Every week, Kaiser Health News reporter Jessica Marcy selects interesting reading from around the Web.
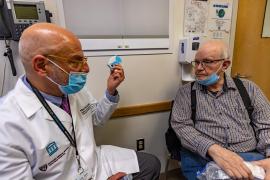
Time: Your Doctor’s Bedside Manner Could Affect Your Health
Even if your doctor doesn’t have the best beside manner, you’re probably willing to excuse her behavior as long as she treats your condition and makes you healthy again, right? Well, you might not want to be so forgiving. It turns out that rudeness and incivility among doctors, in particular in the operating room, can actually lead to poorer health outcomes and even higher death rates among patients. Dr. Andrew Klein, director of (the) comprehensive transplant center at Cedars Sinai in Los Angeles, and his colleague Pier Forni, founder of the Johns Hopkins Civility Project at Johns Hopkins University, collected data on previous studies of surgeons’ behavior in the operating room and the subsequent outcomes of the patients on whom they performed procedures. They found that when doctors were more courteous to operating room staff, their patients were more likely to survive and avoid complications than the patients of docs who were O.R. boors (Alice Park, 7/19).
Columbia Journalism Review: A Shout Out To The Palm Beach Post
The Palm Beach Post deserves kudos for exposing how Florida governor Rick Scott conducted the business of his urgent care clinics in the state, and what his actions reveal for health care to come. Scott is something of health care’s bad boy, having gotten into trouble running Columbia/ HCA, the giant for-profit hospital chain owned by the Frist family of Tennessee. That’s Frist as in former Sen. Majority Leader Bill Frist. In the late 1990s, the FBI uncovered a Medicare billing fraud scheme involving Columbia hospitals. Columbia later settled the case and paid a fine. Two execs went to jail, and Scott got millions in walking away money. Post health and science reporter Stacy Singer discovered that the same practices Scott pushed at Columbia—bottom-line, bonus-focused management that encouraged a culture of cheating—were deployed at his Solantic Urgent Care clinics, which have just been sold to a New York private equity firm. Using the old-fashioned reporting technique of plowing through government documents, Singer revealed the aggressive, profit-first strategy that guided the management of the clinics (Trudy Lieberman, 7/20).
Rolling Stone: Linked Birth Defects: Coal Industry Blames … Inbreeding
A few weeks ago, we posted about a new study linking mountaintop removal coal mining with increased incidence of birth defects. The study by researchers at West Virginia University examined two million health records in Appalachia and concluded that kids born near mountaintop mining operations suffered higher rates of a variety of central nervous system, musculoskeletal, urogenital and circulatory and respiratory problems. Well, over at Coal Tattoo, Ken Ward Jr. unearthed an internet posting from a group of coal industry lawyers that attempts to discredit the study by charging that researchers left out a very important cause of birth defects in Appalachia: consanguinity. Which is a fancy term for inbreeding (Jeff Goodell, 7/12).
Huffington Post: Michele Bachmann’s Migraines: Sexism And Stigma Rage On
It used to be that Americans wondered if a woman could be taken seriously as a presidential candidate. They also questioned if modern society would ever elect someone who’s been divorced. … So what’s the new roadblock du jour? Migraines. Roughly 36 million Americans suffer from this neurological condition — including about 18 percent of women. And candidate Michele Bachmann is one of them. (In full disclosure, so am I.) And, now, her politics aside, critics are seriously questioning whether this one factor is enough to disqualify her from the pursuing the presidency (Laura Schocker, 7/20).
American Medical News: When Doctors And Patients Have The Same Disease
Now a neurologist, Dr. (Brien) Smith says his experiences growing up with epilepsy help him relate to patients with the disorder. … Despite years, and sometimes decades, of study, most physicians spend their careers as outside observers of their patients’ maladies. But in some cases, physicians have experienced the diseases or disorders they treat. Being both physician and patient has its benefits when it comes to relating to patients, said William Shaffer, MD, a neurologist at North Colorado Medical Center in Greeley, Colo. Dr. Shaffer was diagnosed with multiple sclerosis during his second year of medical school and now specializes in treating patients with MS. Having the disease helps him connect with patients (Carolyne Krupa, 7/18).