Latest KFF Health News Stories
Hospitals Cash In on a Private Equity-Backed Trend: Concierge Physician Care
Hospitals are increasingly stretching a velvet rope, offering “concierge service” to an affluent clientele. Critics say the practice exacerbates primary care shortages.
A State-Sanctioned Hospital Monopoly Raises Concerns
The Federal Trade Commission has long argued that competition makes the economy better. But some states have stopped the agency from blocking hospital mergers that create local or regional monopolies, and the results have been messy. Two dozen states have at some point passed controversial legislation waiving anti-monopoly laws, allowing rival hospitals to merge and replacing competition […]
After Appalachian Hospitals Merged Into a Monopoly, Their ERs Slowed to a Crawl
Ballad Health was granted the nation’s largest state-sanctioned hospital monopoly in 2018. Since then, its emergency rooms have become more than three times as slow.
Concerns Grow Over Quality of Care as Investor Groups Buy Not-for-Profit Nursing Homes
For-profit groups own more than 70% of U.S. nursing homes. Industry leaders and researchers wonder whether corporations and investors can succeed where not-for-profit organizations have struggled. Or, will quality of care suffer in the name of making money?
Operating in the Red: Half of Rural Hospitals Lose Money, as Many Cut Services
A recent report finds half of America’s rural hospitals are losing money, and many are struggling to stay open. Researchers and advocates worry the hospitals’ financial spiral will have immediate and long-term health effects on their communities.
The FTC Is Attacking Drugmakers’ ‘Patent Thickets’
It’s a big job clearing out so-called “patent thickets” drugmakers create to keep their products’ prices high. But the Federal Trade Commission is giving it a shot.
Senate Probes the Cost of Assisted Living and Its Burden on American Families
In the wake of a KFF Health News-New York Times series, members of the Special Committee on Aging are asking residents and their families to submit their bills and are calling for a Government Accountability Office study.
The Colonoscopies Were Free. But the ‘Surgical Trays’ Came With $600 Price Tags.
Health providers may bill however they choose — including in ways that could leave patients with unexpected bills for “free” care. Routine preventive care saddled an Illinois couple with his-and-her bills for “surgical trays.”
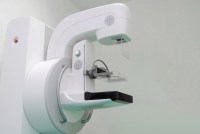
Mamografías que usan inteligencia artificial cuestan dinero extra… pero, ¿vale la pena?
Este software puede identificar patrones y anomalías que los radiólogos humanos podrían pasar por alto. Pero no es el estándar de atención.
Mammography AI Can Cost Patients Extra. Is It Worth It?
Artificial intelligence software to aid radiologists in detecting problems or diagnosing cancer has been moving rapidly into clinical use, where it shows great promise. But it’s a turnoff for some patients asked to pay out-of-pocket for technology that’s not quite ready for prime time.
From Hospital to Hospitality: Spin Doctors Brand Getting Sick as an Adventure. It’s Not.
At $1,000 a night for a private room, medical centers are offering fancy food and casting health care as a “journey.” Instead of creature comforts, how about helping us feel better?
Why Do We Pay For so Much Worthless Health Care?
Medical advances are expensive. Take Wegovy, the wildly successful obesity drug that we learned last week may also reduce the risk of heart disease. If just 10 percent of Medicare beneficiaries start taking the drug, taxpayers could be on the hook for nearly $27 billion a year. So how can the country afford the latest […]
Compensation Is Key to Fixing Primary Care Shortage
Many proposals have been floated about how to address the nation’s primary care problem. They range from training slots to medical school debt forgiveness but often sidestep comprehensive payment reform.
Biden Administration’s Limit on Drug Industry Middlemen Backfires, Pharmacists Say
A rule taking effect Jan. 1 was intended to stop one set of abuses by pharmacy benefit managers, or PBMs, but some pharmacists say it’s enabling these price brokers to simply do new things unfairly.
Facing Criticism, Feds Award First Maternal Health Grant to a Predominantly Black Rural Area
Mississippi has the highest rate of maternal mortality in the U.S. Now, it also has a federal grant to help in rural areas. The award could signal more flexibility from federal officials.
These Appalachia Hospitals Made Big Promises to Gain a Monopoly. They’re Failing to Deliver.
Ballad Health, the only hospital system across a large swath of Tennessee and Virginia, has fallen short of quality-of-care and charity care obligations — even as it’s sued thousands of patients for unpaid bills.
Biden Administration to Ban Medical Debt From Americans’ Credit Scores
The White House said the Consumer Financial Protection Bureau will develop new regulations that would prevent unpaid medical bills from being counted on credit reports.
Your Exorbitant Medical Bill, Brought to You by the Latest Hospital Merger
After decades of unchecked mergers, health care is the land of giants, with huge medical systems monopolizing care in many cities, states, and even whole regions of the country. This decreases patient choice, impedes innovation, erodes quality of care, and raises prices. And federal regulators have been slow to act.
Look Up Your Hospital: Is It Being Penalized by Medicare?
Each year, Medicare punishes hospitals that have high rates of readmissions and high rates of infections and patient injuries. Check out which hospitals have been penalized.
Be Aware: Someone Could Steal Your Medical Records and Bill You for Their Care
Consumers should know that this type of fraud can happen, whether from a large-scale breach or theft of an individual’s data. The result could be thousands of dollars in medical bills.