Latest KFF Health News Stories
Deciden bajar sus salarios para poder tener seguro a través del Obamacare
Para este matrimonio de Tennessee, la diferencia de salario significó tener una prima de $87, frente a una anterior de $2,100.
Middle-Class Earners Weigh Love And Money To Curb Obamacare Premiums
Ineligible for subsidies, a Tennessee woman quit her job to get an affordable health care premium. Conventional steps — such as maxing out your 401(k) contribution each year — may also do the job, financial planners say.
Podcast: ‘What The Health?’ We Have Numbers!
In this episode of “What the Health?” Julie Rovner of Kaiser Health News, Sarah Kliff of Vox.com, Joanne Kenen of Politico and Alice Ollstein of Talking Points Memo discuss the first days of open enrollment for 2018 individual health insurance plans and whether the Democratic gains in Tuesday’s off-off-year elections will have any impact on health care policy in Washington, D.C.
Obamacare: comprar seguro es más complicado que nunca. Aquí, algunas tretas
Es esencial que conozca sus opciones en base a los ingresos y al tamaño de su familia. Aquí, algunas respuestas clave para entender el mercado de seguros.
Obamacare Shopping Is Trickier Than Ever. Here’s A Cheat Sheet.
This year, more than ever, it is important to know your options.
Rising Health Insurance Costs Frighten Some Early Retirees
Higher premiums loom for Americans in their late 50s and early 60s who are still too young for Medicare and don’t qualify for subsidies under Obamacare.
Obamacare: 5 nuevas cosas que debes saber
El período abierto de inscripción para las personas que compran su propio seguro de salud ya está en marcha, y termina el 15 de diciembre de 2017. Estos son cinco factores para tener en cuenta.
5 Things To Know About ACA At Year 5
This year’s Obamacare open enrollment will be marked by a number of changes. KHN helps you navigate them.
Podcast: ‘What The Health?’ Open Enrollment is Nigh
In this episode of “What the Health?” Julie Rovner of Kaiser Health News, Margot Sanger-Katz of The New York Times, Sarah Kliff of Vox.com and Alice Ollstein of Talking Points Memo discuss this year’s open enrollment for individual health insurance that starts Nov. 1. And Rovner interviews Lori Lodes, a former Obama administration health official and founder of the new group “Get Covered America.” Plus, for “extra credit,” the panelists recommend their favorite health stories of the week.
Federal Judge Denies Bid To Force Feds To Resume ACA Subsidies
U.S. District Judge Vince Chhabria said the vast majority of states have already prepared for the termination of the payments and already devised responses that give consumers better coverage.
2 Senators Reach Deal On A Health Law Fix, But Bringing Congress Along Is Tricky
The bipartisan accord would restore funding for the cost-sharing reductions that President Donald Trump ended last week and would give states more flexibility to devise alternatives for providing and subsidizing health care.
Trump actuando solo: lo que debe saber sobre los cambios a la ley de salud
Las medidas del presidente Donald Trump eliminan los reembolsos a las aseguradoras, pero no los subsidios que permiten a los consumidores pagar sus primas.
Trump Acting Solo: What You Need To Know About Changes To The Health Law
A quick guide to revisions to the cost-sharing subsidies for lower-income marketplace customers and the proposal to add different plans to the market.
Facebook Live: Trump Ends Payments For Cost-Sharing Reductions. What’s Next?
In this Facebook Live chat, KHN’s Jay Hancock answers questions about President Donald Trump’s announcement that he will end federal payments for the Affordable Care Act’s cost-sharing reductions.
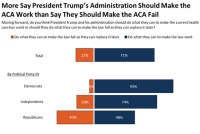
While Trump Moves To Dismantle Health Law, Public Favors Repair
Nearly three-quarters of Americans would like to see the administration focus on efforts on making the Affordable Care Act work, rather than trying to make it fail.
Podcast: ‘What The Health?’ Let’s Blow It Up
In this episode of “What the Health?” Julie Rovner of Kaiser Health News, Margot Sanger-Katz of The New York Times, Sarah Kliff of Vox and Julie Appleby of Kaiser Health News discuss the Trump administration’s latest efforts to undermine the individual insurance market.
California Slaps Surcharge On ACA Plans As Trump Remains Coy On Subsidies
Covered California authorized a 12.4 percent average surcharge on silver-tier plans, the second-least expensive option sold on the exchange. It brings the total average premium increase on those plans to nearly 25 percent next year.
Sen. Collins Announces Opposition To GOP Bill To Replace Obamacare
The statement from the Maine senator came after the Congressional Budget Office said the bill would cause millions of people to become uninsured.
Podcast: ‘What The Health?’ Why Is It So Difficult To Control Drug Prices?
In this episode of “What the Health?” Mary Agnes Carey of Kaiser Health News, Sarah Karlin-Smith of Politico, Margot Sanger-Katz of The New York Times and Julie Appleby of Kaiser Health News discuss the recent extension of cost-sharing subsidies for millions of low-income beneficiaries on the Affordable Care Act’s marketplaces and the state of play on Capitol Hill and in the states concerning initiatives to lower prescription drug costs.
Despite Insurers’ Tactical Win On ACA’s Cost-Sharing Payments, Uncertainty Lingers
Court allows state attorneys general to join a pending legal challenge to keep billions in subsidies flowing to consumers and insurers, despite the Trump administration’s resistance.