Latest KFF Health News Stories
Biden Is Right About $35 Insulin Cap but Exaggerates Prior Costs for Medicare Enrollees
Most Medicare enrollees likely were not paying a monthly average of $400 — as President Joe Biden stated — before the insulin cap took effect. However, because costs and other factors result in widely varying prices, some Medicare enrollees might have paid that much in a given month.
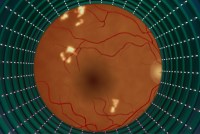
Programas de inteligencia artificial diagnostican retinopatía diabética en minutos
En medio de todo el revuelo en torno a la inteligencia artificial en la atención médica, la tecnología de exámenes de la vista está surgiendo como uno de los primeros casos de uso probados de diagnósticos basados en IA en un entorno clínico.
As AI Eye Exams Prove Their Worth, Lessons for Future Tech Emerge
With artificial intelligence in health care on the rise, eye screenings for diabetic retinopathy are emerging as one of the first proven use cases of AI-based diagnostics in a clinical setting.
An Arm and a Leg: Wait, Is Insulin Cheaper Now?
Did the price of insulin go down? It’s not quite that simple. On this episode of “An Arm and a Leg,” producer Emily Pisacreta explores recent changes to the cost of the diabetes medication.
States Target Health Insurers’ ‘Prior Authorization’ Red Tape
Doctors, patients, and hospitals have railed for years about the prior authorization processes that health insurers use to decide whether they’ll pay for patients’ drugs or medical procedures. The Biden administration announced a crackdown in January, but some state lawmakers are looking to go further.
These Patients Had to Lobby for Correct Diabetes Diagnoses. Was Their Race a Reason?
Adults who develop one autoimmune form of diabetes are often misdiagnosed with Type 2 diabetes. Those wrong diagnoses make it harder to get the appropriate medications and technology to manage their blood sugar. Many Black patients wonder if their race plays a role.
Beyond Insulin: Medi-Cal Expands Patient Access to Diabetes Supplies
California’s Medicaid program is making it easier for people with diabetes to obtain the supplies and equipment they need to manage their blood sugar, partly by relaxing preauthorization requirements that can cause life-threatening delays.
California Expands Paid Sick Days and Boosts Health Worker Wages
Gov. Gavin Newsom signed legislation expanding paid sick leave to five days, extending bereavement leave to miscarriages and failed adoptions, and approving an eventual $25-an-hour health care minimum wage. Still, in a possible sign of national ambitions, the Democrat vetoed free condoms in schools and refused to decriminalize psychedelic mushrooms.
New Weight Loss Drugs Carry High Price Tags and Lots of Questions for Seniors
Although nearly 40% of Americans 60 and older are obese, Medicare doesn’t cover weight loss medications. Meanwhile, studies haven’t thoroughly examined new drugs’ impact on older adults.
Many People Living in the ‘Diabetes Belt’ Are Plagued With Medical Debt
The “Diabetes Belt,” as defined by the Centers for Disease Control and Prevention, comprises 644 mostly Southern counties where diabetes rates are high. Of those counties, KFF Health News and NPR found, more than half also have high levels of medical debt.
Redes sociales alimentan obsesión por las drogas para bajar de peso, sin hablar de riesgos
La competencia para hacerse con un mercado que podría valer $100.000 millones al año, solo para los fabricantes de medicamentos, ha desencadenado una ola de publicidad que preocupa a las autoridades sanitarias y médicos de todo el mundo.
Social Media Is Fueling Enthusiasm for New Weight Loss Drugs. Are Regulators Watching?
Online platforms are overflowing with testimonials for GLP-1s. The drugs show promise for inducing weight loss, but many aren’t FDA-approved for that use.
KFF Health News' 'What the Health?': The Confusing Fate of the Abortion Pill
The legality and availability of the abortion pill mifepristone is in question after a federal judge in Texas canceled the FDA’s approval of the first drug used in the two-drug medication abortion regimen. A 5th Circuit Court of Appeals panel overruled that decision in part, saying the pill should remain available, but only under the onerous restrictions in place before 2016. Meanwhile, another federal judge in Washington state issued a ruling in a separate case that conflicts with the Texas decision, ordering the FDA not to roll back any of its restrictions on the drug. Victoria Knight of Axios, Shefali Luthra of The 19th, and Sarah Karlin-Smith of the Pink Sheet join KFF Health News chief Washington correspondent Julie Rovner to discuss these issues and more.
Montana May Require Insurers to Cover Monitoring Devices for Diabetes
Montana is one of several states considering expanding coverage of continuous glucose monitors, but insurance companies and some providers argue that not all people with diabetes need them.
Journalists Delve Into Insulin Costs and Prior Authorization Policy
KHN and California Healthline staff made the rounds on national and local media this week to discuss their stories. Here’s a collection of their appearances.
Fresh Produce Is an Increasingly Popular Prescription for Chronically Ill Patients
Fresh produce prescription programs are getting a boost in Montana as a way of helping people with chronic conditions such as diabetes and high blood pressure. The approach may be a model for other rural states to promote healthy eating in food deserts.
California Picks Generic Drug Company Civica to Produce Low-Cost Insulin
Gov. Gavin Newsom, who blasted pharmaceutical companies for gouging Californians, is moving ahead with state-branded insulin. He’s also eyeing other generic drugs.
California eligió a la compañía de genéricos Civica para producir insulina de bajo costo
Civica está desarrollando tres tipos de insulina genérica, conocida como biosimilar, que estarán disponibles tanto en viales como en plumas inyectables, a un costo de entre $30 y $55.
La insulina representa lo perverso del sistema sanitario estadounidense, ya que los precios de venta de este medicamento centenario, del que dependen 8,4 millones de estadounidenses para sobrevivir, se quintuplicaron en dos décadas.
Why Does Insulin Cost So Much? Big Pharma Isn’t the Only Player Driving Prices
Big Pharma may be moving on from squeezing diabetes patients on insulin prices, but it’s the arbitrators that jack up prices for those who can least afford them.