The Burden of Getting Medical Care Can Exhaust Older Patients
It’s estimated that an older patient can spend three weeks of the year getting care — and that doesn’t count the time it takes to arrange appointments or deal with insurance companies.
Adultos mayores, agotados por tener que organizar tanta atención médica
Un nuevo estudio revela que los pacientes de Medicare dedican aproximadamente tres semanas al año a hacerse pruebas médicas, ver a doctores, someterse a tratamientos o procedimientos médicos, o pasar tiempo en el hospital o en centros de rehabilitación.
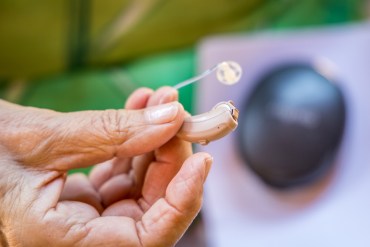
Say That Again: Using Hearing Aids Can Be Frustrating for Older Adults, but Necessary
Hearing loss is more than a nuisance. It also raises the risk of cognitive decline, dementia, falls, depression, and social isolation.
Do We Simply Not Care About Old People?
Recently, thousands of older Americans have been dying weekly of covid. But most Americans aren’t wearing masks in public, a move that could prevent infections. Many at-risk seniors aren’t getting antiviral therapies, and older adults in nursing homes aren’t getting vaccines. Why?
Preparing to Hang Up the Car Keys as We Age
As cognitive skills erode with age, driving skills weaken, but an aging driver may not recognize that. Advance directives on driving are one way to handle this challenge.
America’s Health System Isn’t Ready for the Surge of Seniors With Disabilities
More than a third of older adults have a disability. Many find it difficult to get the medical care they need. New federal regulations would address that problem.
Coping with disability — and the cost of coping with disability — is an enormously important issue for older adults. Nora Super, an expert on aging, shares her personal story.
Who Will Care for Older Adults? We’ve Plenty of Know-How but Too Few Specialists
The principles and practices of geriatrics are being widely disseminated. And we understand much more now about how to improve older adults’ care. Yet we don’t have enough geriatricians to meet the growing demand.
Medicare Expands the Roster of Available Mental Health Professionals
Medicare is expanding access to mental health counselors and marriage and family therapists come Jan. 1. But the belief that seniors who suffer from mental health problems should just grin and bear it remains a troubling barrier to care.
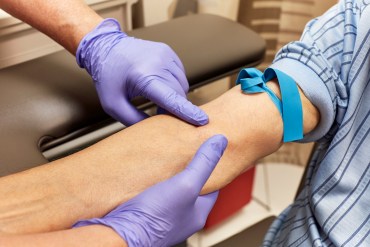
Doubts Abound About a New Alzheimer’s Blood Test
Quest Diagnostics is selling a blood test online to consumers. But results may not be reliable or easy to interpret. And it isn’t covered by insurance.
Let’s Have an Honest Conversation About What to Expect as You Age
A leading geriatrician says a lot of health information for older adults isn’t as useful as it should be. No person’s aging process looks exactly like another’s. So she’s written a guidebook.
Una charla necesaria: qué le ocurre al cuerpo y la mente a medida que se envejece
El envejecimiento altera a las personas por décadas, un largo período influenciado por circunstancias sociales y económicas, conductas, el lugar en donde se vive, y otros factores. E impacta en la fisiología, pero no de manera uniforme para todos.
A New Medicare Proposal Would Cover Training for Family Caregivers
The federal government is proposing having Medicare pay professionals to train family caregivers how to perform tasks like bathing and dressing their loved ones, and properly use medical equipment.
New Alzheimer’s Drug Raises Hopes — Along With Questions
Clinics serving Alzheimer’s patients are working out the details of who will get treated with the new drug Leqembi. It won’t be for everyone with memory-loss symptoms.
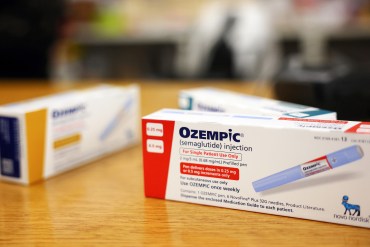
New Weight Loss Drugs Carry High Price Tags and Lots of Questions for Seniors
Although nearly 40% of Americans 60 and older are obese, Medicare doesn’t cover weight loss medications. Meanwhile, studies haven’t thoroughly examined new drugs’ impact on older adults.
In Older Adults, a Little Excess Weight Isn’t Such a Bad Thing
Researchers have found that while obesity at any age risks harming health, a few extra pounds in later life isn’t cause for concern.
How to Negotiate With Resistant Aging Parents? Borrow These Tips From the Business World
Negotiation techniques can help health care providers and family caregivers find common ground with older adults who resist advice or support.
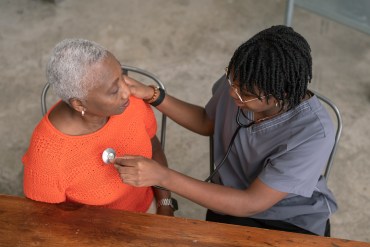
Cardiovascular Disease Is Primed to Kill More Older Adults, Especially Blacks and Hispanics
Cardiovascular disease is the biggest killer of older Americans, with Black and Hispanic people at higher risk. Despite medical advances, researchers say, disparities are expected to worsen in the coming decades.
When Older Parents Resist Help or Advice, Use These Tips to Cope
Dealing with a stubborn or resistant older parent can be a difficult problem for adult children. Family caregivers and professionals have some hard-won lessons on how to manage these evolving relationships.
Tips para ayudar a los padres mayores que se resisten a recibir ayuda o consejos
Lidiar con un padre mayor que se resiste obstinadamente a aceptar ayuda no es fácil. Pero la solución no es que los padres sientan que se está pasando por encima de ellos, tomando el control de sus asuntos.