Latest KFF Health News Stories
Desde el 1 de enero, California se sumó a otros 45 estados y al Distrito de Columbia con leyes que permiten a una persona tomar decisiones en nombre de un paciente, incluso si no estaba autorizada por el paciente antes de que ocurriera la situación médica.
California Requires Hospitals to Turn to a Patient’s Next of Kin, Closing a Longtime Loophole
A state law establishes a list of representatives who can make medical decisions for patients unable to convey their wishes. California is late to making the change; 45 other states and the District of Columbia already have next-of-kin laws.
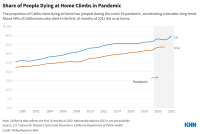
More Californians Are Dying at Home. Another Covid ‘New Normal’?
The proportion of Californians dying at home, rather than in a hospital or nursing home, accelerated during the pandemic, a trend that has outlasted the rigid lockdowns linked to the initial shift.
‘Science Friday’ and KHN: Examining Medicine’s Definition of Death Informs the Abortion Debate
Why is it so hard to agree when life begins? As state abortion laws define it, science, politics, and religion are clashing. KHN’s Sarah Varney shared her reporting with the “Science Friday” radio program.
When Does Life Begin? As State Laws Define It, Science, Politics, and Religion Clash
For decades, the U.S. medical establishment has adhered to a legally recognized standard for brain death, one embraced by most states. Why is a uniform clinical standard for the inception of human life proving so elusive?
Hospices Have Become Big Business for Private Equity Firms, Raising Concerns About End-of-Life Care
Private equity firms are seeing opportunities for profit in hospice care, once the domain of nonprofit organizations. The investment companies are transforming the industry — and might be jeopardizing patient care — in the process.
Black-Owned Hospice Seeks to Bring Greater Ease in Dying to Black Families
National data shows that Black Medicare patients and their families are not making the move to comfort care as often as white patients are. Experts speculate it’s related to spiritual beliefs and widespread mistrust in the medical system due to decades of discrimination.
A New Paradigm Is Needed: Top Experts Question the Value of Advance Care Planning
Prominent researchers say the nationwide effort to get people to spell out how they want to be treated as they die is not improving patients’ care.
Nueva ley de California facilita el proceso de ayuda para morir
Una modificación a la ley vigente reduce el tiempo entre las peticiones necesarias para obtener los medicamentos para terminar con la vida. También protege más a los pacientes.
New California Law Eases Aid-in-Dying Process
Nearly 2,000 terminally ill Californians have used a 2015 law to end their lives with a doctor’s assistance. A revision of the law will make it easier to do so.
Aiding Her Dying Husband, a Geriatrician Learns the Emotional and Physical Toll of Caregiving
When the covid pandemic hit, Dr. Rebecca Elon was thrust into a new role, primary caregiver for her severely ill husband and her elderly mother. “Reading about caregiving of this kind was one thing. Experiencing it was entirely different,” she says.
Getting a Prescription to Die Remains Tricky Even as Aid-in-Dying Bills Gain Momentum
Access to physician-assisted death is expanding across the U.S., but the procedure remains in Montana’s legal gray zone more than a decade after the state Supreme Court ruled physicians could use a dying patient’s consent as a defense.
New Legal Push Aims to Speed Magic Mushrooms to Dying Patients
A proposal in Washington state would use right-to-try laws to allow terminally ill patients access to psilocybin — the famed magic mushrooms of America’s psychedelic ’60s — to ease depression and anxiety.
We Put Off Planning, Until My Father-in-Law’s Medical Crisis Took Us by Surprise
Although the family patriarch did not face a life-threatening emergency, the episode was a reminder that you have to prepare for a real crisis.
Bereaved Families Are ‘the Secondary Victims of COVID-19’
New research suggests the pandemic’s deaths are taking an enormous toll on surviving family members and worrisome ripple effects may linger for years.
Families of Health Workers Killed by COVID Fight for Denied Workers’ Comp Benefits
Attorneys say some state workers’ compensation laws leave workers and families struggling for benefits after a COVID illness or death.
‘I Couldn’t Let Her Be Alone’: A Peaceful Death Amid the COVID Scourge
For three years, staffers at UCLA Health have been quietly fulfilling final wishes for dying patients in the intensive care unit. Amid the isolating forces of the pandemic, their work has become all the more meaningful.
My Mother Died Of The Coronavirus. It’s Time She Was Counted.
Not having an accurate, honest, nationwide way to tally COVID-19 cases will only add to the current tragedy.
Bringing ‘Poogie’ Home: Hospice In The Time Of COVID-19
One family took up the challenge of taking their mother, who had serious medical problems and the coronavirus, from the hospital to die at home. But because of the risk of infection, home hospice can be a daunting experience.
Palliative Care Helped Family Face ‘The Awful, Awful Truth’
Elizabeth and Robert Mar would have celebrated 50 years of marriage in August. Instead, they died within a day of each other. Their two very different deaths illustrate how palliative care is changing to help patients and families cope with the coronavirus pandemic.