Latest KFF Health News Stories
Mandatory Reporting Laws Meant To Protect Children Get Another Look
The state is looking at ways to weed out false reporting of child abuse and neglect as the number of reports reaches a record high.
Medical Providers Still Grappling With UnitedHealth Cyberattack: ‘More Devastating Than Covid’
Medical providers say they’re still coping with the Change Healthcare cyberattack disclosed in February even though parent company UnitedHealth Group reported that much is back to normal and its revenue is up over last year.
Swap Funds or Add Services? Use of Opioid Settlement Cash Sparks Strong Disagreements
The national opioid settlements don’t prohibit using money for initiatives already supported by other means, but doing so could dilute the impact.
Doctors Take On Dental Duties to Reach Low-Income and Uninsured Patients
More doctors are integrating oral health care into their practices, filling a need in America’s dental deserts.
Médicos de atención primaria asumen tareas de dentista para ayudar a pacientes vulnerables
En Denver, la inestabilidad de la vivienda, las barreras del idioma, la falta de transporte y el “costo astronómico” de la odontología sin seguro hacen que la atención dental sea inaccesible para muchos nuevos inmigrantes.
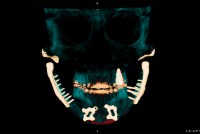
The Horrors of TMJ: Chronic Pain, Metal Jaws, and Futile Treatments
TMJ disorders affect as many as 1 in 10 Americans and yet remain poorly understood and ineffectively treated. Many common treatments used by dentists lack scientific evidence.
Medical Debt Affects Much of America, but Colorado Immigrants Are Hit Especially Hard
Colorado is ahead of the curve on policies to prevent medical debt, but the gap between the debt load in places inhabited primarily by people of color versus non-Hispanic white residents is greater than the national average.
La deuda médica afecta a gran parte de EE.UU., pero en especial a inmigrantes en Colorado
Las luchas del área reflejan una paradoja sobre Colorado. En general, la carga de deuda médica del estado es más baja que la de la mayoría. Pero las disparidades raciales y étnicas son más amplias.
Your Doctor or Your Insurer? Little-Known Rules May Ease the Choice in Medicare Advantage
Disputes between hospitals and Medicare Advantage plans are leading to entire hospital systems suddenly leaving insurance networks. Patients are left stuck in the middle, choosing between their doctors and their insurance plan. There’s a way out.
La nueva ola de propuestas estatales, impulsada por familias que perdieron familiares después de enfrentamientos con la policía, marca un paso importante para desterrar un término que los críticos dicen que incita a la policía a usar fuerza letal en exceso.
Health Workers Fear It’s Profits Before Protection as CDC Revisits Airborne Transmission
Four years since the covid pandemic emerged, health care workers want rules that protect them during outbreaks. They worry the CDC is repeating past mistakes as it develops a crucial set of guidelines for hospitals, nursing homes, prisons, and other facilities that provide health care.
Covid and Medicare Payments Spark Remote Patient Monitoring Boom
Demand for help monitoring patients’ vital signs remotely has taken off since a Medicare change in 2019. Dozens of companies now push the service to help overburdened primary care doctors — and as a revenue stream. But some policy experts say its growth has outpaced oversight and evidence of effectiveness.
As More States Target Disavowed ‘Excited Delirium’ Diagnosis, Police Groups Push Back
After California passed the first law in the nation to limit the disavowed term “excited delirium,” bills in other states are being introduced to help end use of the diagnosis. But momentum is being met with resistance from law enforcement and first responder groups, who cite free speech.
California Pushes to Expand the Universe of Abortion Care Providers
A new California law allows trained physician assistants, also called physician associates, to perform first-trimester abortions without the presence of a supervising doctor. The legislation is part of a broader effort by the state to expand access to abortion care, especially in rural areas. Some doctor groups are wary.
Si eres pobre, un tratamiento de fertilidad suele ser un sueño inaccesible
Pero las personas con ingresos más bajos, a menudo de minorías, tienen más probabilidades de estar cubiertas por Medicaid o por seguros limitados que no tienen esta cobertura.
If You’re Poor, Fertility Treatment Can Be Out of Reach
For low-income people who are on Medicaid or whose employer health plan is skimpy, help for infertility seems unattainable.
Brote de sarampión: Florida dice que niños no vacunados pueden ir a la escuela, desafiando a los CDC
La mayoría de las personas que no están protegidas por una vacuna contraerán sarampión si se exponen al virus. Existe riesgo de muerte.
The state’s surgeon general grants parents permission to send unvaccinated children to school during a measles outbreak, risking their health and that of others.
Lawsuits Claim South Carolina Kids Underwent Unnecessary Genital Exams During Abuse Investigations
Lawsuits allege that several children under 18 in South Carolina have undergone examinations of their private parts during child abuse investigations — even when there were no allegations of sexual abuse. There’s a growing consensus in medicine that genital exams can be embarrassing, uncomfortable, and even traumatic.
Patients See First Savings From Biden’s Drug Price Push, as Pharma Lines Up Its Lawyers
A restructuring of the Medicare drug benefit has wiped out big drug bills for people who need expensive medicines. But the legal battle over drug negotiations means uncertainty over long-term savings.