California Offers a Lifeline for Medical Residents Who Can’t Find Abortion Training
Abortion restrictions in 18 states have curtailed access to training in skills that doctors say are critical for OB-GYN specialists and others. A new California law makes it easier for out-of-state doctors to get experience in reproductive medicine.
¿Pueden los médicos de familia salvar a las zonas rurales de la crisis de obstetras?
El número de bebés que murieron antes de cumplir su primer año aumentó el año pasado; y más de la mitad de los condados rurales no tienen servicios hospitalarios para partos.
Can Family Doctors Deliver Rural America From Its Maternal Health Crisis?
Family medicine doctors already deliver most of rural America’s babies, and efforts to train more in obstetrics care are seen as a way to cope with labor and delivery unit closures.
Mental Health Courts Can Struggle to Fulfill Decades-Old Promise
Mental health courts have been touted as a means to help reduce the flow of people with mental illness into jails and prisons. But the specialized diversion programs can struggle to live up to that promise, and some say they’re a bad investment.
‘I Am Just Waiting to Die’: Social Security Clawbacks Drive Some Into Homelessness
The Social Security Administration is reclaiming billions of dollars in alleged overpayments from some of the nation’s poorest and most vulnerable, leaving some people homeless or struggling to stay in housing, beneficiaries and advocates say.
Health Care Is Front and Center as DeSantis and Newsom Go Mano a Mano
Florida’s Republican Gov. Ron DeSantis and California’s Democratic Gov. Gavin Newsom will square off in a first-of-its-kind debate on Nov. 30. KFF Health News compared the political rivals’ health care positions, showing how their policies have helped — or hindered — the health of their states’ residents.
Journalists Delve Into Open Enrollment, School Nurse Shortages, and More
KFF Health News and California Healthline staff made the rounds on national and local media this week to discuss their stories. Here’s a collection of their appearances.
Most States Ban Shackling Pregnant Women in Custody, Yet Many Report Being Restrained
Advocates for pregnant people in police custody say repeated incidents show prohibitions on handcuffs and other restraints are little more than lip service.
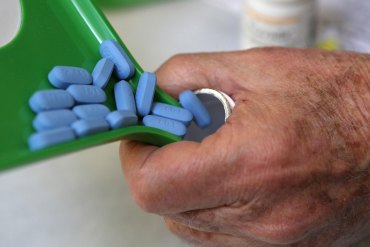
US to Cover HIV Prevention Drugs for Older Americans to Stem Spread of the Virus
The government has proposed that Medicare fully cover preexposure prophylaxis drugs that prevent HIV, a change that could help America catch up with nations in Europe and Africa that are on track to end new infections decades before the U.S. under its current approach.
Prevención del VIH: proponen que Medicare cubra PrEP para adultos mayores
Según el plan de la administración Biden, Medicare cubriría el costo total de los medicamentos de profilaxis previa a la exposición, que previenen la transmisión del VIH.
Tiny, Rural Hospitals Feel the Pinch as Medicare Advantage Plans Grow
More than half of seniors are enrolled in private Medicare Advantage plans instead of traditional Medicare. Rural enrollment has increased fourfold and many small-town hospitals say that threatens their viability.
Quick Genetic Test Offers Hope for Sick, Undiagnosed Kids. But Few Insurers Offer to Pay.
A new, rapid genetic test shows promise in increasing diagnoses and improving treatment for some children with rare genetic conditions. Many insurers won’t cover it, but Florida’s Medicaid program is among those that see benefits — and, potentially, savings.
Pruebas genéticas rápidas a bebés pueden salvar vidas, pero muchas aseguradoras no las cubren
Que Medicaid cubra la prueba puede expandir significativamente el acceso para los bebés; el programa de salud federal gerenciado por los estados que asegura a las familias de bajos ingresos y que cubre a más del 40% de los niños en su primer año de vida.
PrEP, a Key HIV Prevention Tool, Isn’t Reaching Black Women
New HIV infections occur disproportionately among Black women, but exclusionary marketing, fewer treatment options, and provider wariness have limited uptake of preexposure prophylaxis, or PrEP, drugs, which reduce the risk of contracting the virus.
Journalists Track Opioid Settlement Cash and New Fees for Emailing Your Doctor
KFF Health News and California Healthline staff made the rounds on national and local media this week to discuss their stories. Here’s a collection of their appearances.
As Covid Infections Rise, Nursing Homes Are Still Waiting for Vaccines
“People want covid-19 to be in the rearview mirror,” one nursing home official says. Faced with a slow rollout of the updated covid vaccines, and without state mandates for workers to get vaccinated, most skilled nursing facilities are relying on persuasion to boost vaccination rates among staff and residents.
Social Security Overpays Billions to People, Many on Disability. Then It Demands the Money Back.
Beneficiaries in five states described what happened when they received letters calling on them to return overpayments that can reach tens of thousands of dollars or more.
Dr. Google conoce a Dr. ChatGPT: la inteligencia artificial empieza a impactar en la salud
La sintaxis fluida, el tono de autoridad y la destreza de la IA generativa han atraído a todos los sectores de la sociedad, y algunos comparan su impacto futuro con el de la propia Internet.
Watch: In Emergencies, First Comes the Ambulance. Then Comes the Bill.
This installment of InvestigateTV and KFF Health News’ “Costly Care” series delves into the lack of cost protections for patients who find themselves on the hook for an emergency ground ambulance ride.
‘Dr. Google’ Meets Its Match: Dr. ChatGPT
With the rise of generative AI, people who once turned to “Dr. Google” to check on medical symptoms are now turning to chatbots. Researchers say the bots are often more accurate, but urge caution in the absence of any regulations.