Latest KFF Health News Stories
Una decisión difícil: cuando los adultos mayores tienen que dejar de conducir
Los riesgos para los conductores mayores aumentan con la edad y el desarrollo de afecciones como la artritis, el glaucoma y el Parkinson. Y cuando ocurren accidentes, son más propensos a sufrir heridas graves o morir porque son físicamente más vulnerables.
Preparing to Hang Up the Car Keys as We Age
As cognitive skills erode with age, driving skills weaken, but an aging driver may not recognize that. Advance directives on driving are one way to handle this challenge.
Facing Financial Ruin as Costs Soar for Elder Care
The United States has no coherent system of long-term care, leading many to struggle to stay independent or rely on a patchwork of solutions.
Dementia Can Take a Toll on Financial Health, as Some Families Learn the Hard Way
People with dementia and their families often find themselves with few legal rights when dealing with financial scams or the mismanagement of their assets. Research reveals financial troubles can be both an early sign and a painful symptom of cognitive decline.
Dementia Care Programs Help, If Caregivers Can Find Them
Programs assisting people with dementia — and their caregivers — improve quality of life and care. But millions of unpaid family and friend caregivers may not know where or how to find help.
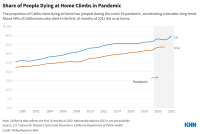
More Californians Are Dying at Home. Another Covid ‘New Normal’?
The proportion of Californians dying at home, rather than in a hospital or nursing home, accelerated during the pandemic, a trend that has outlasted the rigid lockdowns linked to the initial shift.
Ending Involuntary Commitments Would Shift Burden of Dementia Care to Strapped Communities
Health department officials anticipate having to transfer two dozen patients from the Montana State Hospital to another state-run facility if a bill to end involuntary commitments passes.
KFF Health News' 'What the Health?': GOP House Opens With Abortion Agenda
Leaders of the new Republican-led U.S. House kicked off their legislative agenda with two bills supported by anti-abortion groups. While neither is likely to become law, the move demonstrates how abortion will continue to be an issue in Washington. Meanwhile, as open enrollment for the Affordable Care Act nears its end in most states, the number of Americans covered by the plans hits a new high. Margot Sanger-Katz of The New York Times, Alice Miranda Ollstein of Politico, and Sarah Karlin-Smith of the Pink Sheet join KHN’s Julie Rovner to discuss these topics and more. Plus, for extra credit, the panelists recommend their favorite health policy stories of the week they think you should read, too.
Family Caregivers Find Support on #dementia TikTok
The TikTok hashtag “dementia” has billions of views. Caregivers of people with Alzheimer’s and other dementias have been using the site to swap tips and share the burdens of life with dementia.
Clearing Pollution Helps Clear the Fog of Aging — And May Cut the Risk of Dementia
Two studies published this year provide evidence that older adults’ cognitive health may benefit if air quality is improved.
Hospices Have Become Big Business for Private Equity Firms, Raising Concerns About End-of-Life Care
Private equity firms are seeing opportunities for profit in hospice care, once the domain of nonprofit organizations. The investment companies are transforming the industry — and might be jeopardizing patient care — in the process.
KHN’s ‘What the Health?’: Leaked Abortion Opinion Rocks Washington’s World
The unprecedented early leak of a Supreme Court draft opinion that would overturn the landmark abortion-rights ruling Roe v. Wade has heated the national abortion debate to boiling. Meanwhile, the FDA, after years of consideration, moves to ban menthol flavors in cigarettes and cigars. Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico, Shefali Luthra of the 19th, and Jessie Hellmann of CQ Roll Call join KHN’s Julie Rovner to discuss these issues and more. Plus, Rovner interviews KHN’s Paula Andalo, who wrote the latest KHN-NPR “Bill of the Month” episode about a family whose medical debt drove them to seek care south of the border.
Patients Divided Over Alzheimer’s Drug: Is It a ‘Risk I’m Willing to Take’ or Just a ‘Magic Pill’?
Medicare has proposed limiting coverage of Aduhelm, the costly new drug to treat Alzheimer’s disease, and several prominent groups representing patients and their families are pressing the program to make it more widely available. But among individuals facing the disease, the outlook is more nuanced.
Watch: Seniors Share How They’ve Made It Through the Pandemic
Nine seniors from across the country talk frankly about feeling alone and constrained, missing church, and family routines. They also share newfound hope and discoveries that arose from the crisis.
KHN’s ‘What the Health?’: Dealing With Drug Prices
Medicare officials tentatively plan to restrict the use of a controversial Alzheimer’s drug to only those patients participating in clinical trials, while the Department of Health and Human Services looks into lowering the monthly Medicare Part B premium. Meanwhile, covid confusion still reigns, as the Biden administration moves, belatedly, to make more masks and tests available. Joanne Kenen of Politico and the Johns Hopkins Bloomberg School of Public Health, Sarah Karlin-Smith of the Pink Sheet and Rachel Cohrs of Stat join KHN’s Julie Rovner to discuss these issues and more.
Wartime Trauma Hits Close to Home for Scholar of Dementia
The federal government is putting up $7.2 million for a study into the correlation between war trauma and dementia in Vietnamese immigrants. Oahn Meyer, an associate professor at the University of California-Davis who is leading the study, wonders whether her mother’s dementia is linked to trauma she suffered during the Vietnam War.
When the Eye on Older Patients Is a Camera
High-tech tools ease caregivers’ stress but can raise sticky privacy questions and concerns about cost.
Alzheimer’s Drug Targets People With Mild Cognitive Impairment. What Does That Mean?
The condition can be an early signal of Alzheimer’s disease, but not always. Other health concerns could be causing thinking or memory problems, and the new drug, Aduhelm, would not be appropriate for those patients.
Facing Headwinds on New Alzheimer’s Drug, Biogen Launches Controversial Campaign
The makers of Aduhelm, a drug approved last month despite concerns raised by experts about its effectiveness, have launched a website and ads designed to urge people who are worried about their memory to ask doctors about testing. But some health advocates say it is misleading because some memory loss with aging is normal.
Doctores explican pros y contras de recetar la nueva droga para el Alzheimer
Mientras médicos y expertos en políticas de salud debaten los méritos de Aduhelm, el primer fármaco para el Alzheimer aprobado en 18 años, los pacientes simplemente quieren saber: “¿me ayudará?”.