Latest KFF Health News Stories
California Is Investing $500M in Therapy Apps for Youth. Advocates Fear It Won’t Pay Off.
California launched two teletherapy apps as part of the governor’s $500 million foray into health technology with private companies. But the rollout has been so slow that one company has yet to make its app available on Android, and social workers worry youths who need clinical care won’t get referrals.
KFF Health News' 'What the Health?': Abortion — Again — At the Supreme Court
For the second time in as many months, the Supreme Court heard arguments in an abortion case. This time, the justices are being asked to decide whether a federal law that requires emergency care in hospitals can trump Idaho’s near-total abortion ban. Meanwhile, the federal government, for the first time, will require minimum staffing standards for nursing homes. Alice Miranda Ollstein of Politico, Tami Luhby of CNN, and Joanne Kenen of Johns Hopkins University and Politico Magazine join KFF Health News’ Julie Rovner to discuss these stories and more. Plus, for “extra credit,” the panelists suggest health policy stories they read this week they think you should read, too.
FTC Chief Says Tech Advancements Risk Health Care Price Fixing
Technological advances including the widespread use of algorithms make it easier for companies to fix prices without explicitly coordinating, Lina Khan said at a KFF event.
Medical Providers Still Grappling With UnitedHealth Cyberattack: ‘More Devastating Than Covid’
Medical providers say they’re still coping with the Change Healthcare cyberattack disclosed in February even though parent company UnitedHealth Group reported that much is back to normal and its revenue is up over last year.
Too Big To Fail? Now It’s ‘Too Big To Hack’
Congress this week had the chance to formally air grievances over the cascading consequences of the Change Healthcare cyberattack, and lawmakers from both major parties agreed on one culprit: consolidation in health care. Plus, about a year after states began stripping people from their Medicaid rolls, a new survey shows nearly a quarter of adults who were disenrolled are now uninsured. Jessie Hellmann of CQ Roll Call, Sarah Karlin-Smith of the Pink Sheet, and Lauren Weber of The Washington Post join KFF Health News’ Mary Agnes Carey to discuss these stories and more. Also this week, KFF Health News’ Julie Rovner interviews Caroline Pearson of the Peterson Health Technology Institute.
Congress Likely to Kick the Can on Covid-Era Telehealth Policies
With an end-of-year deadline and a presidential election approaching, payment rules that fueled rapid expansion of telehealth in the United States face a last-minute congressional decision.
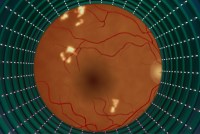
Programas de inteligencia artificial diagnostican retinopatía diabética en minutos
En medio de todo el revuelo en torno a la inteligencia artificial en la atención médica, la tecnología de exámenes de la vista está surgiendo como uno de los primeros casos de uso probados de diagnósticos basados en IA en un entorno clínico.
As AI Eye Exams Prove Their Worth, Lessons for Future Tech Emerge
With artificial intelligence in health care on the rise, eye screenings for diabetic retinopathy are emerging as one of the first proven use cases of AI-based diagnostics in a clinical setting.
Under Fire for Massive Health System Hack, Biden Team Leans on Insurers
The Biden administration has hit on a strategy to deal with the massive, industry-paralyzing cyberattack on a UnitedHealth Group unit: pressuring insurers to fix it. Federal officials have been in constant conversation with senior leaders at UnitedHealth and across the industry, including at a Monday meeting where Department of Health and Human Services and White […]
Covid and Medicare Payments Spark Remote Patient Monitoring Boom
Demand for help monitoring patients’ vital signs remotely has taken off since a Medicare change in 2019. Dozens of companies now push the service to help overburdened primary care doctors — and as a revenue stream. But some policy experts say its growth has outpaced oversight and evidence of effectiveness.
KFF Health News' 'What the Health?': Maybe It’s a Health Care Election After All
Health care wasn’t expected to be a major theme for this year’s elections. But as President Joe Biden and former President Donald Trump secured their respective party nominations this week, the future of both Medicare and the Affordable Care Act appears to be up for debate. Meanwhile, the cyberattack of the UnitedHealth Group subsidiary Change Healthcare continues to do damage to the companies’ finances with no quick end in sight. Margot Sanger-Katz of The New York Times, Anna Edney of Bloomberg News, and Joanne Kenen of Johns Hopkins University and Politico Magazine join KFF Health News’ Julie Rovner to discuss these issues and more. Also this week, Rovner interviews Kelly Henning of Bloomberg Philanthropies about a new, four-part documentary series on the history of public health, “The Invisible Shield.” Plus, for “extra credit” the panelists suggest health policy stories they read this week that they think you should read, too.
Biden Team, UnitedHealth Struggle to Restore Paralyzed Billing Systems After Cyberattack
The cyberattack on a unit of UnitedHealth Group’s Optum division is the worst on the health care industry in U.S. history, hospitals say. Providers struggling to get paid for care say the response by the insurer and the Biden administration has been inadequate.
Statistical Models vs. Front-Line Workers: Who Knows Best How to Spend Opioid Settlement Cash?
A mathematical model designed to direct spending of opioid settlement funds is at the center of a debate over whether to invest in technology to guide long-term decisions or focus on the immediate needs of people in addiction.
KFF Health News' 'What the Health?': Alabama’s IVF Ruling Still Making Waves
Lawmakers in Congress and state legislatures are scrambling to react to the ruling by the Alabama Supreme Court that frozen embryos created for in vitro fertilization are legally children. Abortion opponents are divided among themselves, with some supporting full “personhood” for fertilized eggs, while others support IVF as a moral way to have children. Rachel Cohrs of Stat, Riley Griffin of Bloomberg News, and Joanne Kenen of the Johns Hopkins University schools of nursing and public health and Politico Magazine join KFF Health News’ Julie Rovner to discuss these issues and more. Also this week, Rovner interviews University of Pittsburgh law professor Greer Donley, who explains how a 150-year-old anti-vice law that’s still on the books could be used to ban abortion nationwide. Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too.
Hacking at UnitedHealth Unit Cripples a Swath of the US Health System: What to Know
Change Healthcare, a firm recently bought by insurance giant UnitedHealth Group, reportedly suffered a cyberattack. The company processes 14 billion transactions annually, including payments and requests for insurance authorizations.
Washington intenta ponerse al día con el uso de la inteligencia artificial en el sector de salud
El impacto de la IA en el sector de salud ya es generalizado. La Administración de Alimentos y Medicamentos ha aprobado unos 692 productos de inteligencia artificial.
‘Behind the Times’: Washington Tries to Catch Up With AI’s Use in Health Care
Lawmakers and regulators are trying to understand how AI is changing health care and how it should be regulated. The industry fears overreach.
Senators Weigh Whether Health Care AI Needs a Leash
The Senate Finance Committee contemplated the future yesterday: artificial intelligence and its potential applications to health care. And it turns out the future looks an awful lot like the past and present: Democrats want regulations. And the industry wants money. “There are a lot of reasons to be optimistic,” Finance Committee Chair Ron Wyden (D-Ore.) […]
What the Health Care Sector Was Selling at the J.P. Morgan Confab
When bankers and investors flocked to San Francisco for the largest gathering of health care industry investors, the buzz was all about artificial intelligence, the next hit weight-loss drug, and new opportunities to make money through nonprofit hospitals.
Mamografías que usan inteligencia artificial cuestan dinero extra… pero, ¿vale la pena?
Este software puede identificar patrones y anomalías que los radiólogos humanos podrían pasar por alto. Pero no es el estándar de atención.