provide services to all the patients seeking care.
When the Eye on Older Patients Is a Camera
High-tech tools ease caregivers’ stress but can raise sticky privacy questions and concerns about cost.
3 States Limit Nursing Home Profits in Bid to Improve Care
Following the devastating impact of covid-19 on nursing homes, state lawmakers want to be sure that government and private payments primarily go to improve care and staffing.
The number of Americans 65 and older is expected to nearly double in the next 40 years. Finding a way to provide and pay for the long-term health services they need won’t be easy.
Aiding Her Dying Husband, a Geriatrician Learns the Emotional and Physical Toll of Caregiving
When the covid pandemic hit, Dr. Rebecca Elon was thrust into a new role, primary caregiver for her severely ill husband and her elderly mother. “Reading about caregiving of this kind was one thing. Experiencing it was entirely different,” she says.
Biden Seeks $400 Billion to Buttress Long-Term Care. A Look at What’s at Stake.
Long-term care options are expensive and often out of reach for seniors and people with disabilities. The president has proposed a massive infusion of federal funding for home and community-based health services that advocates say will go a long way toward helping individuals and families.
KHN’s ‘What the Health?’: Health Care as Infrastructure
President Joe Biden’s infrastructure proposal includes items not traditionally considered “infrastructure,” including a $400 billion expansion of home and community-based services for seniors and people with disabilities, and a $50 billion effort to replace water pipes lined with lead. Meanwhile, the politics of covid-19 are turning to how or whether Americans will need to prove they’ve been vaccinated. Joanne Kenen of Politico, Tami Luhby of CNN and Sarah Karlin-Smith of the Pink Sheet join KHN’s Julie Rovner to discuss these issues and more. Plus, Rovner interviews KFF’s Mollyann Brodie about the KFF COVID-19 Vaccine Monitor.
Role Reversal: Covid Increases Ranks of Child Caregivers
Millions of teens and preteens help care for ill parents or grandparents. The pandemic has boosted their numbers while making it harder for them to get social and emotional support outside the home.
Roles invertidos: más cuidadores juveniles por covid
Millones de adolescentes y preadolescentes ayudan a cuidar de padres o abuelos enfermos. La pandemia ha aumentado el número y ha dificultado que obtengan apoyo social y emocional fuera del hogar.