Latest KFF Health News Stories
Mandatory Reporting Laws Meant To Protect Children Get Another Look
The state is looking at ways to weed out false reporting of child abuse and neglect as the number of reports reaches a record high.
Genetics Studies Have a Diversity Problem That Researchers Struggle To Fix
Researchers in Charleston, South Carolina, are trying to build a DNA database of 100,000 people to better understand how genetics affects health risks. But they’re struggling to recruit enough Black participants.
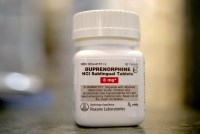
Para frenar las muertes por fentanilo, reparten kits para revertir las sobredosis puerta por puerta
En Philadelphia, funcionarios esperan que este enfoque proactivo transforme a la naloxona en un artículo que esté en los botiquines, para evitar que las personas mueran por sobredosis, especialmente los residentes negros.
To Stop Fentanyl Deaths in Philadelphia, Knocking on Doors and Handing Out Overdose Kits
Facing widening racial disparities in overdose deaths, Philadelphia officials are sending workers and volunteers to knock on doors across the city, aiming to equip households with naloxone and other drug overdose prevention supplies. City officials hope a proactive approach will normalize naloxone as an everyday item in people’s medicine cabinets and prevent overdoses, especially among Black residents.
Journalists Assess the Risks of Bird Flu and the Impacts of Medicaid ‘Unwinding’
KFF Health News and California Healthline staff made the rounds on national and local media this week to discuss their stories. Here’s a collection of their appearances.
End of Internet Subsidies for Low-Income Households Threatens Telehealth Access
A federal program that helped pay for more than 23 million low-income households’ internet access runs out of money soon. The end of the subsidy launched earlier in the pandemic could have profound impacts on health care access.
Rapid Rise in Syphilis Hits Native Americans Hardest
With U.S. syphilis rates climbing to the worst level in seven decades, public health experts and the federal Indian Health Service are scrambling to detect and treat the disease in Native American communities, where babies are infected at a higher rate than in any other demographic.
Encuesta revela que persiste la discriminación racial en la atención médica
Casi la mitad de los pacientes hispanos, los Indio americanos y los nativos de Alaska sienten que no se los respeta.
Many People of Color Worry Good Health Care Is Tied to Their Appearance
Many people from racial and ethnic minority groups brace themselves for insults and judgments before medical appointments, according to a new survey of patients that reaffirms the prevalence of racial discrimination in the U.S. health system.
El daño colateral de la crisis de Medicaid: miles están perdiendo beneficios de alimentos
Las familias de bajos ingresos que necesitan servicios como ayuda alimentaria y dinero en efectivo, se ven afectadas por la carrera burocrática para determinar si decenas de millones de personas aún califican para Medicaid.
Medicaid ‘Unwinding’ Makes Other Public Assistance Harder to Get
The bottleneck caused by states’ reevaluation of Medicaid enrollees has swept up low-income families that rely on other safety-net services.
‘Everybody in This Community Has a Gun’: How Oakland Lost Its Grip on Gun Violence
A few years ago, Oakland won national acclaim for slashing gun-related crimes. Then the covid-19 pandemic tore through poor neighborhoods, and the murder of George Floyd fueled distrust in police. With guns readily available, violent crime has once again skyrocketed, leaving the community struggling to contain it.
Backlash to Affirmative Action Hits Pioneering Maternal Health Program for Black Women
A San Francisco program offers a $1,000-a-month stipend for pregnant Black and Pacific Islander women, part of an effort to address severe racial disparities in maternal health. But conservative groups have sued to shut down the Abundant Birth Project, part of a national backlash against affirmative action in health care.
Evolving Overdose Crisis Shakes Previously Effective Treatments
The prevalence of synthetic drugs is undercutting a previously effective and widely embraced opioid use disorder treatment tactic. Now, the model pioneered in Vermont a decade ago and adopted at sites nationwide, especially in hard-to-reach rural areas, is being forced to evolve.
Health Care ‘Game-Changer’? Feds Boost Care for Homeless Americans
This month, the federal government started paying for treatments delivered outside hospitals and clinics, expanding funding for “street medicine” teams that treat homeless patients. California led the way on the change, which could help sick and vulnerable patients get healthy, sober, and, in some cases, into housing.
Listen: Inroads for Women in California’s Health Care Workforce
KFF Health News senior correspondent Angela Hart leads a discussion about the role women play as California grapples with a shortage of health care providers.
More Cities Address ‘Shade Deserts’ as Extreme Heat Triggers Health Issues
Where trees are growing — and who has access to their shade — affects health and well-being, especially in one of the hottest states in the country.
Dangers and Deaths Around Black Pregnancies Seen as a ‘Completely Preventable’ Health Crisis
Studies show that high rates of Black fetal and infant deaths are largely preventable — and part of systemic failures that contribute to disproportionately high Black maternal mortality rates.
Life in a Rural ‘Ambulance Desert’ Means Sometimes Help Isn’t on the Way
No local hospital and anemic ambulance services mean residents in rural Pickens County, Alabama, are thrown into perilous situations when they have medical emergencies. It’s a kind of medical care roulette that has become a fact of life for rural Americans who live in ambulance deserts.
Doctors Advocate Fresh Efforts to Combat Chagas Disease, a Silent Killer
Chagas disease, caused by a parasite, affects people primarily in rural Latin America. But an estimated 300,000 residents of the U.S. have the disease, which can cause serious heart problems. Patient advocates call for much more aggressive efforts to fight it.