Latest KFF Health News Stories
Medicare Fines for High Hospital Readmissions Drop, but Nearly 2,300 Facilities Are Still Penalized
Federal officials said they are penalizing 2,273 hospitals, the fewest since the fiscal year that ended in September 2014. Driving the decline was a change in the formula to compensate for the chaos caused by the covid-19 pandemic.
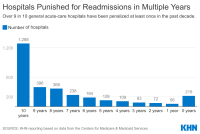
Few Acute Care Hospitals Escaped Readmissions Penalties
More than 9 in 10 general acute-care hospitals have been penalized at least once in the past decade.
Medicare Punishes 2,499 Hospitals for High Readmissions
The federal government’s hospital penalty program finishes its first decade by lowering payments to nearly half the nation’s hospitals for readmitting too many Medicare patients within a month. Penalties, though often small, are credited with helping reduce the number of patients returning for another Medicare stay within 30 days.
Medicare Fines Half of Hospitals for Readmitting Too Many Patients
The penalties are the ninth round of a program created as part of the Affordable Care Act’s broader effort to improve quality and lower costs. The average reduction in federal payments is 0.69%, with 613 hospitals receiving a penalty of 1% or more.
New Round of Medicare Readmission Penalties Hits 2,583 Hospitals
Starting today, Medicare is keeping half a billion dollars in payments from 83% of general hospitals for having too many patients come back.
How Helping Patients Get Good Care At Home Helps Rural Hospitals Survive
Hospitals are now financially rewarded by insurers for safety and efficacy — which often results in patients spending less time as inpatients.
Look-Up: Medicare’s Bonuses And Penalties For Nursing Homes Near You
The federal government is issuing bonuses and penalties to skilled nursing facilities based on how often their patients are readmitted to hospitals within a month of being discharged.
Medicare alivia sanciones por readmisiones en centros con pacientes de bajos ingresos
Siguiendo órdenes del Congreso, Medicare está aliviando sus multas anuales por readmisión en cientos de hospitales que brindan servicios a residentes de bajos ingresos.
Medicare Eases Readmission Penalties Against Safety-Net Hospitals
Penalties will total $566 million for all hospitals. But many that serve a large share of low-income patients will lose less money than they did in previous years.
Your Plumber Offers A Money-Back Guarantee. Should Your Doctor?
Even though consumers don’t expect to pay for faulty service or goods, they are often forced to pay for bad health care. But a small number of hospitals and doctors are seeking to change that practice.
Quiz: How Well Are You Paying Attention?
To strengthen your core knowledge of health care policy, it helps to be a regular reader of Kaiser Health News. Here’s a pop quiz to gauge what you have learned.
Under Trump, Hospitals Face Same Penalties Embraced By Obama
Federal records show that 2,573 hospitals around the country will have their Medicare payments reduced because they have too many patients readmitted.
How To Fight For Yourself At The Hospital — And Avoid Readmission
This new column explains what older adults and their families can do to avoid hospital readmission.
Medicare’s Readmission Penalties Hit New High
Medicare will withhold an estimated $528 million in 2017 from more than 2,500 hospitals that have too many patients returning within 30 days.
Study: 30 Percent Of Children’s Readmissions To Hospitals May Be Preventable
In more than three-quarters of the cases that researchers said might have been preventable, factors at the hospital contributed to the child’s return, according to the researchers.
Missouri Hospitals Seek To Focus Readmission Penalties On Patient Poverty
The Missouri Hospital Association objects to the formula for setting the federal penalties because it does not factor in the number of patients who are poor or in bad health. It is seeking to generate consumer interest in the penalties.
Half Of Nation’s Hospitals Fail Again To Escape Medicare’s Readmission Penalties
The fines, in their fourth year, are assessed on hospitals that have patients frequently return and will cost nearly 2,600 hospitals $420 million in total.
Cleveland Hospitals Grapple With Readmission Fines
The Cleveland Clinic, serving mostly insured patients, sees its Medicare fines go down, while fines go up at the city’s hospitals in low-income neighborhoods. The National Quality Forum is beginning a trial to adjust the program for hospitals that serve more poor people.
Health-Law Test To Cut Readmissions Lacks Early Results
Results so far show community agencies haven’t made a big difference in keeping seniors from making return hospital trips. But administration officials say the program has plenty of potential.
Readmissions Penalties By State: Year 3
Medicare evaluated the readmission rates of the nation’s hospitals in determining the third year of penalties in the Hospital Readmissions Reduction Program. This table lists the average impact on hospitals in each state.