A un año de recibir millones del gobierno federal, los estados apenas han comenzado a pensar cómo utilizar el dinero que recibieron para zanjar la desigualdad en salud que generó, y agravó, la pandemia.
States Have Yet to Spend Hundreds of Millions of Federal Dollars to Tackle Covid Health Disparities
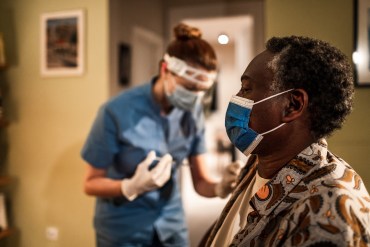
A year ago, the Centers for Disease Control and Prevention awarded states and local health departments $2.25 billion to help people of color and other populations at higher risk from covid. But a KHN review shows public health agencies across the country have been slow to spend it.
After the Pandemic Hit Nursing Homes Hard, California Lawmakers Push to Tighten Licensing Rules
Legislators are proposing an overhaul of California’s licensing system for nursing homes that would make it the most stringent in the country. They argue that disreputable and unlicensed owners and operators have harmed residents. The industry describes the proposed requirements as excessive.
Few Eligible Families Have Applied for Government Help to Pay for Covid Funerals
The Federal Emergency Management Agency will reimburse many families up to $9,000 in funeral expenses for loved ones who died of covid-19. But fewer than half of eligible families have applied, while others have run into application problems.
KHN’s ‘What the Health?’: The Invisible Pandemic
Covid cases are again climbing, but you wouldn’t know it from the behavior of public health and elected officials, much less the general public, all of whom seem to want to put the pandemic in the rearview mirror. Meanwhile, the fallout over the leaked Supreme Court draft opinion on abortion continues even as the Senate fails — again — to muster the votes to write abortion rights into law. Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico, Alice Miranda Ollstein of Politico, and Sandhya Raman of CQ Roll Call join KHN’s Julie Rovner to discuss these issues and more. Plus, for extra credit, the panelists suggest their favorite health policy stories of the week they think you should read, too.
¿Por qué más adultos mayores no reciben los refuerzos contra covid?
Según los CDC, aproximadamente 1 de cada 3 estadounidenses mayores de 65 años que completaron su ronda inicial de vacunación aún no han recibido la primera vacuna de refuerzo. Investigadores enfatizan que este grupo sigue teniendo el mayor riesgo de enfermedad grave y muerte por covid-19.
Is Paxlovid, the Covid Pill, Reaching Those Who Most Need It? The Government Won’t Say
Many public health workers are unable to see how many doses of Pfizer’s antiviral treatment are shipped to their communities and cannot tell whether vulnerable residents are filling prescriptions as often as their wealthier neighbors.
Why Won’t More Older Americans Get Their Covid Booster?
Approximately 1 in 3 Americans 65 and older who completed their initial vaccination round still have not received a first booster shot. The numbers dismay researchers, who say the lag has cost tens of thousands of lives.
Travel Nurses See Swift Change of Fortunes as Covid Money Runs Dry
Travel nurse contracts that were plentiful and paid the temporary nurses far more than hospital staff nurses are vanishing. Hospitals nationwide are turning their energies to recruiting full-time people.
Guía para entender a las subvariantes de ómicron
¿Qué tan diferentes son estas subvariantes entre sí? ¿Puede la infección por una subvariante proteger a alguien de la infección por otra? Y, ¿qué tan bien funcionan contra estas variantes las vacunas que se desarrollaron antes de la aparición de ómicron?
A Guide to Help You Keep Up With the Omicron Subvariants
How different are the seemingly endless stream of emerging omicron subvariants from one another and how protected are we?
Sweeping, Limited, or No Powers at All? What’s at Stake in the Mask Mandate Appeal
Dictionaries, public comments, and even an old court case that involved underwear pricing could play a role as the government appeals a ruling that sharply limits federal authority during pandemics.
KHN’s ‘What the Health?’: More Covid Complications for Congress
Congress is back in session, but covid diagnoses for Vice President Kamala Harris and two Democratic senators have temporarily left the Senate without a working majority to approve continued covid funding. Meanwhile, opponents of the Affordable Care Act have filed yet another lawsuit challenging a portion of the law, and we say goodbye to the late Sen. Orrin Hatch of Utah, who left a long legacy of health laws. Rachel Cohrs of STAT News, Anna Edney of Bloomberg News, and Rebecca Adams of KHN join KHN’s Julie Rovner to discuss these issues and more.
After Medical Bills Broke the Bank, This Family Headed to Mexico for Care
The Fierro family owed a Yuma, Arizona, hospital more than $7,000 for care given to mom and dad, so when a son dislocated his shoulder, they headed to Mexicali. The care was quick, good, and affordable.
La familia Fierro le debe a un hospital de Yuma, Arizona, más de $7,000 por dos situaciones médicas. Así que cuando uno de los hijos se dislocó el hombro, fueron a Mexicali, México. La atención fue rápida, buena y económica.
Despite Losing Federal Money, California Is Still Testing Uninsured Residents for Covid — For Now
Federal funding that paid for covid testing, treatment, and vaccines for uninsured people has run out. While some states struggle to make up the difference, California is relying on other state and local programs to continue free testing.
Judge’s Ruling on the CDC Mask Mandate Highlights the Limits of the Agency’s Power
A recent court decision that overturns one of the Centers for Disease Control and Prevention’s few pandemic rules — masks required on public transportation — spotlights how little power remains in federal hands to enforce public health protections.
Why Cheap, Older Drugs That Might Treat Covid Never Get Out of the Lab
The hydroxychloroquine and ivermectin fiascoes have soured many doctors on repurposing drugs for covid. A few inexpensive old drugs may be as good as some of the new antivirals, but they face complex obstacles to get to patients.
Better Ventilation Can Prevent Covid Spread. But Are Companies Paying Attention?
The research is clear that improving indoor air quality is an essential tool in stemming the spread of covid and a host of other diseases. But companies have to be willing to invest.
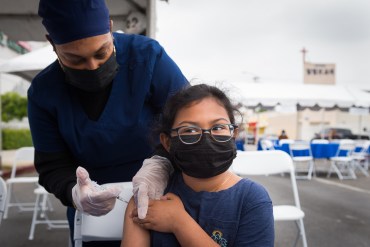
Se desploma la asistencia a eventos de vacunación contra covid en Los Ángeles
A medida que las infecciones por covid han ido disminuyendo, también lo ha hecho el interés en las vacunas, a pesar de que estas dosis son altamente efectivas para evitar enfermarse de gravedad y morir a causa del virus.